Facts about parkinsons disease – Facts about Parkinson’s disease sets the stage for this enthralling narrative, offering readers a glimpse into a complex and multifaceted condition. This comprehensive exploration delves into the various aspects of Parkinson’s, from its core symptoms and causes to treatment options and the impact it has on individuals and families.
We’ll cover the basics, including definitions, symptoms, and how Parkinson’s affects daily life. Then, we’ll examine the possible causes and risk factors, along with the diagnostic process and available treatment options. Furthermore, we’ll explore strategies for living with the disease, the challenges faced by families and caregivers, and the ongoing research into potential treatments and preventive measures. Finally, we’ll look at illustrative case studies and the impact of the disease on individual lives.
Introduction to Parkinson’s Disease
Parkinson’s disease is a progressive neurological disorder that affects movement. It’s characterized by a gradual decline in the production of dopamine, a crucial neurotransmitter involved in controlling movement. This decline leads to a range of motor and non-motor symptoms that progressively worsen over time. The disease typically affects people over the age of 60, although younger onset cases do exist.Understanding the core symptoms, stages, and impact of Parkinson’s disease is vital for effective management and support for individuals living with this condition.
Early diagnosis and appropriate treatment strategies can significantly improve quality of life and slow the progression of the disease.
Definition of Parkinson’s Disease
Parkinson’s disease is a neurodegenerative disorder primarily affecting the central nervous system. It’s characterized by the degeneration of dopamine-producing neurons in a specific area of the brain, leading to a deficiency in dopamine. This deficiency disrupts the normal functioning of the brain’s motor control system.
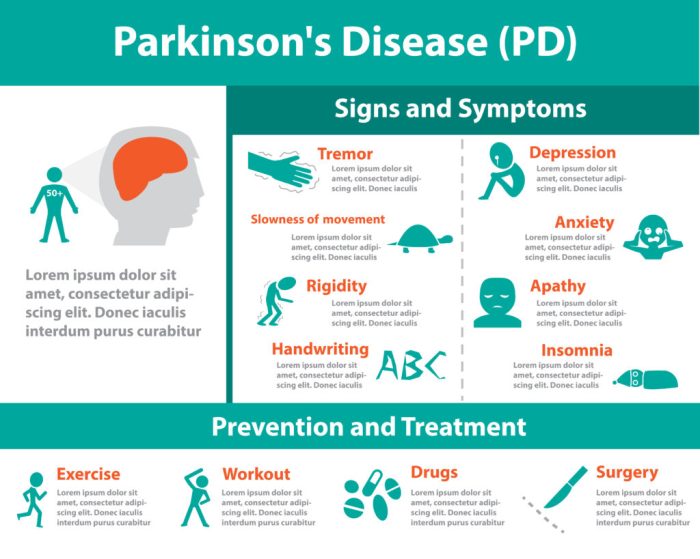
Core Symptoms of Parkinson’s Disease
The primary motor symptoms of Parkinson’s disease include tremors, rigidity, bradykinesia (slowness of movement), and postural instability. Tremors are often the first noticeable symptom, typically occurring at rest and affecting one hand. Rigidity manifests as stiffness in the muscles, making movement difficult and jerky. Bradykinesia leads to slowness in initiating and performing movements, and postural instability results in impaired balance and an increased risk of falls.
Learning about Parkinson’s disease is fascinating, but it’s also important to understand how various health conditions can intertwine. For example, some medications for atrial fibrillation, like medications for atrial fibrillation , might have unexpected interactions with Parkinson’s treatments. This highlights the complexity of managing multiple health issues and the importance of consulting with healthcare professionals. Ultimately, staying informed about Parkinson’s disease is key to understanding potential connections and managing care effectively.
Impact of Parkinson’s Disease on Daily Life
Parkinson’s disease significantly impacts daily life. The progressive nature of the disease often leads to difficulties in performing routine tasks like dressing, eating, and walking. The non-motor symptoms, such as sleep disturbances, cognitive impairment, and depression, further complicate daily functioning. These challenges can affect social interactions, employment, and overall well-being.
Stages of Parkinson’s Disease
The progression of Parkinson’s disease is typically categorized into stages, reflecting the severity of symptoms and impact on daily life. This classification aids in treatment planning and managing expectations.
| Stage | Symptoms | Treatments | Quality of Life Implications |
|---|---|---|---|
| Early Stage (1-2) | Mild tremors and rigidity, noticeable only during specific activities. Walking and balance may be slightly affected. | Medication to manage symptoms, physical therapy to maintain mobility. | Individuals can often maintain independence in daily activities. Social and occupational functioning remain largely intact. |
| Mid Stage (3-4) | Tremors and rigidity become more pronounced. Walking difficulties, balance problems, and increased risk of falls are evident. Speech may become slurred. Difficulty with fine motor skills. | Increased medication dosage, consideration of deep brain stimulation (DBS) for severe cases. Ongoing physical therapy and occupational therapy for improved mobility and daily living skills. | Individuals may require assistance with daily tasks. Social interaction may be impacted due to mobility challenges. |
| Late Stage (5) | Significant motor impairment. Individuals may require assistance with all aspects of daily living, including walking, dressing, and eating. Cognitive decline and other non-motor symptoms may be prominent. | High doses of medication. Advanced therapies like DBS, if appropriate. Specialized caregiving and support are crucial. | Significant dependence on caregivers for all aspects of daily life. Reduced social interaction and potential for isolation. |
Causes and Risk Factors: Facts About Parkinsons Disease
Understanding the causes of Parkinson’s Disease is crucial for developing effective treatments and preventive strategies. While the precise mechanisms remain somewhat elusive, researchers have identified a complex interplay of genetic predispositions and environmental influences that contribute to the development of this debilitating neurological disorder. This exploration will delve into the known causes and risk factors, offering insights into the factors that may increase a person’s vulnerability to Parkinson’s.
Known Causes
Parkinson’s Disease is not fully understood, but several contributing factors are recognized. Genetic predispositions, environmental exposures, and a combination of both play significant roles in its development. The interplay of these factors is often complex and not yet fully elucidated. The specific mechanisms by which these factors contribute to the disease’s progression remain an active area of research.
Genetic Factors
Certain genetic mutations have been linked to an increased risk of developing Parkinson’s Disease. Individuals with a family history of Parkinson’s are more likely to develop the disease themselves, suggesting a genetic component. Specific genes involved in dopamine production and neuronal function have been identified as potential contributors to the disease’s development. However, it’s crucial to understand that a genetic predisposition doesn’t guarantee the development of Parkinson’s, and many people with these genes do not develop the disease.
Environmental Factors
Environmental exposures have also been implicated in Parkinson’s Disease development. Exposure to certain pesticides and herbicides has been associated with a heightened risk. Furthermore, some studies suggest a potential link between repeated head trauma and the development of Parkinson’s. While these environmental factors are recognized as potential contributors, the precise mechanisms through which they affect the brain remain unclear.
Understanding these interactions is essential for the development of preventive measures.
Comparison of Risk Factors
| Risk Factor | Description | Potential Impact | Examples |
|---|---|---|---|
| Genetics | Specific gene mutations can increase the likelihood of developing Parkinson’s. | Increased susceptibility to the disease, especially with a family history. | Mutations in genes like LRRK2 and PARKIN. |
| Environmental Toxins | Exposure to certain pesticides, herbicides, and heavy metals. | Possible disruption of neuronal function, potentially leading to Parkinson’s development. | Exposure to rotenone, manganese, or paraquat. |
| Head Trauma | Repeated head injuries, such as those sustained in sports or accidents. | Potentially increased risk of developing Parkinson’s, particularly with cumulative trauma. | Concussions or repeated blows to the head. |
| Age | The risk of Parkinson’s increases with age. | A major risk factor, as the aging process affects brain function. | Individuals over 60 are more susceptible. |
Diagnosis and Assessment
Diagnosing Parkinson’s Disease involves a careful evaluation process, combining medical history, neurological examinations, and various diagnostic tools. The process aims to rule out other conditions with similar symptoms, ensuring an accurate diagnosis to guide appropriate treatment strategies. Accurate diagnosis is crucial for timely intervention and management of the disease.Neurological examinations are paramount in assessing Parkinson’s Disease. These examinations evaluate motor skills, balance, reflexes, and cognitive functions.
They provide valuable insights into the progression and severity of the disease, helping clinicians determine the best course of action. The findings from these examinations, combined with other data, contribute to a more comprehensive understanding of the patient’s condition.
Neurological Examinations
Neurological examinations are essential for diagnosing Parkinson’s Disease. These examinations assess various aspects of the nervous system, including motor function, balance, coordination, reflexes, and cognitive abilities. A comprehensive neurological examination allows clinicians to identify specific signs and symptoms indicative of Parkinson’s Disease. Observations of posture, gait, tremors, rigidity, bradykinesia, and other motor abnormalities are carefully noted during the examination.
Diagnostic Tools
Various diagnostic tools aid in the assessment of Parkinson’s Disease. These tools provide objective measurements and support the clinical evaluation, helping to confirm the diagnosis and differentiate it from other neurological disorders. The integration of multiple diagnostic methods improves the accuracy of the diagnosis.
Diagnostic Procedures
The following table summarizes key diagnostic procedures used for Parkinson’s Disease, outlining their purpose, procedure, and typical results.
| Procedure | Description | Procedure Details | Typical Results (Parkinson’s Disease) |
|---|---|---|---|
| Detailed Medical History | Gathering information about the patient’s medical history, including symptoms, onset, duration, and progression of the condition. | In-depth discussion about the patient’s symptoms, lifestyle, family history, and use of medications. | Reports of gradual onset of tremors, rigidity, slowness of movement (bradykinesia), and balance problems. History of similar symptoms in family members may be reported. |
| Neurological Examination | Evaluation of motor skills, balance, reflexes, and cognitive functions. | Assessment of posture, gait, tremors, rigidity, bradykinesia, and response to commands. Tests for reflexes and coordination are also performed. | Presence of resting tremor, rigidity in limbs, bradykinesia (slow movement), difficulty with balance and coordination. |
| Imaging Studies (e.g., MRI, CT scan) | Imaging techniques to rule out other neurological conditions. | MRI scans create detailed images of the brain’s internal structures, while CT scans use X-rays to generate cross-sectional images. | Typically, normal brain structure and function, with no evidence of other neurological disorders, such as tumors or strokes. |
| Dopamine Transporter Scan (DaTscan) | A specialized imaging technique that assesses dopamine levels in the brain. | A radioactive tracer is injected, and images are taken to measure the uptake of dopamine in specific brain areas. | Reduced dopamine transporter uptake in the basal ganglia, which is a key area for Parkinson’s Disease. |
| Response to Levodopa | Assessment of the patient’s response to a medication known to alleviate Parkinson’s symptoms. | Administering a dose of levodopa and observing the effects on motor symptoms. | Significant improvement in motor symptoms (tremor, rigidity, bradykinesia) upon levodopa administration, providing strong evidence for Parkinson’s Disease. |
Treatment Options

Managing Parkinson’s Disease effectively involves a multifaceted approach combining medication and lifestyle adjustments. This section delves into the various treatment strategies available, from pharmacological interventions to non-pharmacological therapies, exploring their respective benefits and drawbacks. Understanding these options empowers individuals and their care teams to make informed decisions about the best course of action.
Pharmacological Treatments
Pharmacological treatments aim to alleviate motor symptoms by replenishing or mimicking dopamine levels in the brain. Levodopa is the most effective medication for Parkinson’s, converting to dopamine in the brain. Other medications, such as dopamine agonists, MAO-B inhibitors, and COMT inhibitors, are often used in combination with levodopa to manage symptoms and potential side effects.
- Levodopa: This is a cornerstone of Parkinson’s treatment, as it directly increases dopamine levels in the brain. Its effectiveness is high, but long-term use can lead to motor fluctuations and dyskinesias (involuntary movements). Individual responses vary, and the optimal dosage and timing are crucial for managing symptoms and minimizing side effects.
- Dopamine Agonists: These medications mimic the effects of dopamine in the brain. They can be effective in the early stages of Parkinson’s, but they may carry a higher risk of side effects, including impulse control disorders like compulsive gambling or shopping. The risk of these side effects generally increases with higher doses and longer durations of use.
- MAO-B Inhibitors: These medications help to slow the breakdown of dopamine in the brain. They are often used in combination with levodopa, particularly in the early stages of the disease, to help improve motor function and delay the need for higher doses of levodopa. Common side effects include nausea, vomiting, and dizziness.
- COMT Inhibitors: These medications help to prevent the breakdown of levodopa in the body, allowing more levodopa to reach the brain. They are typically used in combination with levodopa to enhance its effectiveness and reduce the need for higher doses. Potential side effects include nausea, vomiting, and diarrhea.
Non-Pharmacological Approaches
Non-pharmacological strategies play a vital role in managing the overall well-being of individuals with Parkinson’s. These approaches complement pharmacological treatments by addressing motor and non-motor symptoms, improving quality of life.
- Physical Therapy: Exercises and physical therapy routines help improve balance, mobility, and flexibility. These strategies are crucial in reducing the impact of motor symptoms and maintaining independence in daily activities. Specific exercises, such as Tai Chi and yoga, can be particularly beneficial.
- Occupational Therapy: Occupational therapists assist individuals in adapting their daily routines to accommodate the challenges posed by Parkinson’s. They focus on strategies for maintaining independence in activities like dressing, eating, and using the bathroom. Modifications to the home environment can also be implemented to enhance safety and accessibility.
- Speech Therapy: Speech therapy can help address communication difficulties, swallowing problems, and voice changes that often accompany Parkinson’s. This therapy can significantly improve communication and quality of life.
- Support Groups and Counseling: Support groups provide a platform for individuals with Parkinson’s and their families to connect, share experiences, and receive emotional support. Counseling can address the emotional and psychological challenges associated with the disease.
Comparison of Treatment Options
| Treatment Option | Pros | Cons | Suitability for Disease Stage |
|---|---|---|---|
| Levodopa | Highly effective in reducing motor symptoms; readily available. | Potential for motor fluctuations, dyskinesias; side effects can vary significantly. | Generally suitable for all stages, but adjustments may be needed as the disease progresses. |
| Dopamine Agonists | Effective in early stages; may delay the need for levodopa. | Higher risk of impulse control disorders, nausea, sleep disturbances; effectiveness can diminish over time. | Best suited for early stages; potential benefit for delaying levodopa initiation. |
| MAO-B Inhibitors | Can slow disease progression; often used in early stages. | Mild side effects are common; less potent than other options. | Beneficial in early-to-mid stages to complement other treatments. |
| COMT Inhibitors | Enhances levodopa’s effectiveness; reduces fluctuations. | Side effects like nausea and diarrhea can occur; often used in combination with levodopa. | Suitable for later stages when motor fluctuations become more pronounced. |
| Physical Therapy | Improves mobility, balance, and flexibility. | Requires consistent effort and adherence to the program. | Beneficial for all stages; crucial for maintaining independence. |
Living with Parkinson’s Disease
Navigating Parkinson’s disease requires a multifaceted approach that goes beyond medication. Effective management hinges on understanding the disease’s impact on daily life, adopting strategies for symptom control, and building a robust support system. This involves embracing lifestyle adjustments and proactive planning to maintain a high quality of life.Living well with Parkinson’s involves a conscious effort to adapt to the evolving challenges.
Did you know Parkinson’s disease is often associated with motor symptoms like tremors and rigidity? While researching the various health conditions linked to it, I stumbled upon the fascinating connection between Parkinson’s and potential liver issues, such as overview of fatty liver disease. Learning about the possible overlap between these two conditions has me thinking more about the complex interplay of factors influencing Parkinson’s progression.
It’s important to remember that further research is needed to definitively establish any direct causal links, but it’s definitely a compelling area of study.
Strategies for symptom management, strong support networks, and tailored lifestyle changes are crucial for individuals to live fulfilling lives despite the complexities of the disease. This section will explore these essential aspects in detail.
Symptom Management Strategies
Effective symptom management is key to maintaining quality of life for individuals with Parkinson’s. A comprehensive approach encompasses various strategies. This includes understanding the fluctuations in symptoms, recognizing triggers, and employing strategies to minimize their impact.
- Regular exercise is essential. Aerobic activities, such as walking or swimming, can help improve motor skills, balance, and overall well-being. Strength training exercises can enhance muscle strength and reduce stiffness. Physical therapy tailored to Parkinson’s can be highly beneficial in improving mobility and managing tremors.
- Occupational therapy can provide valuable assistance in adapting daily tasks and environments to accommodate motor challenges. This includes modifying household layouts, selecting assistive devices, and optimizing workspaces to enhance independence and reduce fatigue.
- Speech therapy plays a critical role in managing communication difficulties. Speech therapists can help improve speech clarity, swallowing, and vocal volume, facilitating better communication and reducing social isolation.
Support Systems for Individuals with Parkinson’s
Building a strong support network is vital for emotional well-being and practical assistance. This includes family, friends, support groups, and healthcare professionals.
Learning about Parkinson’s disease is fascinating, but understanding its differences from other neurological conditions like myasthenia gravis vs ALS is equally important. For example, while Parkinson’s involves motor control issues, comparing it to conditions like myasthenia gravis vs ALS reveals distinct symptoms and underlying causes. Ultimately, delving into the specific facts about Parkinson’s disease helps us better appreciate the complexities of neurological disorders.
- Support groups offer a valuable platform for individuals with Parkinson’s and their caregivers to connect with others facing similar experiences. Sharing experiences, exchanging coping strategies, and receiving emotional support from peers can be profoundly beneficial.
- Family and friends can provide invaluable emotional and practical support. Encouraging open communication, actively listening to concerns, and offering assistance with daily tasks can significantly ease the burden on individuals with Parkinson’s.
- Healthcare professionals, including neurologists, physical therapists, occupational therapists, and speech therapists, are integral members of the support team. They provide expert guidance, develop personalized treatment plans, and offer ongoing support throughout the disease progression.
Lifestyle Adjustments for Managing Parkinson’s
Adopting healthy lifestyle habits can positively influence symptom management and overall well-being. A balanced diet, regular sleep patterns, and stress reduction techniques are crucial components.
- A balanced diet rich in fruits, vegetables, and whole grains can help maintain energy levels, manage weight, and support overall health. Consult with a registered dietitian to develop a personalized nutrition plan.
- Prioritizing adequate sleep is essential for restoring energy and improving cognitive function. Establishing a consistent sleep schedule, creating a relaxing bedtime routine, and ensuring a conducive sleep environment can contribute to better sleep quality.
- Stress management techniques, such as mindfulness exercises, yoga, or deep breathing, can help mitigate stress and anxiety, which can exacerbate Parkinson’s symptoms. Identifying personal stress triggers and developing effective coping mechanisms is vital.
Creating a Supportive Care Plan
A well-structured care plan can help individuals with Parkinson’s and their caregivers navigate the challenges effectively.
| Task | Responsibility | Timeline | Notes |
|---|---|---|---|
| Medication management | Individual with Parkinson’s and/or caregiver | Daily | Ensuring timely and accurate medication administration. |
| Exercise and physical therapy | Individual with Parkinson’s, caregiver, and therapist | Regular (e.g., weekly) | Scheduling and attending appointments, tracking progress. |
| Dietary management | Individual with Parkinson’s and/or caregiver | Daily | Planning and preparing meals, ensuring nutritional adequacy. |
| Social activities | Individual with Parkinson’s, family, friends, support groups | As needed | Maintaining social connections and engagement. |
Research and Advancements
Unveiling the mysteries of Parkinson’s Disease hinges on continuous research and innovation. Scientists are tirelessly pursuing a deeper understanding of the disease mechanisms, exploring potential therapeutic targets, and developing new and improved treatments. This relentless pursuit promises to improve the lives of those affected by Parkinson’s and potentially pave the way for a cure.
Current Research Efforts
Research efforts encompass a broad spectrum of approaches, from fundamental studies of the disease mechanisms to clinical trials evaluating novel therapies. These investigations involve numerous researchers, institutions, and organizations worldwide, united in their commitment to advancing knowledge and improving patient outcomes. Scientists are exploring various avenues, including genetic studies to identify susceptibility genes, examining environmental factors that might contribute to the disease, and developing advanced imaging techniques to better visualize and understand the brain changes associated with Parkinson’s.
Promising New Treatments and Therapies
Several promising new treatments and therapies are currently under investigation. These innovative approaches aim to address the underlying causes of the disease or alleviate its symptoms more effectively. One area of focus is the development of therapies that target specific proteins or pathways involved in the disease process. Other strategies involve using gene therapy to introduce beneficial genes or silencing disease-causing genes.
Furthermore, stem cell therapies are being explored as a potential way to replace damaged nerve cells.
Challenges and Opportunities in Parkinson’s Research
While significant progress has been made, challenges remain in Parkinson’s research. One major hurdle is the complexity of the disease, encompassing various subtypes and diverse patient responses to treatments. Another significant challenge is the lengthy and costly process of clinical trials, which often require substantial resources and time. However, there are exciting opportunities. The growing availability of advanced technologies, including sophisticated imaging techniques and sophisticated computational tools, provides unprecedented avenues for investigation and data analysis.
Improved understanding of the disease’s genetic and environmental components will lead to more personalized treatments and preventive strategies.
Progress in Understanding the Disease Mechanism
The understanding of Parkinson’s disease mechanisms is continually evolving. This table Artikels some key findings and their potential implications:
| Specific Findings | Potential Implications | Future Directions | Examples |
|---|---|---|---|
| Identification of specific protein aggregates (Lewy bodies) in the brain | Provides a potential target for therapies aimed at preventing or eliminating these aggregates. | Develop drugs that can selectively target and dissolve these aggregates without harming healthy brain tissue. | Developing drugs that target alpha-synuclein aggregation. |
| Discovery of genetic links to Parkinson’s | Allows for the identification of individuals at higher risk and potentially earlier diagnosis. | Development of genetic tests and personalized treatment strategies based on individual genetic profiles. | Genetic screening to identify individuals with a high probability of developing Parkinson’s. |
| Neuroinflammation is linked to disease progression. | Provides potential targets for anti-inflammatory therapies to slow or halt disease progression. | Investigate drugs that can reduce inflammation and the impact of immune cells on the brain. | Developing anti-inflammatory drugs specifically designed for Parkinson’s. |
| Dysfunction of dopamine pathways is central to the motor symptoms. | Suggests that therapies aimed at improving dopamine signaling could be effective in managing motor symptoms. | Further development of dopamine replacement therapies and alternative strategies to enhance dopamine production. | Developing new and improved dopamine replacement therapies. |
Impact on Families and Caregivers
Parkinson’s Disease isn’t just a challenge for the person diagnosed; it profoundly impacts the entire family unit. Caregivers, often spouses, children, or other relatives, shoulder a significant emotional and practical burden. Understanding these burdens and the available support systems is crucial for fostering a supportive environment.The disease’s progression often necessitates significant adjustments in daily routines, financial planning, and emotional well-being for everyone involved.
The challenges faced by families and caregivers are multifaceted, encompassing everything from the physical demands of caregiving to the emotional toll of witnessing a loved one’s decline. This section will delve into the specific difficulties and highlight strategies for navigating these challenges effectively.
Emotional Challenges for Families and Caregivers
The emotional toll of Parkinson’s Disease on caregivers is substantial. Caregivers experience a range of emotions, including anxiety, fear, sadness, and frustration, as they witness the gradual decline in their loved one’s abilities. This can lead to feelings of isolation and a sense of being overwhelmed. The emotional strain is compounded by the uncertainty surrounding the disease’s progression.The constant worry about the future, the need to adjust to changing needs, and the potential for a decrease in quality of life for the person with Parkinson’s can take a significant emotional toll on family members.
This can manifest as feelings of guilt, resentment, or a sense of loss of their former relationship.
Practical Challenges for Families and Caregivers
Beyond the emotional burden, Parkinson’s Disease presents a myriad of practical challenges. These challenges often center around managing daily tasks and ensuring the well-being of the person with Parkinson’s. This can include coordinating medical appointments, administering medication, managing finances, and providing personal care.The demands of caregiving can disrupt the caregiver’s own life, potentially impacting work, social activities, and personal well-being.
This can lead to a decline in the caregiver’s own health and well-being.
Communication and Emotional Support for Caregivers
Open communication within the family unit is paramount. Honest conversations about expectations, needs, and concerns can prevent misunderstandings and foster a supportive environment. Sharing the burden of caregiving amongst family members, where possible, can alleviate the strain on any one individual.Caregivers need to prioritize their own well-being. This includes seeking professional support, joining support groups, and taking time for self-care activities.
Encouraging caregivers to participate in these activities will lead to improved outcomes and resilience. Professional counseling or therapy can provide invaluable support in navigating the emotional challenges.
Caregiver Needs and Support Resources, Facts about parkinsons disease
| Caregiver Needs | Potential Support Resources | Strategies for Self-Care | Examples |
|---|---|---|---|
| Physical Demands | Home health aides, physical therapists, assistive devices | Regular exercise, healthy diet, adequate sleep | Hiring a home health aide to assist with bathing or meal preparation. |
| Financial Concerns | Social Security Disability Insurance, financial advisors, community resources | Budgeting, seeking financial counseling | Exploring options for financial assistance to cover medical expenses. |
| Emotional Well-being | Support groups, counseling, therapists, friends and family | Journaling, meditation, mindfulness, hobbies | Participating in support groups to connect with others facing similar challenges. |
| Time Management | Care coordination services, scheduling tools, family support | Prioritizing tasks, delegating responsibilities | Using online calendars or care coordination services to manage appointments and tasks. |
Caregiver needs are diverse and vary based on individual circumstances. The table above offers a framework for understanding the broad range of needs and potential resources. Remember that caregivers should not hesitate to seek help and support when needed. Finding appropriate support is key to preserving both the caregiver’s and the patient’s well-being.
Illustrative Case Studies
Understanding Parkinson’s Disease through real-life examples is crucial for comprehending the wide range of experiences and challenges faced by individuals affected by this neurodegenerative disorder. Each case presents a unique journey, shaped by varying symptom profiles, treatment responses, and long-term outcomes. These narratives highlight the importance of personalized care and the ongoing need for research and support.
Case Study Examples
The diverse nature of Parkinson’s Disease is vividly illustrated through individual case studies. Variations in symptom onset, progression rates, and treatment responses underscore the need for individualized care plans. These examples showcase the challenges and triumphs experienced by individuals living with this complex condition.
Patient Demographics, Symptoms, Treatments, and Outcomes
This table provides illustrative examples of Parkinson’s Disease cases, showcasing the variability in symptom presentation and progression. Note that these are simplified examples and real-life cases may have more nuanced details.
| Case Study | Patient Demographics | Symptoms | Treatments and Outcomes |
|---|---|---|---|
| Case 1 | 65-year-old male, retired teacher, with a family history of tremor disorders. | Tremor in the right hand, rigidity in the left arm, slowness of movement (bradykinesia), and balance problems. | Initiated on levodopa therapy, showing significant improvement in motor function for the first 5 years. Later, experienced fluctuations in motor control, including “on-off” periods, requiring adjustments to medication and non-pharmacological interventions like physical therapy. Developed mild cognitive impairment after 10 years. |
| Case 2 | 42-year-old female, lawyer, no family history of neurological disorders. | Progressive rigidity in both legs, postural instability, and speech difficulties. Experienced early onset, presenting with non-motor symptoms like sleep disturbances and depression. | Combination of levodopa, dopamine agonists, and deep brain stimulation (DBS) surgery. Showed good response to DBS in controlling motor symptoms, but experienced some side effects like dysphagia (difficulty swallowing). Maintained a high quality of life, successfully continuing her career with adjustments. |
| Case 3 | 78-year-old female, homemaker, with a history of hypertension and type 2 diabetes. | Bradykinesia, tremor in both hands, and gait disturbances. Presented with significant fatigue and difficulty with daily activities. | Levodopa therapy, along with physical therapy and occupational therapy, was initially successful in improving motor function and daily living skills. Experiences increasing fatigue and difficulty in performing daily activities after 7 years, eventually requiring assistance with activities of daily living. Participated in support groups, which provided crucial emotional support. |
Preventive Measures
While Parkinson’s disease currently lacks a definitive cure, understanding potential preventive strategies is crucial. Research continues to shed light on lifestyle choices that may reduce the risk of developing this debilitating neurodegenerative disorder. By adopting proactive measures, individuals can potentially mitigate their susceptibility to Parkinson’s.
Potential Protective Factors
Numerous factors may play a role in reducing the risk of Parkinson’s. These factors are often intertwined with overall health and well-being. A healthy lifestyle encompassing balanced nutrition, regular exercise, and stress management techniques can contribute significantly to a lower risk.
Lifestyle Factors
A balanced diet rich in fruits, vegetables, and antioxidants is believed to be beneficial. Antioxidants, such as those found in berries and dark leafy greens, are thought to help protect brain cells from oxidative stress, a process linked to neurodegenerative diseases. Regular physical activity, including cardiovascular exercise and strength training, is also considered crucial. Physical activity improves blood circulation and promotes overall brain health.
Stress management techniques, such as meditation or yoga, are also thought to potentially play a protective role. Sufficient sleep is essential for cognitive function and overall well-being.
Current Research on Prevention
Current research on Parkinson’s prevention is ongoing and multifaceted. Studies are exploring the potential role of specific dietary components, such as caffeine and certain vitamins, in reducing the risk. The impact of environmental exposures, including pesticides and industrial chemicals, is also under investigation. Some studies suggest that individuals who engage in regular physical activity and maintain a healthy weight may have a lower risk of developing Parkinson’s.
More research is needed to confirm these associations and establish causal relationships.
Actionable Steps
- Balanced Diet: Prioritize a diet rich in fruits, vegetables, and antioxidants. Limit processed foods, saturated fats, and excessive sugar intake.
- Regular Exercise: Engage in at least 150 minutes of moderate-intensity aerobic activity per week, combined with strength training exercises.
- Stress Management: Incorporate stress-reducing activities like meditation, yoga, or deep breathing exercises into your routine.
- Sufficient Sleep: Aim for 7-9 hours of quality sleep each night to support optimal brain function.
- Cognitive Stimulation: Engage in activities that challenge your brain, such as reading, puzzles, or learning new skills.
Outcome Summary
In conclusion, understanding Parkinson’s disease requires a holistic approach. It’s a condition that touches upon many facets of life, impacting individuals, families, and society as a whole. While challenges remain, ongoing research and supportive resources are vital in improving the lives of those affected. This exploration provides a starting point for further learning and engagement with this important topic.