Magnesium and metabolic syndrome study delves into the intricate relationship between magnesium intake and metabolic syndrome. Metabolic syndrome, a cluster of conditions increasing the risk of heart disease, stroke, and type 2 diabetes, often goes hand-in-hand with inadequate magnesium levels. This study explores the potential mechanisms, research findings, and dietary implications of magnesium’s role in metabolic health. We’ll examine how magnesium impacts key aspects of metabolism, including insulin sensitivity, glucose regulation, and inflammation, and discuss the potential for dietary interventions to mitigate metabolic syndrome risk.
The study will cover a broad spectrum of topics, from defining metabolic syndrome and outlining its components to summarizing key research studies. It will also discuss the potential biological mechanisms linking magnesium to metabolic syndrome risk factors, the importance of dietary sources of magnesium, and recommended intake levels. Furthermore, it will explore potential future research directions and present illustrative data visualization techniques.
Introduction to Magnesium and Metabolic Syndrome
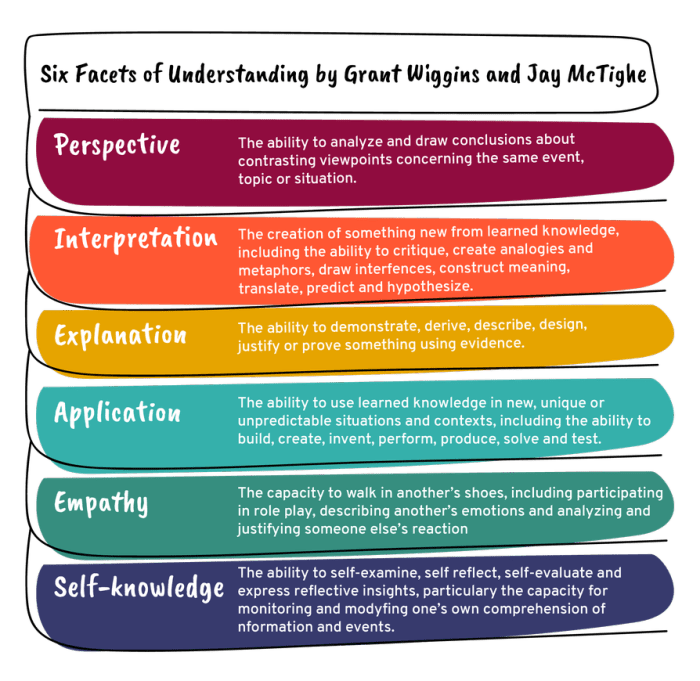
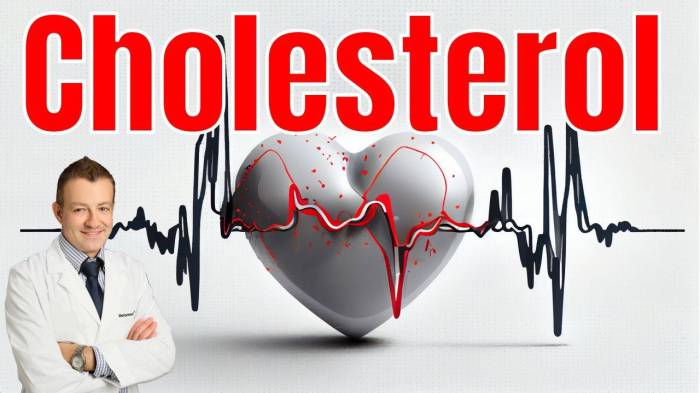
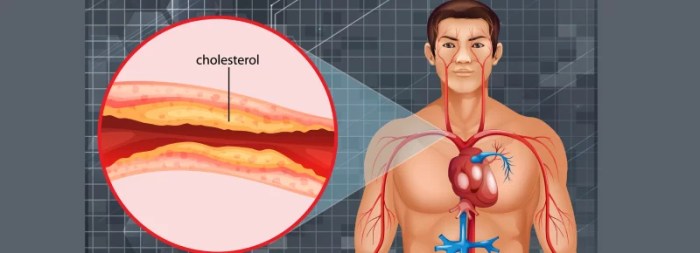
Metabolic syndrome is a cluster of conditions that increase the risk of heart disease, stroke, and type 2 diabetes. These conditions often occur together and include high blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol or triglyceride levels. Understanding the intricate interplay of these factors is crucial for effective prevention and management strategies.Magnesium, a crucial mineral, plays a significant role in numerous metabolic processes.
Its deficiency can disrupt these processes, potentially contributing to the development and progression of metabolic syndrome. This exploration will delve into the intricate relationship between magnesium and metabolic syndrome, examining the potential mechanisms by which magnesium deficiency may contribute to this cluster of disorders. We will also present a summary table to illustrate the potential links between specific metabolic syndrome components and magnesium status.
Defining Metabolic Syndrome
Metabolic syndrome is characterized by a constellation of interrelated metabolic abnormalities. These include elevated blood pressure, high blood sugar levels, increased abdominal fat, and abnormal blood lipid profiles. The precise criteria and thresholds for diagnosing metabolic syndrome vary slightly between organizations, but the underlying concept remains consistent. The presence of these factors significantly elevates the risk of cardiovascular disease and type 2 diabetes.
Magnesium’s Role in Metabolic Health
Magnesium is a vital nutrient involved in hundreds of enzymatic reactions within the body. It is crucial for regulating blood sugar levels, blood pressure, and insulin sensitivity. Adequate magnesium intake is essential for maintaining healthy metabolic function and preventing metabolic disorders. Magnesium’s role extends to muscle and nerve function, and it contributes to the body’s calcium balance.
Potential Mechanisms of Magnesium Deficiency and Metabolic Syndrome
Magnesium deficiency can disrupt several metabolic pathways, potentially contributing to the development of metabolic syndrome. Reduced insulin sensitivity, impaired glucose metabolism, and dysregulation of blood pressure are some key consequences of insufficient magnesium intake. Magnesium deficiency may also influence the body’s ability to manage fat metabolism and inflammation, both of which are linked to metabolic syndrome. Furthermore, magnesium plays a role in regulating blood pressure, and its deficiency can contribute to hypertension.
Current Understanding of the Relationship
The research on the relationship between magnesium and metabolic syndrome is growing, though not fully conclusive. Some studies suggest a correlation between low magnesium levels and the prevalence of metabolic syndrome, while others have found no significant association. The complexity of the underlying mechanisms and the potential confounding factors involved make definitive conclusions challenging.
Summary of Metabolic Syndrome Components and Potential Links to Magnesium Status
| Component | Description | Potential Magnesium Role | Evidence |
|---|---|---|---|
| Elevated Blood Pressure | Systolic blood pressure consistently above 130 mmHg and/or diastolic blood pressure consistently above 85 mmHg. | Magnesium plays a role in vascular relaxation and blood pressure regulation. Deficiency may impair these functions, contributing to hypertension. | Some studies show an association between low magnesium intake and hypertension, but more research is needed. |
| High Blood Sugar | Fasting blood glucose levels consistently above 100 mg/dL. | Magnesium is involved in insulin sensitivity and glucose metabolism. Deficiency may reduce insulin effectiveness, leading to hyperglycemia. | Studies suggest an association between low magnesium levels and impaired glucose tolerance, but the evidence is not always consistent. |
| Excess Abdominal Fat | Accumulation of fat around the waist, typically measured by waist circumference. | Magnesium deficiency may affect fat metabolism and distribution. The exact mechanisms are not fully understood, but the relationship is suspected. | Limited research specifically links magnesium to abdominal fat accumulation, requiring more investigation. |
| Abnormal Blood Lipid Profile | High levels of triglycerides and/or low levels of HDL cholesterol. | Magnesium may influence lipid metabolism and cholesterol levels, though the precise mechanism remains to be fully elucidated. | Studies have shown some associations, but the evidence is not always strong and needs more conclusive research. |
Research Studies on Magnesium and Metabolic Syndrome
Magnesium’s role in metabolic health is increasingly recognized. Numerous studies explore the association between magnesium intake/status and various metabolic syndrome risk factors. Understanding the findings, study designs, and limitations of these investigations is crucial for developing effective interventions.
A significant body of research investigates the potential link between magnesium deficiency and the development or exacerbation of metabolic syndrome. Observational and interventional studies have yielded valuable insights, but inconsistencies in results necessitate careful consideration of methodological nuances. Different study designs, populations, and outcome measures contribute to variations in findings. Analyzing these variations and identifying potential confounding factors are essential to understanding the true relationship between magnesium and metabolic syndrome.
Recent studies on magnesium and metabolic syndrome are fascinating, highlighting the mineral’s potential role in managing various aspects of the condition. While the exact mechanisms are still being explored, it’s clear that magnesium plays a crucial part in the body’s metabolic processes. For instance, understanding the differences in how drugs like Trulicity and Ozempic work, especially their efficacy and side effects, is also vital for people with metabolic conditions, as discussed in this detailed comparison: trulicity vs ozempic uses efficacy side effects.
Ultimately, more research into the interplay between magnesium, metabolic syndrome, and potential pharmaceutical interventions is needed to develop comprehensive treatment strategies.
Summary of Significant Studies
Numerous studies have examined the association between magnesium intake/status and metabolic syndrome risk factors. These studies employ diverse methodologies, including observational studies tracking dietary intake and blood magnesium levels, and interventional trials evaluating the effects of magnesium supplementation on metabolic markers. The goal of these investigations is to determine if magnesium plays a role in the development or progression of metabolic syndrome, and the mechanisms through which it might influence these processes.
Study Designs and Populations
Observational studies often involve large populations, such as cohorts or cross-sectional surveys. These studies help to identify correlations between magnesium intake and metabolic syndrome risk factors. Interventional studies, on the other hand, typically involve smaller groups of participants and may utilize controlled interventions like magnesium supplementation. These studies aim to establish cause-and-effect relationships between magnesium and metabolic outcomes.
Population characteristics, including age, gender, ethnicity, and baseline health conditions, significantly impact the findings of such studies. These characteristics must be taken into account when comparing results across different investigations.
Comparison of Findings and Discrepancies
Some studies show a positive association between lower magnesium intake or status and an increased risk of metabolic syndrome or its components (like high blood pressure, high blood sugar, and abdominal obesity). Other studies, however, do not show a consistent or significant association. This inconsistency might stem from variations in study populations, duration of follow-up, or the specific definitions used for metabolic syndrome.
Furthermore, confounding factors like dietary habits, physical activity, and other nutrient intakes can obscure the true effect of magnesium. The heterogeneity in study designs and populations poses challenges in drawing definitive conclusions.
Methodological Limitations
A key limitation in many studies is the reliance on self-reported dietary intake, which can be inaccurate and prone to recall bias. Assessment of magnesium status is also not always standardized across studies, making comparisons challenging. Furthermore, the duration of follow-up in some studies may not be long enough to detect subtle changes in metabolic syndrome risk factors.
Confounding factors, including socioeconomic status and other health conditions, are often not adequately controlled, potentially influencing the observed associations. The lack of a standardized definition of metabolic syndrome across studies also introduces variability in the results.
Table of Research Studies
| Study Type | Population | Findings | Limitations |
|---|---|---|---|
| Observational | Adults in a specific geographic region with diverse dietary habits | Lower magnesium intake associated with higher risk of metabolic syndrome. | Potential for confounding factors like dietary patterns and other nutritional deficiencies. Limited causal inferences. |
| Interventional | Individuals with prediabetes, receiving magnesium supplementation for 6 months. | Magnesium supplementation did not significantly improve insulin sensitivity or reduce metabolic risk factors. | Small sample size, short duration of the study, lack of a placebo control group. |
| Observational | Post-menopausal women enrolled in a cohort study | Low magnesium status was linked to elevated fasting blood glucose levels. | Potential for other factors influencing both magnesium levels and blood glucose. Self-reported dietary data. |
| Interventional | Individuals with diagnosed metabolic syndrome, following a specific magnesium-rich diet. | Participants on a magnesium-rich diet showed improvements in blood pressure and lipid profiles. | Lack of a control group, and the study duration might not have been long enough to evaluate long-term effects. |
Mechanisms Linking Magnesium and Metabolic Syndrome

Magnesium plays a crucial role in numerous metabolic processes, and its deficiency has been implicated in the development and progression of metabolic syndrome. Understanding the intricate mechanisms through which magnesium influences various metabolic risk factors is essential for developing effective preventative and therapeutic strategies. These mechanisms are often interconnected, highlighting the importance of magnesium in maintaining overall metabolic health.The biological mechanisms connecting magnesium to metabolic syndrome are multifaceted and involve several key metabolic pathways.
These interactions are complex, and research continues to unravel the intricate details of how magnesium impacts insulin sensitivity, glucose regulation, inflammation, lipid profiles, and blood pressure. This exploration aims to provide a comprehensive overview of the proposed mechanisms, linking them to specific components of metabolic syndrome.
Magnesium’s Role in Insulin Sensitivity
Magnesium is essential for insulin signaling and glucose uptake into cells. A magnesium deficiency can impair insulin receptor function, leading to reduced insulin sensitivity and, subsequently, impaired glucose homeostasis. This reduced sensitivity can lead to elevated blood glucose levels and increase the risk of developing type 2 diabetes, a key component of metabolic syndrome.
Recent studies on magnesium and metabolic syndrome are fascinating. They suggest a potential link between low magnesium levels and increased risk of high blood pressure, a key component of metabolic syndrome. Understanding what causes high blood pressure is crucial for effectively managing this complex condition. This further emphasizes the importance of magnesium’s role in overall metabolic health and highlights the need for more research in this area.
Magnesium’s Role in Glucose Metabolism, Magnesium and metabolic syndrome study
Magnesium is critical for numerous enzymatic reactions involved in glucose metabolism. These reactions, including glycolysis and the Krebs cycle, rely on magnesium as a cofactor. Deficiency in magnesium can disrupt these processes, leading to impaired glucose utilization and elevated blood glucose levels. Furthermore, magnesium deficiency can impair glycogen synthesis and storage, contributing to glucose intolerance.
Magnesium’s Role in Inflammation
Chronic low-grade inflammation is a hallmark of metabolic syndrome. Magnesium has anti-inflammatory properties. It may modulate the production of inflammatory cytokines, such as TNF-alpha and IL-6. Maintaining adequate magnesium levels may help reduce inflammation, thus mitigating the risk factors associated with metabolic syndrome. Reduced inflammation may lead to a decrease in the risk of insulin resistance and other metabolic complications.
Magnesium’s Impact on Lipid Profiles
Magnesium may influence lipid profiles by regulating the synthesis and metabolism of lipids. Studies suggest that magnesium deficiency may be associated with increased levels of triglycerides and LDL cholesterol. Conversely, adequate magnesium intake may help maintain healthy lipid levels, potentially reducing the risk of dyslipidemia, another key component of metabolic syndrome.
Magnesium’s Role in Blood Pressure Regulation
Magnesium is involved in the regulation of vascular tone and blood pressure. It helps relax blood vessels, contributing to healthy blood pressure levels. Magnesium deficiency may contribute to increased vascular stiffness and hypertension, further exacerbating the risk factors associated with metabolic syndrome. Maintaining optimal magnesium levels could potentially reduce blood pressure and improve vascular health.
Table: Mechanisms Linking Magnesium and Metabolic Syndrome
| Mechanism | Metabolic Syndrome Component | Explanation |
|---|---|---|
| Insulin Sensitivity | Insulin Resistance | Magnesium is crucial for insulin signaling and glucose uptake. Deficiency impairs insulin receptor function, leading to reduced insulin sensitivity. |
| Glucose Metabolism | Hyperglycemia | Magnesium acts as a cofactor for enzymes in glucose metabolism. Deficiency disrupts these processes, leading to impaired glucose utilization. |
| Inflammation | Chronic Inflammation | Magnesium possesses anti-inflammatory properties, potentially modulating the production of inflammatory cytokines, reducing inflammation and improving insulin sensitivity. |
| Lipid Profiles | Dyslipidemia | Magnesium may influence lipid synthesis and metabolism. Deficiency may be associated with increased triglycerides and LDL cholesterol. |
| Blood Pressure Regulation | Hypertension | Magnesium helps regulate vascular tone and blood pressure. Deficiency may lead to increased vascular stiffness and hypertension. |
Dietary Sources and Recommendations: Magnesium And Metabolic Syndrome Study
Nourishing your body with the right foods is crucial for overall health, and this includes ensuring adequate magnesium intake. Magnesium plays a vital role in countless bodily functions, including energy production and blood sugar regulation. This section delves into the dietary sources of magnesium, highlighting the recommended daily intake for various population groups, and discussing the potential benefits of magnesium-rich diets for metabolic syndrome management.
Dietary Sources of Magnesium
Magnesium is widely distributed throughout the food kingdom, not concentrated in a few specific foods. Its presence varies significantly across different food groups. Leafy green vegetables, whole grains, legumes, and nuts are excellent sources. Animal products, while containing magnesium, typically offer lower amounts compared to plant-based options. Understanding the diverse sources and their respective magnesium content allows for the creation of a balanced and varied diet.
Recommended Dietary Allowance (RDA) for Magnesium
The recommended daily intake of magnesium varies depending on factors such as age, sex, and overall health. The RDA serves as a guideline for adequate intake, aiming to support optimal bodily functions. Meeting these recommendations can play a vital role in preventing deficiencies and potentially managing metabolic syndrome. Consult with a healthcare professional or registered dietitian for personalized advice on magnesium intake.
Potential Role in Preventing/Managing Metabolic Syndrome
A well-balanced diet rich in magnesium may contribute to the prevention or management of metabolic syndrome. Studies suggest a potential link between adequate magnesium intake and improved blood sugar control, blood pressure regulation, and insulin sensitivity. These factors are all key components in metabolic syndrome management, and a diet emphasizing magnesium-rich foods may offer valuable support.
Dietary Magnesium Sources Table
| Food | Magnesium Content (mg) | Serving Size |
|---|---|---|
| Spinach (cooked) | 70 | 1 cup |
| Almonds | 60 | 1/4 cup |
| Black beans | 30 | 1 cup |
| Whole-wheat bread | 40 | 1 slice |
| Avocado | 25 | 1/2 avocado |
| Salmon (cooked) | 35 | 3 ounces |
Note: Magnesium content may vary based on preparation methods and growing conditions. This table provides a general guideline.
Implications and Future Directions
The research on magnesium and metabolic syndrome reveals a compelling link between adequate magnesium intake and improved metabolic health. Understanding this relationship has significant implications for public health strategies aimed at preventing and managing metabolic syndrome, a cluster of conditions that increases the risk of heart disease, stroke, and type 2 diabetes. This section explores the potential applications of this knowledge in dietary recommendations and preventive strategies, along with promising avenues for future research.
Public Health Implications
The findings highlight the importance of magnesium in maintaining metabolic health. Public health interventions should focus on increasing dietary magnesium intake through various strategies, including education campaigns promoting magnesium-rich foods, fortification of staple foods, and potentially even supplementation in at-risk populations. These initiatives could have a substantial impact on reducing the prevalence of metabolic syndrome and associated chronic diseases.
Recent studies on magnesium and metabolic syndrome are fascinating, highlighting its potential role in managing the condition. Maintaining a healthy immune system is crucial, especially for healthcare workers, and recommended vaccinations for healthcare workers play a vital part in this. Ultimately, the research into magnesium and metabolic syndrome continues to offer promising insights into preventative healthcare.
For example, public health campaigns could emphasize the importance of whole grains, leafy greens, nuts, and legumes, which are excellent sources of magnesium.
Dietary Recommendations and Preventive Strategies
Current dietary guidelines often lack specific recommendations regarding magnesium intake. Future guidelines should incorporate magnesium as a crucial nutrient for metabolic health, providing clear recommendations for daily intake based on age, sex, and activity levels. This would necessitate a comprehensive evaluation of existing dietary guidelines, and potentially lead to adjustments in food labeling requirements to include magnesium content.
For example, food manufacturers could be encouraged to increase magnesium content in processed foods while maintaining nutritional value. Preventive strategies could include targeted dietary interventions for individuals at high risk of metabolic syndrome, focusing on increasing magnesium intake and maintaining a balanced diet.
Potential Areas for Future Research
Further research is essential to fully elucidate the complex relationship between magnesium and metabolic syndrome. This includes exploring the potential benefits of specific magnesium forms, investigating interactions with other nutrients, and examining the role of magnesium in different stages of metabolic syndrome development. For instance, exploring the effects of different magnesium salts (e.g., magnesium citrate, magnesium glycinate) on metabolic markers could yield valuable insights.
Table of Potential Future Research Avenues
| Research Area | Potential Impact | Methodological Considerations |
|---|---|---|
| Specific Magnesium Forms | Identifying optimal magnesium forms for metabolic improvement. This could lead to targeted supplementation strategies. | Rigorous clinical trials comparing the efficacy of various magnesium forms on metabolic markers. Considerations for bioavailability and potential side effects of each form are crucial. |
| Magnesium-Nutrient Interactions | Understanding how magnesium interacts with other nutrients (e.g., calcium, potassium) in influencing metabolic outcomes. | Controlled dietary interventions examining the combined effects of magnesium and other key nutrients on metabolic parameters. Careful monitoring of interactions between nutrients is essential. |
| Magnesium and Metabolic Syndrome Stages | Assessing the impact of magnesium intake at different stages of metabolic syndrome development, from pre-diabetes to full-blown syndrome. | Longitudinal studies following individuals over time, tracking magnesium intake and metabolic markers across different stages of the disease progression. |
| Magnesium Bioavailability | Determining factors influencing magnesium absorption and utilization in the body. | Investigating the role of gut health, genetic predisposition, and other physiological factors in magnesium bioavailability. |
Illustrative Data Presentation
Visualizing the relationship between magnesium intake and metabolic syndrome risk factors is crucial for understanding the potential impact of magnesium supplementation. Effective graphical representations can highlight trends, patterns, and correlations, facilitating a deeper comprehension of the data and supporting evidence-based recommendations. This section will explore various graph types and their suitability for different data sets, providing practical examples.
Graph Types for Data Visualization
Understanding the nuances of different graph types is key to effectively communicating research findings. Choosing the right graph depends on the nature of the data being analyzed and the specific relationships being explored. The following table Artikels common graph types and their suitability for various data sets related to magnesium intake and metabolic syndrome.
| Graph Type | Data Suitability | Example Application |
|---|---|---|
| Scatter Plot | Illustrating the relationship between two continuous variables (e.g., magnesium intake and blood pressure). | Plotting magnesium intake (mg/day) against fasting blood glucose levels (mg/dL) to visualize potential correlations. A strong negative correlation might suggest that higher magnesium intake is associated with lower blood glucose levels. |
| Line Graph | Demonstrating trends over time or across different groups (e.g., changes in waist circumference over time or comparisons between magnesium-supplemented and control groups). | Tracking changes in waist circumference (cm) over a 12-month period for individuals in a magnesium supplementation trial. The line graph would show the trend in waist circumference over time, potentially highlighting the effect of the supplement. |
| Bar Graph | Comparing categorical data (e.g., magnesium intake levels categorized by different dietary patterns or comparing risk factors across various age groups). | Comparing the average magnesium intake (mg/day) across different dietary patterns (e.g., Mediterranean, Western). The bar graph would visually represent the differences in magnesium intake between the dietary groups. |
| Box Plot | Summarizing the distribution of a variable across different groups (e.g., comparing the distribution of fasting insulin levels in individuals with varying magnesium intake levels). | Comparing the distribution of fasting insulin levels (µIU/mL) in individuals with high and low magnesium intake. The box plot would visually represent the median, quartiles, and potential outliers for each group, facilitating a comparison of the central tendency and variability. |
| Histogram | Showing the frequency distribution of a continuous variable (e.g., the distribution of magnesium intake levels in a population sample). | Representing the frequency of magnesium intake levels (mg/day) in a population sample. The histogram would show the shape of the distribution and identify potential clusters or peaks in the data. |
Interpreting Graphical Representations
Carefully interpreting the visualizations is critical for drawing accurate conclusions. Look for patterns, trends, and correlations within the data. For example, a strong negative correlation in a scatter plot between magnesium intake and blood pressure levels would suggest that higher magnesium intake is associated with lower blood pressure. Considering the limitations of the data and potential confounding factors is also important.
Final Thoughts

In conclusion, this study on magnesium and metabolic syndrome highlights the potential importance of magnesium in preventing and managing metabolic syndrome. The research suggests a strong correlation between magnesium status and various metabolic risk factors, although further investigation is needed to fully elucidate the underlying mechanisms. Ultimately, understanding this intricate relationship is crucial for developing effective public health strategies and personalized dietary recommendations to promote metabolic health and reduce the burden of metabolic syndrome.