What is primary ovarian insufficiency? This condition, often affecting women in their reproductive years, can significantly impact their health and well-being. It’s characterized by the premature loss of ovarian function, leading to irregular periods, fertility issues, and other potential health complications. This comprehensive look will explore the various aspects of POI, from its definition and causes to its management and long-term implications.
POI encompasses a spectrum of experiences, from subtle symptoms to more pronounced difficulties. Understanding the stages of ovarian function and how POI fits within this framework is key to comprehending the condition’s diverse manifestations. This exploration will delve into the potential causes of POI, ranging from genetic predispositions to environmental factors, while also highlighting the importance of early diagnosis and personalized treatment approaches.
Definition and Overview
Primary ovarian insufficiency (POI) is a condition characterized by the premature loss of ovarian function in women before the age of 40. This means the ovaries stop producing the hormones needed for normal menstrual cycles and egg development. It’s a significant concern for women of reproductive age, as it can lead to infertility and other health complications.POI differs from menopause, which typically occurs in the 40s and 50s, as it’s an earlier and often unexpected cessation of ovarian function.
It’s important to distinguish POI from other conditions that might share similar symptoms, such as thyroid disorders or polycystic ovary syndrome (PCOS), as the treatment approach will vary. Understanding the stages of ovarian function is crucial for diagnosing and managing POI.
Stages of Ovarian Function
Ovarian function progresses through distinct stages. From puberty, the ovaries develop and release eggs, driven by hormones. The release of these eggs is cyclical and controlled by the hypothalamic-pituitary-ovarian (HPO) axis. POI disrupts this delicate balance, leading to a premature cessation of ovarian function. Different stages include the pre-pubertal phase, the pubertal phase characterized by menarche, and the reproductive phase where ovulation and menstruation occur regularly.
The post-menopausal phase marks the final stage of ovarian function.
Prevalence of POI
The prevalence of POI varies across different populations. Estimates suggest that it affects approximately 1% to 5% of women of reproductive age. Factors like genetics, ethnicity, and environmental influences can potentially play a role in influencing the prevalence rates. However, more research is needed to fully understand these factors.
Impact on Reproductive Health
POI significantly impacts reproductive health, leading to infertility. Women with POI have difficulty conceiving naturally. This is due to the absence of mature eggs needed for fertilization. As a result, assisted reproductive technologies (ARTs) may be necessary for achieving pregnancy. It also impacts the woman’s overall health and well-being due to the hormonal changes and other related health issues.
Comparison of POI with Other Reproductive Conditions, What is primary ovarian insufficiency
| Condition | Symptoms | Diagnosis | Treatment |
|---|---|---|---|
| Primary Ovarian Insufficiency (POI) | Irregular or absent menstrual cycles, infertility, hot flashes, vaginal dryness, mood swings, and fatigue. | Assessment of hormone levels (FSH, LH, estradiol), pelvic ultrasound, and possibly genetic testing. | Hormone replacement therapy (HRT), lifestyle modifications (diet, exercise), and fertility treatments (in cases of infertility). |
| Menopause | Similar to POI, but typically occurring later in life (40s-50s). | Clinical evaluation, including menstrual history and hormone levels. | Hormone replacement therapy (HRT), lifestyle modifications. |
| Polycystic Ovary Syndrome (PCOS) | Irregular periods, acne, hirsutism (excessive hair growth), weight gain, and infertility. | Clinical evaluation, including hormone levels, ultrasound, and possibly blood tests. | Lifestyle modifications, medication to regulate ovulation, and fertility treatments. |
| Hypothalamic Amenorrhea | Absence of menstruation due to dysfunction of the hypothalamus, often related to stress, excessive exercise, or eating disorders. | Detailed history, hormone level assessment, and imaging studies. | Addressing the underlying cause (stress management, weight gain, etc.), hormone therapy, and potentially fertility treatments. |
Causes and Risk Factors
![The Logos | [2025.06.18] The Logos - Yahusha's Message For Laodicea #thelogos #YahushaChrist # ... What is primary ovarian insufficiency](http://lyricapills.com/wp-content/uploads/2025/06/Sbro_Castlehill_Primary_P7B-2_50908002-2219b7mt4-2048x1365-1-1.jpg)
Primary ovarian insufficiency (POI) is a complex condition with a variety of potential underlying causes. While the exact mechanism isn’t always clear, a combination of genetic predisposition and environmental factors likely plays a role in its development. Understanding these factors is crucial for both diagnosis and potential preventative strategies.
Known Causes of POI
A multitude of factors can contribute to the premature ovarian failure characteristic of POI. These range from inherited genetic mutations to environmental exposures, each impacting ovarian function in distinct ways. Recognizing these diverse causes is important for personalized treatment approaches.
Role of Genetic Factors
Genetic predisposition significantly influences the risk of developing POI. Inherited mutations in genes involved in ovarian development, function, and maintenance can lead to premature ovarian failure. This genetic vulnerability interacts with other factors, potentially exacerbating the risk of POI. For instance, women with a family history of POI may have a higher chance of developing the condition themselves.
Environmental Risk Factors
Environmental exposures can also contribute to the development of POI. Factors like exposure to certain chemicals, infections, and even nutritional deficiencies have been linked to premature ovarian aging. However, the precise nature of the link and the extent of the impact remain subjects of ongoing research.
Comparison of Different Causes
The various causes of POI can be compared and contrasted based on their mechanisms. Genetic mutations typically affect the intrinsic function of the ovaries, leading to impaired oocyte production and hormone synthesis. Environmental factors, on the other hand, can exert a more indirect effect, potentially disrupting ovarian function through oxidative stress or other mechanisms. Recognizing these differences is vital in developing targeted interventions.
Hierarchical Structure of POI Causes
Causes of POI can be organized into a hierarchical structure, highlighting the interconnectedness of factors. At the highest level, causes can be categorized as genetic or environmental. Further breakdown would identify specific genetic mutations or environmental exposures, each with varying degrees of impact.
Genetic Mutations Potentially Associated with POI
| Mutation | Gene | Symptoms | Frequency |
|---|---|---|---|
| Specific mutation example (e.g., BRCA1 mutation) | BRCA1 | Early-onset breast cancer, ovarian cancer, increased risk of other cancers | Relatively low frequency (variable depending on ethnicity) |
| Specific mutation example (e.g., FOXL2 mutation) | FOXL2 | Premature ovarian failure, sometimes with other endocrine abnormalities | Moderately low frequency |
| Specific mutation example (e.g., POR mutation) | POR | Premature ovarian failure, sometimes with other metabolic issues | Low frequency |
| Specific mutation example (e.g., ATM mutation) | ATM | Increased risk of various cancers, developmental delays, and immunodeficiency | Low frequency |
This table presents examples of genetic mutations that have been linked to POI. The frequency of each mutation varies, and the specific symptoms can vary based on the exact mutation and affected genes. This table should not be considered exhaustive, and ongoing research continues to identify additional potential genetic links to POI.
Symptoms and Diagnosis
Primary ovarian insufficiency (POI) presents with a diverse range of symptoms, often subtle and variable. Recognizing these symptoms and understanding the diagnostic process is crucial for timely intervention and management. Early diagnosis allows for appropriate treatment strategies, potentially improving reproductive outcomes and overall well-being.Recognizing the signs and symptoms of POI is critical for prompt medical evaluation. A thorough understanding of the diagnostic criteria and the specific tests used is essential for accurate identification of the condition.
This will enable healthcare providers to offer the most effective treatment and support options.
Common Symptoms Experienced by Women with POI
Understanding the range of symptoms associated with POI is essential for early detection. These symptoms can vary significantly from woman to woman, and their severity can fluctuate.Women experiencing POI may exhibit a range of symptoms, including irregular or absent menstrual periods, reduced fertility, and other hormonal imbalances. These symptoms often overlap with other conditions, making accurate diagnosis challenging.
Diagnostic Criteria for POI
The diagnostic criteria for POI revolve around the presence of amenorrhea (absence of menstruation) for at least four consecutive months, along with elevated follicle-stimulating hormone (FSH) levels. This combination of symptoms and laboratory findings is indicative of ovarian dysfunction.The diagnostic criteria for POI are based on the combination of clinical presentation, menstrual history, and laboratory test results. The absence of menstruation for at least four consecutive months, coupled with elevated FSH levels, typically suggests POI.
Role of Diagnostic Tests in Identifying POI
Various diagnostic tests play a crucial role in identifying POI. These tests help evaluate ovarian function and confirm the diagnosis. A combination of tests is usually employed to arrive at a conclusive diagnosis.
- Blood Tests: Blood tests are essential in evaluating hormone levels. These tests measure levels of follicle-stimulating hormone (FSH), luteinizing hormone (LH), and estradiol. Elevated FSH levels, in particular, are a key indicator of POI. Low estradiol levels are often associated with POI. These hormonal imbalances are a crucial element in the diagnostic process.
- Imaging Tests: While not always necessary, imaging tests like ultrasound may be used to assess the ovaries and rule out other potential causes. This can help distinguish between POI and other conditions with similar symptoms.
Common Signs and Symptoms Leading to a Diagnosis of POI
The following are some of the most common signs and symptoms that may lead to a diagnosis of POI.
- Irregular or absent menstrual periods: This is a hallmark symptom, often the first indication of potential POI. The absence of menstruation for extended periods (e.g., four consecutive months) can trigger a referral to a healthcare professional.
- Infertility: Difficulty conceiving or an inability to conceive can be a significant indicator of POI. This symptom, coupled with irregular periods, can prompt further investigation.
- Early menopause symptoms: Symptoms such as hot flashes, night sweats, and vaginal dryness can be indicative of declining ovarian function, and can contribute to a diagnosis of POI.
Importance of Early Diagnosis for Managing POI
Early diagnosis of POI is crucial for effective management. It allows for timely interventions to address the hormonal imbalances and associated symptoms. Early diagnosis also facilitates reproductive options, if desired.
Primary ovarian insufficiency (POI) is a condition where a woman’s ovaries stop working properly before the age of 40. It can lead to a range of symptoms, and managing those symptoms can sometimes involve using adjuvant analgesics, which are medications used to enhance the effects of pain relief. Learning more about what these medications are can be helpful for understanding potential treatment options for POI.
what are adjuvant analgesics Ultimately, understanding POI and its various treatment approaches is key to navigating this condition effectively.
Diagnostic Tests for POI
| Test | Purpose | Procedure | Results ||—|—|—|—|| Follicle-stimulating hormone (FSH) | Measures the level of FSH in the blood. | Blood draw. | Elevated FSH levels (typically greater than 30 mIU/mL) in the early follicular phase suggest POI. || Luteinizing hormone (LH) | Measures the level of LH in the blood. | Blood draw.
| Elevated LH levels (often in conjunction with elevated FSH) may indicate ovarian dysfunction. || Estradiol | Measures the level of estradiol in the blood. | Blood draw. | Low estradiol levels are frequently observed in women with POI. || Ultrasound | Evaluates the size and structure of the ovaries.
Primary ovarian insufficiency (POI) is a condition where a woman’s ovaries stop working properly before the age of 40. It can be challenging to manage, and often leads to a need for hormone replacement therapy. Interestingly, similar to POI, diet plays a crucial role in managing other chronic conditions like diet and chronic pancreatitis , highlighting the interconnectedness of various health issues.
Ultimately, understanding the root causes of POI and seeking appropriate medical advice is key to effective management.
| Transvaginal ultrasound. | Reduced ovarian size and/or the presence of ovarian cysts may be observed. |
Management and Treatment
Navigating primary ovarian insufficiency (POI) requires a multifaceted approach that addresses the hormonal imbalances and associated health concerns. Effective management hinges on a combination of therapies, including hormone replacement therapy (HRT), and a focus on overall well-being, including the management of potential comorbidities. This proactive approach can significantly improve quality of life and long-term health outcomes for individuals with POI.
Treatment Options for POI
Managing POI involves a personalized strategy tailored to individual needs and symptoms. Treatment options encompass a spectrum of approaches, from hormone replacement therapy to alternative therapies and the careful management of related conditions. The primary goal is to alleviate symptoms, maintain bone health, and support reproductive goals, if applicable.
Hormone Replacement Therapy (HRT)
Hormone replacement therapy (HRT) plays a crucial role in managing POI. HRT replenishes the missing estrogen and other hormones, mitigating the symptoms associated with the condition. This therapy comes in various forms, including pills, patches, creams, and gels, each with its own advantages and potential side effects. The optimal HRT regimen is determined by a healthcare professional, considering factors such as individual needs, health history, and preferences.
Potential Side Effects of HRT
While HRT is often effective, it’s essential to be aware of potential side effects. These can include bloating, breast tenderness, headaches, mood changes, and in some cases, a higher risk of blood clots or uterine cancer. Regular monitoring with a healthcare provider is crucial to manage these side effects and adjust the HRT regimen as needed. Careful consideration of the individual’s medical history and risk factors is essential when prescribing HRT.
Alternative Therapies
Alternative therapies, such as acupuncture, herbal remedies, and dietary modifications, may help alleviate some POI symptoms. However, it’s important to note that the effectiveness of these therapies is not always well-documented, and they should be used in conjunction with conventional medical care, not as a replacement. Discussions with a healthcare professional are crucial before incorporating any alternative therapies into the treatment plan.
Dietary changes and lifestyle modifications may support symptom management, but they should not replace prescribed medications.
Managing Associated Conditions
POI often coexists with other health conditions, such as osteoporosis, cardiovascular disease, and depression. Addressing these associated conditions is just as important as managing POI itself. A comprehensive treatment plan should encompass strategies to mitigate these risks, potentially including medications, lifestyle changes, and regular check-ups.
Table of Treatment Options for POI
| Treatment | Method | Benefits | Drawbacks |
|---|---|---|---|
| Hormone Replacement Therapy (HRT) | Various forms (pills, patches, creams, gels) | Relieves symptoms, maintains bone health, potentially supports fertility (in some cases). | Potential side effects (blood clots, uterine cancer, etc.), requires regular monitoring, and can be costly. |
| Lifestyle Modifications | Diet, exercise, stress management | Improved overall health, potential symptom reduction. | May not be sufficient for all symptoms, requires consistent effort. |
| Alternative Therapies (e.g., Acupuncture, Herbal Remedies) | Complementary therapies | Potential symptom relief. | Limited scientific evidence, may not be suitable for all individuals, and should be used cautiously. |
| Management of Associated Conditions | Medications, lifestyle changes, regular check-ups | Reduces risk of long-term health problems. | Requires ongoing monitoring and potentially multiple specialists. |
Long-Term Health Implications: What Is Primary Ovarian Insufficiency
Primary ovarian insufficiency (POI) isn’t just a disruption of reproductive years; it significantly impacts a woman’s overall well-being in the long term. Understanding these implications is crucial for proactive management and ensuring a healthy future. Women with POI face a unique set of challenges requiring tailored strategies for preventative care and addressing potential complications.
Increased Risk of Specific Conditions
Women with POI are at a higher risk of developing certain health issues compared to their counterparts who experience normal ovarian function throughout their lives. This increased risk stems from the hormonal imbalances associated with POI. The reduced estrogen production leads to a cascade of potential health consequences. For example, reduced estrogen levels can accelerate bone loss, increasing the risk of osteoporosis.
Primary ovarian insufficiency (POI) is a condition where a woman’s ovaries stop working properly before the age of 40. It can affect fertility, and sometimes, lifestyle choices like the type of tea you drink might play a role. For example, understanding the nuances of black tea vs green tea could be part of a broader approach to overall health, which is crucial for managing POI.
Ultimately, though, the best approach to managing POI is a personalized one, with the help of a healthcare professional.
Importance of Regular Monitoring and Preventative Care
Regular check-ups and proactive preventative measures are essential for managing the long-term health implications of POI. This includes monitoring bone density, cardiovascular health, and mental well-being. Early detection and intervention are crucial for preventing complications and maintaining a high quality of life. These preventative strategies are not just about symptom management; they’re about empowering women to take control of their health trajectory.
Strategies for Managing the Psychological Impact of POI
The diagnosis and management of POI can be emotionally challenging for many women. It’s crucial to acknowledge the potential psychological impact and develop coping mechanisms. Support groups, counseling, and open communication with healthcare providers can help women navigate the emotional complexities associated with this condition. Finding support systems and understanding that feelings of anxiety or depression are valid reactions to a significant health change is essential for well-being.
Potential Impact on Bone Health
The reduced estrogen production in POI significantly impacts bone health. Lower estrogen levels lead to accelerated bone loss, increasing the risk of osteoporosis and fractures. Women with POI may experience bone density loss at an earlier age and at a faster rate compared to those with normal ovarian function. This is a critical area for proactive monitoring and treatment to prevent long-term complications.
Table: Potential Long-Term Health Implications of POI
| Issue | Impact | Prevention | Management |
|---|---|---|---|
| Osteoporosis | Increased risk of fractures, reduced bone density, and potential disability. Examples include wrist or hip fractures. | Regular weight-bearing exercise, adequate calcium and vitamin D intake, and potentially medication. | Bone density scans (DEXA scans) to monitor bone health. Estrogen therapy (if appropriate) and/or other medications to maintain bone density. |
| Cardiovascular Disease | Higher risk of heart disease, stroke, and high blood pressure. For example, increased risk of developing high cholesterol or high blood pressure. | Maintaining a healthy weight, regular exercise, a balanced diet low in saturated and trans fats, and blood pressure management. | Regular cardiovascular screenings, blood pressure monitoring, and cholesterol management. |
| Mental Health Issues | Increased risk of anxiety, depression, and other mental health concerns due to hormonal changes and the impact on fertility. | Stress management techniques, support groups, and counseling can help. Open communication with healthcare providers and support systems. | Regular mental health check-ups, counseling, and support groups. Addressing any underlying anxiety or depression promptly. |
| Metabolic Syndrome | Increased risk of conditions like type 2 diabetes, high blood pressure, high cholesterol, and obesity. | Maintaining a healthy weight, balanced diet, and regular exercise. | Regular blood sugar and lipid monitoring, blood pressure management, and lifestyle modifications. |
Research and Future Directions
Primary Ovarian Insufficiency (POI) research is actively exploring various avenues to better understand its complexities and develop effective treatments and preventative strategies. Current studies are focusing on identifying underlying causes, improving diagnostic accuracy, and ultimately enhancing the quality of life for women affected by POI. This exploration includes understanding the long-term health implications and the often-overlooked psychological impact.Research in this area is crucial, as POI affects women in their reproductive years, impacting their ability to conceive naturally and potentially increasing their risk of developing other health problems later in life.
The ongoing investigation into POI is vital for improving outcomes and providing support to those affected.
Current Research on POI
Research into POI is multifaceted, encompassing genetic studies, hormonal investigations, and exploration of environmental factors. Researchers are actively seeking to understand the intricate interplay of genes, hormones, and environmental triggers that contribute to the development of POI. Studies are investigating specific genetic markers and hormonal imbalances, aiming to develop more accurate diagnostic tools and targeted treatments. Preliminary findings suggest that certain genetic mutations may increase the risk of POI, but more research is needed to confirm these connections.
Investigating environmental factors, such as exposure to toxins or certain medications, is also an important area of research.
Promising Areas of Research
Several promising research areas hold the potential to revolutionize our understanding and treatment of POI. These include:
- Identifying specific genetic markers: This involves pinpointing genetic variations that may predispose individuals to POI. If successful, this knowledge could lead to early detection and potentially preventative measures.
- Developing novel diagnostic tools: Researchers are actively working on refining diagnostic methods for POI, particularly in the early stages. This could include blood tests, imaging techniques, or even biomarkers that accurately identify women at risk.
- Exploring novel treatment strategies: Current treatment options primarily focus on hormone replacement therapy. However, ongoing research investigates alternative therapies and strategies for improving fertility outcomes, such as assisted reproductive technologies (ART) tailored for POI. Research is also exploring potential preventative measures for those at high risk.
- Addressing the psychological impact of POI: Recognizing and addressing the emotional and psychological toll of POI is crucial. This includes understanding the specific challenges women face, developing support programs, and integrating mental health resources into treatment plans.
Potential Future Treatments and Preventative Strategies
Future treatments for POI might include targeted therapies based on specific genetic or hormonal profiles. Early detection and intervention, based on identified risk factors, could potentially slow or prevent the progression of the condition. Preventative strategies could involve lifestyle modifications, such as a balanced diet and regular exercise, to mitigate the risk of POI in susceptible individuals.
Importance of Ongoing Research
Ongoing research is critical for improving the lives of women with POI. Better understanding of the underlying causes, development of more accurate diagnostic tools, and exploration of novel treatments will ultimately lead to improved outcomes and better quality of life for those affected.
Need for More Research on the Psychological Impact of POI
The psychological impact of POI is often overlooked, despite its significant effect on women’s well-being. Research is needed to better understand the emotional distress, body image issues, and social challenges associated with the condition. This understanding is essential for developing comprehensive support programs that address the emotional needs of women with POI.
Key Research Areas in POI
| Area | Current Status | Future Directions | Potential Impact |
|---|---|---|---|
| Identifying specific genetic markers | Some preliminary studies have identified potential genetic links, but further research is needed. | Developing genetic tests for early detection and personalized risk assessment. | Improved early detection and potentially preventative measures. |
| Developing novel diagnostic tools | Ongoing research focuses on refining current diagnostic methods and exploring new biomarkers. | Development of rapid, accurate, and non-invasive diagnostic tests for early detection and monitoring. | Improved accuracy and earlier intervention for treatment. |
| Exploring novel treatment strategies | Current treatments primarily involve hormone replacement therapy. | Investigating targeted therapies based on individual genetic profiles and exploring assisted reproductive technologies (ART) tailored for POI. | Potential improvement in fertility outcomes and quality of life. |
| Addressing the psychological impact of POI | Limited research currently exists on the psychological aspects of POI. | Developing targeted support programs and incorporating mental health services into treatment plans. | Improved mental well-being and quality of life for women with POI. |
Last Word

In summary, primary ovarian insufficiency, while presenting unique challenges, is a manageable condition. By understanding its causes, symptoms, and treatment options, women can take proactive steps to maintain their overall well-being. Early diagnosis and comprehensive care are essential to address the short-term and long-term impacts of POI. Further research and awareness are critical to advancing treatment options and improving the quality of life for those affected.
Remember, support systems and open communication are crucial for navigating this journey.










 This flowchart provides a visual representation of the steps involved in using a gold plan. The flow chart should be well-labeled and clearly display the steps involved in enrolling, submitting claims, navigating the claims process, and utilizing provider support.
This flowchart provides a visual representation of the steps involved in using a gold plan. The flow chart should be well-labeled and clearly display the steps involved in enrolling, submitting claims, navigating the claims process, and utilizing provider support.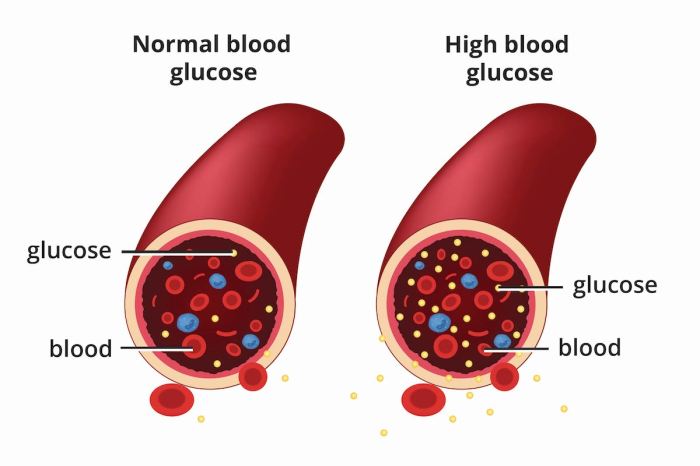
 The figure illustrates the potential progression of both diabetes and colon cancer in a single patient. The x-axis represents time, and the y-axis represents the severity of each disease. The figure demonstrates how poorly controlled diabetes, represented by the upward trend in blood glucose levels, can correlate with the development and progression of precancerous polyps and ultimately, colon cancer. The figure highlights the importance of early detection and consistent management of both conditions to mitigate the risk and improve outcomes.
The figure illustrates the potential progression of both diabetes and colon cancer in a single patient. The x-axis represents time, and the y-axis represents the severity of each disease. The figure demonstrates how poorly controlled diabetes, represented by the upward trend in blood glucose levels, can correlate with the development and progression of precancerous polyps and ultimately, colon cancer. The figure highlights the importance of early detection and consistent management of both conditions to mitigate the risk and improve outcomes.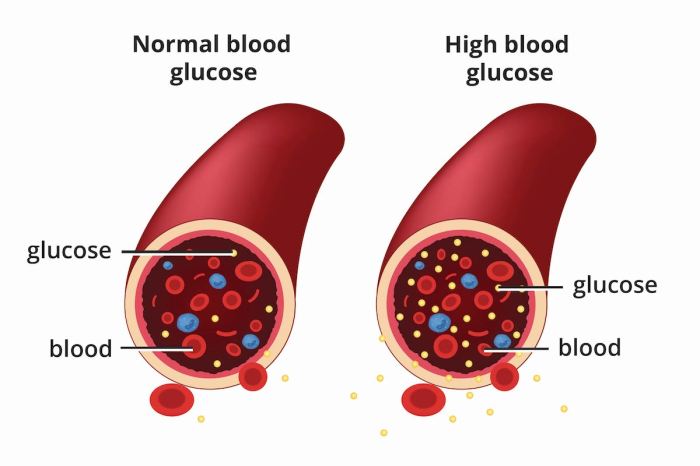


 (Diagram placeholder. A permanent pacemaker is typically implanted under the skin near the collarbone, with thin wires (leads) extending to the heart chambers. The pulse generator is housed within the implanted casing.)
(Diagram placeholder. A permanent pacemaker is typically implanted under the skin near the collarbone, with thin wires (leads) extending to the heart chambers. The pulse generator is housed within the implanted casing.)













