What age does macular degeneration start? This crucial question unlocks a complex understanding of this vision-threatening condition. Macular degeneration, a progressive eye disease, can rob individuals of sharp central vision. Understanding its onset, types (like wet and dry), and risk factors is essential for prevention and early detection. We’ll explore the variability in age of onset, delving into genetic predispositions, environmental influences, and the role of lifestyle choices.
This journey will illuminate the factors contributing to the development of macular degeneration and equip you with valuable insights for maintaining healthy vision throughout life.
From the initial stages of the disease to the eventual impact on daily life, this comprehensive guide will equip you with the knowledge to navigate the complexities of macular degeneration. The following sections will unravel the intricacies of its onset, the variability of age, and how various factors contribute to its development. We’ll also explore available treatment options and the importance of early detection.
Prepare to gain a profound understanding of this critical eye condition.
Introduction to Macular Degeneration: What Age Does Macular Degeneration Start
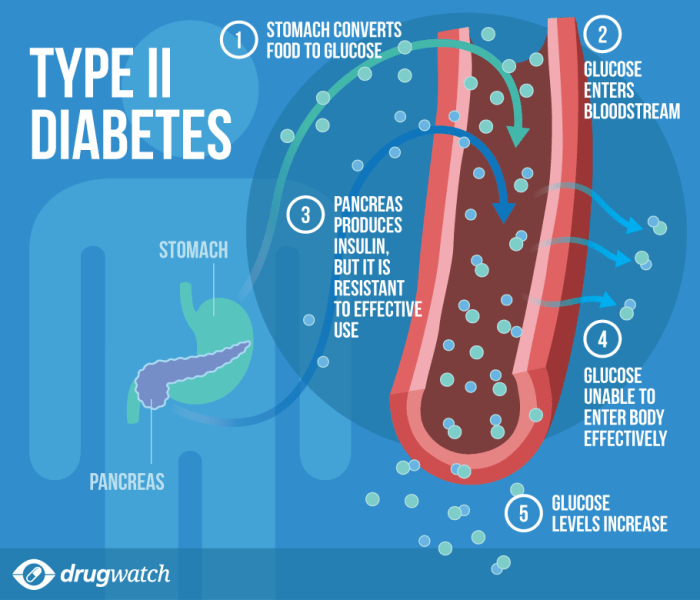
Macular degeneration is a progressive eye disease that affects the macula, the central part of the retina responsible for sharp, detailed vision. This crucial area of the eye is essential for tasks like reading, driving, and recognizing faces. When the macula deteriorates, the ability to see fine details and colors diminishes significantly. This gradual loss of central vision can drastically impact a person’s quality of life, making everyday activities challenging.Macular degeneration exists in two primary forms: wet and dry.
Macular degeneration, unfortunately, can start showing up at any age, though it’s more common in older adults. While focusing on healthy habits like a balanced diet is crucial for overall eye health, and considering things like foods to avoid on Ozempic like this , it’s important to remember that genetic predisposition and lifestyle choices can influence when and how it develops.
So, while you can’t predict the exact age, maintaining good eye health throughout life is always a good strategy.
Dry macular degeneration, the more common type, involves a gradual thinning of the macula. Wet macular degeneration, while less prevalent, is more aggressive and involves abnormal blood vessel growth under the macula, leading to leakage and scarring. Both forms result in vision loss, though the mechanisms and progression differ.Several factors increase the risk of developing macular degeneration.
Age is a significant risk factor, with the prevalence increasing dramatically after the age of 50. Genetics also plays a role; individuals with a family history of macular degeneration are at a higher risk. Smoking, a diet deficient in certain nutrients (like antioxidants), and a history of cardiovascular disease are also associated with an increased likelihood of developing the condition.
Types of Macular Degeneration and Associated Symptoms
Different types of macular degeneration present with distinct symptoms, and the rate of progression can vary. Understanding these differences is crucial for early diagnosis and appropriate management.
| Type of Macular Degeneration | Common Symptoms | Approximate Age of Onset |
|---|---|---|
| Dry Macular Degeneration | Blurred central vision, distortion of straight lines, gradual loss of central vision, difficulty reading fine print, and reduced color perception. | Typically after 50, but can occur earlier in some cases. |
| Wet Macular Degeneration | Sudden vision loss, distorted or blurry central vision, straight lines appearing wavy, and a sudden decrease in color perception. | Typically after 50, but can occur earlier in some cases, often after dry MD. |
Note: The age of onset is an approximation. Individual experiences can vary significantly. Early diagnosis and management can help maintain vision and slow progression in most cases.
Age of Onset Variability

Macular degeneration, a leading cause of vision loss in older adults, isn’t a uniform experience. The age at which it manifests can vary significantly, impacting individuals differently and requiring tailored management strategies. Understanding this variability is crucial for early detection and proactive interventions.The range of ages at which macular degeneration appears highlights the complexity of this condition. While the typical onset is in later adulthood, individuals can experience the disease much earlier in life.
This age disparity is due to a combination of genetic predispositions, environmental factors, and lifestyle choices.
Typical Age of Onset for Different Types
Age-related macular degeneration (AMD) typically presents in individuals over the age of 50, but the exact age of onset can vary based on the specific type. Dry AMD, the more common form, usually appears later than wet AMD. Wet AMD, characterized by the abnormal growth of blood vessels, tends to manifest at a somewhat earlier age than dry AMD, though this isn’t always the case.
Furthermore, other less common forms of macular degeneration may have different typical age ranges, necessitating individualized assessment.
Examples of Early Onset
While less common, macular degeneration can emerge in individuals younger than the typical age of 50. Some individuals with a strong family history of AMD might develop symptoms earlier. Certain genetic mutations can significantly increase the risk of early-onset macular degeneration, even in those under 40. Additionally, certain lifestyle factors, such as prolonged exposure to intense sunlight or specific medical conditions, might also play a role.
An example of early onset would be an individual diagnosed with wet AMD in their 30s due to a family history of the condition.
Factors Contributing to Age Variation
Several factors can influence the age at which macular degeneration develops. These factors interact in complex ways, and the precise contribution of each can vary from person to person.
| Factor | Description | Impact on Onset |
|---|---|---|
| Genetics | Inherited predisposition to the condition, including specific gene mutations. | Can significantly accelerate or delay the onset, particularly in cases with strong family history. |
| Lifestyle Factors | Dietary habits, smoking, exposure to sunlight, and overall health conditions. | Poor lifestyle choices can increase the risk and potentially lead to earlier onset. |
| Environmental Factors | Exposure to environmental toxins, pollution, and certain dietary deficiencies. | Exposure to harmful substances can negatively affect retinal health, potentially accelerating macular degeneration. |
| Underlying Medical Conditions | Conditions such as diabetes, high blood pressure, and high cholesterol. | Certain pre-existing health problems can increase the risk of macular degeneration and potentially accelerate its onset. |
| Age | The most significant risk factor, but not a predictor for onset in all cases. | Generally associated with increased risk as the population ages. |
Genetic Predisposition and Macular Degeneration
Genetics plays a significant role in determining an individual’s susceptibility to macular degeneration. While age remains the most significant risk factor, inherited variations in genes can influence the likelihood of developing the condition and, importantly, the age at which it might manifest. Understanding these genetic influences is crucial for identifying individuals at higher risk and potentially developing preventative strategies.The complex interplay between genetic predisposition and environmental factors dictates the development of macular degeneration.
Environmental factors, such as smoking, diet, and exposure to sunlight, can influence the progression of the disease in individuals with a genetic predisposition. Conversely, individuals without a genetic predisposition might still develop the condition due to significant environmental factors, although the age of onset might be later. This interplay highlights the importance of both genetic and environmental factors in understanding the disease.
Specific Genes Associated with Risk
Several genes have been linked to an increased risk of macular degeneration. Research continues to uncover new associations, adding to our understanding of the genetic basis of the disease. This intricate genetic landscape suggests that multiple genes contribute to the overall risk.
Genetic Mutations and Age of Onset
While a precise correlation between specific genetic mutations and exact age of onset is often elusive, some patterns emerge. The presence of certain genetic mutations may lead to earlier-onset disease in some individuals compared to those without such mutations. The influence of other genetic variations and environmental factors can significantly modify the expected age of onset.
Macular degeneration, a common eye condition, can start showing up at various ages, but it’s often more prevalent in older adults. While exploring different ways to manage eye health is important, it’s also crucial to consider support options like mobility aids with fibromyalgia if you or someone you know has fibromyalgia. The age of onset for macular degeneration is often associated with factors like genetics and lifestyle, so it’s a complex issue.
Ultimately, maintaining a healthy lifestyle and getting regular eye checkups are key to detecting and managing the condition.
| Genetic Mutation | Approximate Age of Onset (Example) | Description |
|---|---|---|
| CFH gene mutations | 50-60s (often earlier in those with family history) | The CFH gene is strongly associated with age-related macular degeneration. Mutations in this gene lead to a greater risk of the condition. The exact age of onset varies significantly, depending on the specific mutation and other contributing factors. |
| ARMS2 gene mutations | 40-50s (often earlier in those with family history) | Mutations in the ARMS2 gene are also implicated in a heightened risk of macular degeneration. The age of onset, like in CFH, is not fixed and can vary based on individual factors. |
| TIMP3 gene mutations | 60-70s (may be earlier in individuals with other risk factors) | The TIMP3 gene is involved in regulating the extracellular matrix. Mutations in this gene can increase the risk of macular degeneration. The observed age of onset, like in the other genes, is a general estimate. |
Note: The ages presented in the table are approximations and can vary significantly. Individual experiences are influenced by numerous genetic and environmental factors.
Interaction Between Genetics and Environment
The relationship between genetic predisposition and environmental factors is complex. Individuals with a strong genetic predisposition might experience earlier onset and more rapid progression of the disease if exposed to environmental risk factors. Conversely, individuals without a strong genetic predisposition might still develop macular degeneration if environmental factors are severe enough. This highlights the combined impact of these factors on the disease’s progression.
Macular degeneration, a common eye condition, can start to affect vision at various ages, though it’s more prevalent in older individuals. Factors like genetics and lifestyle play a role, but maintaining a healthy red blood cell rbc count here might contribute to overall eye health, potentially delaying the onset of age-related macular degeneration. Ultimately, the precise age of onset varies significantly from person to person.
Environmental Influences
Environmental factors play a significant role in the development and progression of age-related macular degeneration (AMD). While genetics are a strong predictor, external influences can either exacerbate or mitigate the risk of AMD, potentially affecting the age of onset. Understanding these influences is crucial for developing preventative strategies and personalized approaches to managing the disease.
Environmental Exposures Potentially Linked to AMD
Environmental exposures, such as sunlight, smoking, diet, and certain infections, have shown a correlation with AMD. Sunlight, with its ultraviolet (UV) radiation, is believed to damage the retina over time, potentially contributing to AMD development. Similarly, exposure to certain pollutants in the air or water may also play a role. Smoking is a well-established risk factor, its impact on oxidative stress and inflammation likely contributing to the disease’s progression.
A diet deficient in certain nutrients, or high in saturated fats, may also influence AMD development.
Potential Mechanisms of Environmental Impact
Environmental factors likely influence AMD through various mechanisms. Oxidative stress, the imbalance between free radicals and antioxidant defenses, is a key player. Exposure to UV radiation, air pollutants, and even certain dietary choices can increase oxidative stress in the eye. This stress can damage retinal cells, potentially accelerating the degeneration process. Inflammation is another critical factor.
Chronic low-grade inflammation in the eye, induced by various environmental exposures, may lead to the breakdown of retinal tissues. Smoking, for example, directly contributes to inflammation and increases oxidative stress, creating a double-edged risk factor for AMD.
Impact of Different Environmental Factors
The impact of different environmental factors on the age of onset of AMD can vary. While some factors, like smoking, have a consistently strong correlation with earlier onset, others, like diet, might have a more nuanced impact, depending on the specific dietary choices and overall health. Factors such as UV exposure can increase the risk of AMD, but the degree of impact depends on the duration and intensity of the exposure.
The influence of environmental factors is not always direct or predictable. Interactions between genetic predispositions and environmental factors can significantly alter the age of onset and disease progression.
Comparison of Environmental Factors’ Impact on Age of Onset
| Environmental Factor | Approximate Impact on Age of Onset (Note: This is a rough estimate and can vary greatly based on individual factors.) |
|---|---|
| Smoking | Potentially accelerates onset by several years. |
| High UV Exposure | May contribute to earlier onset, particularly in individuals with genetic predisposition. |
| Poor Diet (High in Saturated Fats, Low in Antioxidants) | Potentially accelerates onset by several years, primarily by increasing oxidative stress. |
| Air Pollution | Potentially increases risk, but the effect on onset age is less clear compared to other factors. |
| Certain Infections | Possible association with earlier onset, but more research is needed. |
Note: The table above provides a general overview. Individual responses to environmental factors can vary significantly due to genetic predisposition, lifestyle, and other factors.
Lifestyle and Age of Onset

Our lifestyle choices play a significant role in the development and progression of macular degeneration. While genetics and environmental factors are influential, the decisions we make daily can impact when and how severely this condition manifests. Understanding these connections is crucial for proactive measures to safeguard eye health.Maintaining a healthy lifestyle can delay the onset of macular degeneration or slow its progression.
This involves adopting a balanced diet, regular exercise, and avoiding harmful habits like smoking. The impact of these choices on the disease’s trajectory is substantial, and understanding how they interact with the genetic predisposition is key to personalized strategies for prevention.
Diet’s Impact on Macular Degeneration
A balanced diet rich in antioxidants and essential nutrients is crucial for maintaining overall health, including eye health. Vitamins like lutein and zeaxanthin, found in leafy greens, are particularly beneficial for protecting the macula. Studies suggest that diets high in fruits, vegetables, and omega-3 fatty acids may contribute to delaying the onset and slowing the progression of macular degeneration.
Conversely, diets high in saturated fats and processed foods might have an adverse effect. The specific nutrients that impact macular degeneration are still under investigation.
Exercise and Macular Degeneration
Regular physical activity is beneficial for overall health and may also play a role in protecting against macular degeneration. Exercise improves blood circulation, delivering essential nutrients to the eyes and potentially reducing inflammation. The exact mechanisms through which exercise influences macular degeneration are not fully understood, but evidence suggests a positive correlation between physical activity and reduced risk.
For instance, a study found a lower incidence of macular degeneration in individuals who consistently engaged in moderate-intensity exercise.
Smoking and Macular Degeneration
Smoking significantly increases the risk of developing macular degeneration. The harmful chemicals in tobacco smoke damage blood vessels, impairing the delivery of nutrients to the eyes and potentially leading to accelerated macular degeneration. Individuals who smoke are more likely to experience a faster progression of the disease, resulting in greater vision loss compared to nonsmokers. Quitting smoking, even at later stages, can still have positive effects on the progression of macular degeneration.
Importance of Regular Eye Exams
Regular eye exams are vital for early detection of macular degeneration. Early diagnosis allows for timely intervention and management strategies, potentially slowing the progression of the disease and preserving vision. Even if there are no apparent symptoms, regular check-ups can identify early signs of macular degeneration. Early detection is essential because treatment options are often more effective when implemented in the initial stages.
Lifestyle Factors Affecting Macular Degeneration
| Factor | Description | Impact on Onset |
|---|---|---|
| Balanced Diet (Fruits, Vegetables, Omega-3s) | High intake of antioxidants and essential nutrients. | Positive |
| Regular Exercise | Maintaining a consistent physical activity routine. | Positive |
| Smoking | Consumption of tobacco products. | Negative |
| Regular Eye Exams | Routine check-ups to monitor eye health. | Positive |
Early Detection and Diagnosis
Catching macular degeneration early is crucial for managing its progression and preserving vision. Early intervention can significantly slow the rate of vision loss, allowing individuals to maintain independence and quality of life. Understanding the early signs and the diagnostic procedures available is key to proactive eye health.Early detection of macular degeneration relies heavily on regular eye exams, coupled with knowledge of potential symptoms.
The process involves identifying subtle changes in vision that might initially go unnoticed. Different age groups may exhibit varying symptoms, and recognizing these differences is essential for prompt diagnosis and treatment.
Recognizing Early Signs
Early signs of macular degeneration may be subtle and easily missed, especially in the initial stages. Individuals may notice a blurring or distortion of central vision, particularly in activities requiring sharp focus like reading or driving. Straight lines might appear wavy, and colors may appear faded or less vibrant. Difficulty distinguishing fine details, such as facial features, is another possible symptom.
Peripheral vision usually remains unaffected initially, which can mask the progression of the disease in its early stages.
Common Diagnostic Procedures, What age does macular degeneration start
Various diagnostic tools and procedures are used to detect macular degeneration. A comprehensive eye exam is the cornerstone of the diagnostic process. This involves evaluating the health of the entire eye, including the retina, optic nerve, and other structures. Detailed visual acuity tests are conducted to assess the sharpness and clarity of vision at different distances. Additional tests may include:
- Amsler Grid Test: This test helps detect distortion or blurring in central vision. The Amsler grid is a grid-like pattern used to measure the clarity and straightness of the lines. Any deviation from the normal grid pattern can be a sign of macular degeneration. This test is often used as a screening tool.
- Optical Coherence Tomography (OCT): OCT uses light waves to create detailed images of the retina, revealing the thickness and structure of the macula. This test can identify any changes or thinning in the macular region, which are indicative of macular degeneration. It can also help distinguish between different types of macular degeneration.
- Fluorescein Angiography: This test involves injecting a dye into the bloodstream and taking pictures of the retinal blood vessels as the dye circulates. It helps to visualize the blood flow within the retina, highlighting any abnormalities that might be present. This can help diagnose macular degeneration by revealing any issues with the blood vessels supplying the macula.
Vision Tests at Different Ages
The approach to vision testing for macular degeneration varies based on the individual’s age. Children and young adults may undergo standard vision tests, similar to those performed for other refractive errors. As individuals age, the frequency and type of tests may increase. Older adults, particularly those with risk factors, might undergo more specialized tests, such as OCT or fluorescein angiography, to detect early signs of the disease.
Regular comprehensive eye exams are essential regardless of age to detect and address any vision changes promptly.
Diagnostic Procedures for Different Age Groups
The diagnostic approach varies depending on the age of the patient. Young individuals often undergo standard vision tests to assess visual acuity and refraction. As people age, the diagnostic process might include more in-depth examinations, such as OCT or fluorescein angiography, to screen for macular degeneration. This tailored approach allows healthcare professionals to adapt their diagnostic strategies to the specific needs of each age group.
Furthermore, family history and risk factors play a crucial role in determining the appropriate diagnostic steps for individuals of different ages.
Treatment Options
Unfortunately, there’s no cure for macular degeneration, but several treatments can help slow its progression and manage symptoms. These approaches aim to preserve vision and improve the quality of life for individuals affected by this condition. The specific treatment plan will depend on the type of macular degeneration, the stage of the disease, and the individual’s overall health.Current treatments primarily focus on slowing the disease’s progression rather than reversing it.
The effectiveness of these treatments can vary significantly, and ongoing research continues to explore new and potentially more effective therapies.
Available Treatment Options
Various treatments are available for managing macular degeneration, each with its own set of benefits and drawbacks. The most common treatments involve medications, lifestyle adjustments, and supportive care.
- Anti-VEGF Medications: These medications, administered through injections into the eye, target vascular endothelial growth factor (VEGF), a protein that contributes to the growth of abnormal blood vessels in the eye. By reducing VEGF levels, these injections can help slow the growth of these problematic vessels, thereby potentially reducing the damage to the macula. For example, ranibizumab (Lucentis) and aflibercept (Eylea) are common anti-VEGF medications used in treating macular degeneration.
- Lifestyle Modifications: While not a cure, adopting a healthy lifestyle can potentially mitigate some risk factors associated with macular degeneration. These lifestyle changes can include maintaining a balanced diet rich in antioxidants and vitamins, regular exercise, and abstaining from smoking. For instance, a diet rich in fruits and vegetables high in antioxidants like lutein and zeaxanthin has shown promise in potentially reducing the risk of the disease.
- Complementary and Alternative Therapies: Some individuals explore complementary and alternative therapies, such as nutritional supplements or specific diets, to potentially mitigate the progression of the disease. However, it’s crucial to consult with a healthcare professional before using these therapies, as their effectiveness has not been rigorously proven and can potentially interact with other medications.
Effectiveness of Treatments
The effectiveness of different treatments for slowing the progression of macular degeneration can vary significantly. Anti-VEGF medications, when administered as prescribed, are often quite effective in slowing the growth of abnormal blood vessels and preserving vision in many cases. However, the response to treatment is not uniform and may vary based on individual factors. Furthermore, treatment effectiveness may decrease over time as the disease progresses.
The response to anti-VEGF medications can be measured through regular ophthalmological examinations.
Treatment Variations
The choice of treatment for macular degeneration will vary based on the type and stage of the disease. Early-stage dry macular degeneration might respond differently to treatment than wet macular degeneration, and the effectiveness of interventions may also differ depending on the specific characteristics of the individual’s condition. For example, a patient with early-stage dry macular degeneration might be more likely to benefit from dietary modifications and lifestyle changes, while a patient with wet macular degeneration might require more aggressive treatments like anti-VEGF injections.
Comparison of Treatment Options
| Treatment Type | Effectiveness | Potential Side Effects |
|---|---|---|
| Anti-VEGF Medications (e.g., Lucentis, Eylea) | Often effective in slowing disease progression, preserving vision, and reducing fluid buildup in the macula. | Eye infections, increased eye pressure, and bleeding in the eye are possible side effects, although they are usually temporary and manageable. |
| Lifestyle Modifications (e.g., diet, exercise, smoking cessation) | While not a cure, these modifications can mitigate some risk factors and improve overall health, which might have a positive impact on the disease’s progression. | No direct side effects associated with these lifestyle modifications, but consistent adherence is crucial. |
| Complementary and Alternative Therapies | Effectiveness is not consistently proven, and interactions with other medications are possible. | Potential side effects are dependent on the specific therapy and should be discussed with a healthcare professional. |
Conclusion
In conclusion, macular degeneration’s onset is a multifaceted issue influenced by a complex interplay of genetic predisposition, environmental factors, and lifestyle choices. While a precise age of onset isn’t always predictable, understanding the contributing factors is crucial for early detection and potential intervention. This exploration has highlighted the significance of genetic testing, environmental awareness, and the importance of proactive lifestyle choices to mitigate risk.
The key takeaway? Maintaining a healthy lifestyle, regular eye exams, and open communication with your eye care professional are paramount in safeguarding your vision.