15 types of headaches: Understanding the diverse nature of head pain is crucial for effective management. This guide delves into the specifics of each type, exploring their symptoms, potential causes, and treatment options. From the familiar tension headache to the more complex migraine, we’ll uncover the unique characteristics of each.
This detailed exploration will equip you with the knowledge needed to identify your own head pain and take informed steps toward better management. We’ll cover everything from the basics of headache definition to advanced treatment strategies.
Introduction to Headaches
Headaches, a common human experience, encompass a diverse range of conditions affecting the head and often characterized by pain. They vary significantly in intensity, duration, and location, impacting individuals in numerous ways. Understanding these nuances is crucial for effective management and treatment. This exploration delves into the general characteristics of headaches, their prevalence, historical context, and diverse classifications.Headaches are typically described as pain or discomfort in the head region.
This pain can manifest in various forms, from mild and throbbing to severe and debilitating. All types of headaches share the common element of head pain, although the underlying causes, symptoms, and treatment approaches differ. The sheer variety of headaches highlights the complexity of this widespread health concern.The prevalence of headaches is substantial, significantly impacting daily life for countless individuals.
Studies indicate that headaches are a leading cause of disability globally, affecting productivity, relationships, and overall well-being. The impact can be particularly significant for those experiencing chronic or severe headaches.Historical perspectives on headaches offer insights into how our understanding has evolved. Early civilizations often attributed headaches to supernatural causes, while modern medicine has identified a complex interplay of neurological, environmental, and physiological factors.
This understanding, based on scientific inquiry, has led to more effective diagnostic and treatment approaches.
Classification of Headaches
Headaches are broadly categorized into primary and secondary types. Primary headaches are not caused by an underlying medical condition, while secondary headaches are symptoms of another medical problem. This categorization helps in diagnosis and treatment planning.
Common Headache Types
This table Artikels some common types of headaches, their typical symptoms, and potential contributing factors. Understanding these characteristics can aid in identifying the specific type of headache being experienced.
| Headache Type | Common Symptoms | Potential Causes |
|---|---|---|
| Tension-type headache | Mild to moderate, often described as a band-like pressure or tightness around the head; may be accompanied by muscle stiffness or tenderness; often no nausea or vomiting. | Stress, anxiety, poor posture, eye strain, lack of sleep, dehydration, jaw clenching. |
| Migraine | Moderate to severe, throbbing pain, often unilateral (one-sided); frequently accompanied by nausea, vomiting, and sensitivity to light and sound; auras (visual disturbances) can precede the pain. | Genetics, hormonal fluctuations, stress, caffeine withdrawal, certain foods and drinks (e.g., aged cheeses, processed meats), sleep disturbances. |
| Cluster headache | Severe, intense, piercing pain, usually around one eye or temple; often accompanied by tearing, nasal congestion, and eyelid drooping on the affected side. Occur in clusters. | Genetics, environmental factors, stress, smoking. |
| Chronic daily headache | Headache occurring more than 15 days per month for 3 months or more; often tension-type-like pain. | Stress, underlying medical conditions (e.g., sinusitis), sleep disorders, medication overuse. |
Categorizing Headache Types
Headaches, a common ailment affecting millions worldwide, manifest in diverse forms and intensities. Understanding the different types of headaches is crucial for effective diagnosis and treatment. This section delves into the categorization of headache types, exploring their specific symptoms, underlying causes, and potential treatment approaches. Recognizing the particular characteristics of each type can lead to more accurate diagnoses and, consequently, more effective management strategies.Differentiating between various headache types is essential for appropriate medical intervention.
Accurate categorization allows healthcare professionals to pinpoint the root cause and tailor treatment plans accordingly. This detailed exploration of headache types will cover primary and secondary headaches, outlining their distinguishing features, symptom profiles, and potential triggers.
Primary Headaches
Primary headaches are not associated with an underlying medical condition. They are often triggered by factors like stress, diet, or environmental conditions. Understanding their diverse manifestations is crucial for effective management.
- Tension-type headaches: Characterized by a dull, pressing pain typically located on both sides of the head. The pain often feels like a band tightening around the head. Associated symptoms might include muscle tenderness in the neck and shoulders, and emotional stress often plays a significant role in triggering these headaches.
- Migraines: Known for their pulsating, moderate to severe pain, often concentrated on one side of the head. Migraine sufferers frequently experience accompanying symptoms such as nausea, vomiting, and extreme sensitivity to light and sound. The pain intensity can vary greatly between individuals.
- Cluster headaches: Marked by intense, sharp, and piercing pain that typically affects one side of the head. These headaches occur in clusters, often lasting for weeks or months, with periods of remission in between. They are frequently accompanied by tearing of the eye on the affected side, nasal congestion, and sweating.
Secondary Headaches
Secondary headaches are a symptom of an underlying medical condition. Identifying the underlying cause is paramount for appropriate treatment.
- Medication overuse headaches: These headaches arise from the overuse of pain relievers, often over-the-counter medications. This chronic use can disrupt the brain’s pain pathways, leading to recurring headaches. Consistent misuse of analgesics can trigger this type of headache, resulting in a cyclical pain pattern.
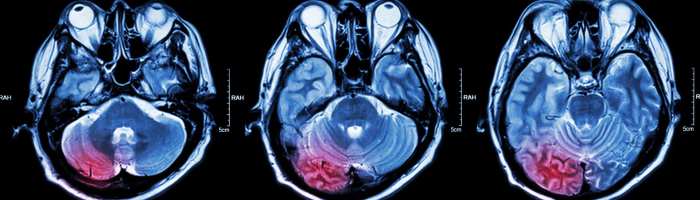
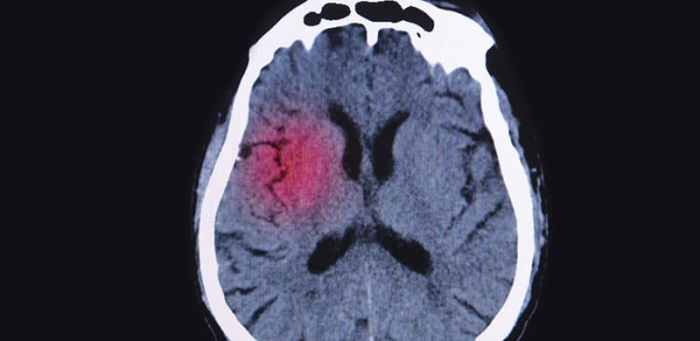
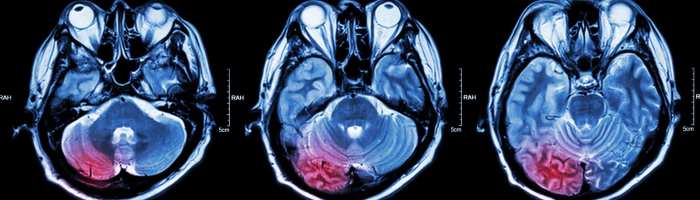
- Head injuries: Traumatic brain injuries, whether mild or severe, can lead to various types of headaches. The impact can cause inflammation and swelling in the brain, leading to head pain, along with other neurological symptoms.
- Brain tumors: Although less common, brain tumors can present with headaches, particularly if the tumor is growing and pressing against sensitive brain tissues. The pain can be constant or intermittent, varying in intensity. Often, a persistent headache coupled with other neurological symptoms could indicate the presence of a brain tumor.
- Meningitis: Inflammation of the membranes surrounding the brain and spinal cord (meningitis) can cause severe headaches. The headaches are often accompanied by fever, stiff neck, and sensitivity to light. A rapid onset of severe headache along with these additional symptoms is indicative of meningitis and warrants immediate medical attention.
Comparing Headache Types
| Headache Type | Location | Severity | Accompanying Symptoms | Potential Causes |
|---|---|---|---|---|
| Tension-type | Bilateral | Mild to Moderate | Muscle tenderness, stress | Stress, anxiety, poor posture |
| Migraine | Unilateral | Moderate to Severe | Nausea, vomiting, photophobia | Genetics, stress, hormonal changes |
| Cluster | Unilateral | Severe | Eye tearing, nasal congestion | Unknown, potential genetic predisposition |
| Medication overuse | Variable | Moderate to Severe | Headache frequency | Excessive use of pain relievers |
Symptoms and Diagnosis
Headaches, a common ailment, manifest in diverse ways, making accurate diagnosis crucial. Understanding the specific symptoms and diagnostic methods for each type of headache allows for appropriate treatment and management. This section delves into the common symptoms, diagnostic approaches, and variations in presentation among individuals.Diagnostic approaches for headaches often involve a combination of patient history, physical examination, and potentially, further investigations.
Accurate diagnosis relies on recognizing patterns in symptoms, their intensity, and frequency. A thorough evaluation by a healthcare professional is essential to determine the underlying cause and establish an effective treatment plan.
Common Symptoms of Headache Types
Recognizing the specific symptoms associated with different headache types is vital for proper diagnosis and management. Symptoms can range from mild discomfort to severe pain, impacting daily activities. Variations in symptom presentation exist among individuals, highlighting the importance of a personalized approach to diagnosis.
Ever wondered about the 15 different types of headaches? It’s fascinating how many variations there are! While exploring those different types, it got me thinking about how to handle skin issues after losing weight. Learning about methods to tighten skin after weight loss, like the ones discussed in this article how to tighten skin after weight loss , is key to feeling confident and comfortable.
Ultimately, understanding these various headache types is still my main focus.
- Tension-type headaches are often described as a dull, aching pain, typically located on both sides of the head. The pain intensity can range from mild to moderate, and the duration can vary from a few minutes to several hours.
- Migraines frequently feature throbbing or pulsing pain, often concentrated on one side of the head. Accompanying symptoms can include nausea, vomiting, and extreme sensitivity to light and sound.
- Cluster headaches are characterized by severe, intense pain, typically located around one eye or temple. The pain is often described as sharp or burning, and the episodes can last from 15 minutes to 3 hours.
- Sinus headaches result from inflammation of the sinuses. Pain is often focused around the forehead, temples, or cheeks and can be accompanied by nasal congestion, fever, and facial tenderness.
Diagnostic Methods for Various Headaches
Accurate diagnosis relies on a comprehensive approach that considers a patient’s medical history, physical examination findings, and potentially, additional tests. A detailed history about the headache’s characteristics (location, intensity, duration, frequency) is critical.
Ever wondered about the 15 different types of headaches? It’s a fascinating topic, but sometimes the underlying cause might be a bit more complex. For instance, if you’re taking medications like gabapentin, it’s important to research potential side effects, like weight changes. Finding out if gabapentin can lead to weight gain can be crucial for managing your health effectively.
Check out this resource to learn more: does gabapentin cause weight gain. Ultimately, understanding the different kinds of headaches is key to seeking the right treatment, but a holistic approach that considers potential medication side effects is important too. That said, learning about the various types of headaches is still a very interesting pursuit.
- The physical examination may include checking for signs of inflammation, fever, or other neurological abnormalities. This assessment can help rule out other potential causes for the pain.
- Diagnostic tools like imaging techniques (CT scans or MRIs) may be necessary to rule out structural abnormalities or other underlying medical conditions. These imaging procedures can provide detailed visualizations of the brain and surrounding tissues.
- Neurological examinations are conducted to assess reflexes, coordination, and other neurological functions. This helps to determine if the headache is related to any neurological dysfunction.
Symptom Variations Between Individuals
Headache symptoms can differ significantly among individuals, even for the same type of headache. Factors such as age, gender, and underlying health conditions can influence the experience. Pain intensity, location, and associated symptoms can vary, emphasizing the need for personalized diagnosis and treatment.
- For example, a migraine in one person might be accompanied by visual disturbances, while another might experience only throbbing pain.
- Furthermore, the severity and duration of symptoms can fluctuate based on individual susceptibility and triggers.
Symptom Summary Table
This table summarizes common symptoms, their severity, and duration for different headache types. Note that these are general guidelines, and individual experiences may vary.
| Headache Type | Symptoms | Severity | Duration |
|---|---|---|---|
| Tension-type headache | Dull, aching pain, often bilateral | Mild to moderate | Minutes to hours |
| Migraine | Throbbing/pulsating pain, often unilateral, with associated symptoms (nausea, vomiting, photophobia) | Moderate to severe | 4-72 hours |
| Cluster headache | Severe, intense pain, often around one eye or temple | Severe | 15 minutes to 3 hours |
| Sinus headache | Pain focused around forehead, temples, or cheeks, with nasal congestion, fever, facial tenderness | Moderate | Hours to days |
Causes and Risk Factors
Headaches, a common ailment, can stem from a multitude of factors. Understanding the potential causes and risk factors associated with different headache types is crucial for effective prevention and management. Identifying triggers and lifestyle influences can help individuals take proactive steps to reduce their headache frequency and improve their overall well-being.
Potential Causes of Different Headache Types
Various factors contribute to the development of various headache types. These factors range from environmental triggers to underlying medical conditions. Understanding these causes can help individuals identify potential triggers and adopt preventative measures.
- Tension-type headaches are frequently linked to stress, muscle tension in the neck and shoulders, poor posture, and eye strain. Sleep deprivation, dehydration, and even certain foods can also play a role.
- Migraines often have a complex interplay of genetic predisposition and environmental triggers. Stress, lack of sleep, changes in routine, certain foods (like aged cheeses or chocolate), and even weather fluctuations can act as potent triggers.
- Cluster headaches are characterized by intense, debilitating pain around one eye or temple. While the precise cause remains unclear, environmental factors such as smoke, alcohol, and changes in weather patterns can contribute to their onset.
- Medication overuse headaches result from the frequent or excessive use of pain relievers, such as over-the-counter analgesics. This can create a cycle of dependency, leading to chronic headaches.
Risk Factors Associated with Headache Types, 15 types of headaches
Certain risk factors increase an individual’s susceptibility to specific headache types. Recognizing these factors can help individuals take preventive measures.
- Tension-type headaches are more common in individuals with pre-existing anxiety or stress disorders, and those who experience prolonged periods of physical or mental strain.
- Migraines often run in families, suggesting a genetic component. Certain personality traits, such as perfectionism or heightened sensitivity to sensory stimuli, may also increase the risk. A history of head trauma can also be a significant risk factor.
- Cluster headaches tend to affect individuals in their 30s and 40s, although no definitive risk factors have been established. However, smoking and alcohol use are known triggers, increasing the risk of these headaches.
- Medication overuse headaches are directly linked to the frequent and excessive consumption of pain relievers. Individuals who self-medicate for headaches or other ailments may be at a higher risk.
Lifestyle Factors and Headache Frequency
Lifestyle choices play a significant role in the frequency and severity of headaches. Maintaining a healthy lifestyle can effectively reduce the risk and impact of headaches.
- A consistent sleep schedule, proper hydration, and a balanced diet are crucial for overall well-being and can significantly reduce headache frequency. Adequate hydration helps maintain proper bodily functions and prevent dehydration-related headaches.
- Stress management techniques, such as yoga, meditation, or deep breathing exercises, can effectively reduce stress-related tension-type headaches and migraines.
- Regular physical activity and exercise can improve circulation, reduce stress, and potentially lower the frequency of headaches. Maintaining a healthy weight can also contribute to overall well-being.
- Identifying and avoiding triggers, such as certain foods, environmental factors, or stress-inducing situations, can greatly reduce the likelihood of experiencing a headache.
Summary Table
| Headache Type | Potential Causes | Risk Factors | Preventive Measures |
|---|---|---|---|
| Tension-type | Stress, muscle tension, poor posture, eye strain, sleep deprivation, dehydration, certain foods | Anxiety, stress disorders, prolonged physical/mental strain | Stress management techniques, good posture, regular exercise, sufficient sleep, hydration, trigger avoidance |
| Migraine | Genetic predisposition, environmental triggers (stress, lack of sleep, food, weather), head trauma | Family history of migraines, certain personality traits, head trauma | Stress management, regular sleep, trigger avoidance, proper diet, hydration |
| Cluster | Environmental factors (smoke, alcohol, weather changes), unknown factors | Age (30s-40s), smoking, alcohol use | Avoid triggers, maintain healthy lifestyle, seek professional help |
| Medication overuse | Frequent or excessive use of pain relievers | Self-medication habits | Consult a doctor, identify alternative pain relief strategies, manage underlying pain conditions |
Treatment and Management
Treating headaches effectively involves a multifaceted approach tailored to the specific type and individual needs. Understanding the underlying causes and triggers is crucial for developing an effective management strategy. This includes both immediate pain relief and long-term preventative measures. Proper diagnosis and personalized treatment plans are vital to achieving optimal outcomes and improving quality of life.Effective management often involves a combination of over-the-counter medications, prescription therapies, and alternative approaches.
Addressing lifestyle factors and stress management techniques can significantly contribute to headache prevention and mitigation.
Over-the-Counter and Prescription Medications
Many headaches respond well to over-the-counter pain relievers, such as ibuprofen or acetaminophen. These medications are generally safe and effective for mild to moderate headaches, but their effectiveness varies depending on the headache type. For more severe or frequent headaches, prescription medications may be necessary. These medications often target specific pain pathways or underlying mechanisms. Examples include triptans, which are often effective for migraine headaches, and other specific medications designed to address specific headache types.
Alternative Therapies
Alternative therapies, such as acupuncture, biofeedback, and relaxation techniques, can be valuable adjuncts to conventional treatments. These methods can help manage underlying stress and tension, which are common triggers for certain headache types. Acupuncture, for example, involves inserting thin needles into specific points on the body, stimulating nerve pathways and potentially reducing pain signals. These therapies are often used in conjunction with other treatment methods to create a comprehensive approach.
Preventive Measures
Preventive measures are crucial for managing chronic headaches. Identifying and avoiding triggers, such as stress, certain foods, or environmental factors, can significantly reduce headache frequency and severity. Regular sleep hygiene, stress management techniques, and maintaining a healthy diet are all essential elements of a comprehensive prevention strategy. For example, keeping a headache diary can help identify patterns and triggers.
Treatment Options for Specific Headache Types
| Headache Type | Treatment Options | Potential Side Effects | Effectiveness Rates |
|---|---|---|---|
| Tension-type headaches | Over-the-counter pain relievers (ibuprofen, acetaminophen), relaxation techniques, stress management, biofeedback. | Mild gastrointestinal upset (with NSAIDs), drowsiness (with some medications). | Generally effective for mild to moderate cases. |
| Migraines | Triptans (e.g., sumatriptan), ergotamine, NSAIDs, CGRP inhibitors (e.g., fremanezumab). Preventive medications may include beta-blockers, antidepressants, or calcium channel blockers. | Nausea, vomiting, dizziness, or, in rare cases, more serious side effects with some medications. | Triptans can be highly effective for acute migraine attacks, but effectiveness varies between individuals. Preventive medications can significantly reduce frequency and severity. |
| Cluster headaches | Oxygen therapy, triptans, and other medications like verapamil. | Side effects vary depending on the medication, and may include nausea, dizziness, or more severe complications with some medications. | Oxygen therapy is often highly effective in acute cluster headache attacks, while other medications can reduce frequency and severity. |
| Other types (e.g., medication overuse headaches) | Reducing or eliminating the causative medication. Lifestyle changes, stress management, and other specific therapies may be needed. | Withdrawal symptoms if medication is abruptly stopped. | Success rates depend on the severity of the medication overuse and the patient’s response to treatment. |
Identifying and addressing underlying medical conditions, such as sinus infections or dental problems, can be crucial for successful treatment and management of headache pain.
Lifestyle Considerations
Headaches can be significantly influenced by lifestyle choices. Understanding how factors like stress, diet, sleep, and hydration impact headache frequency is crucial for effective management. By making conscious adjustments in these areas, individuals can often reduce the intensity and frequency of their headaches.
The Role of Stress Management
Stress is a powerful trigger for many headache types. Chronic stress can lead to muscle tension and vasoconstriction, both of which can contribute to headaches. Recognizing stress triggers and developing healthy coping mechanisms is paramount. Techniques such as meditation, deep breathing exercises, yoga, and spending time in nature can be valuable tools in managing stress and reducing headache frequency.
Prioritizing relaxation and downtime is equally important. Finding activities that bring a sense of calm and peace can help mitigate the impact of stress on headache susceptibility.
Healthy Dietary Habits
Dietary choices play a significant role in headache prevention. Certain foods and drinks can trigger headaches in susceptible individuals. Avoiding processed foods, sugary drinks, and excessive caffeine consumption can often help minimize headache frequency. A balanced diet rich in fruits, vegetables, and whole grains can provide essential nutrients and contribute to overall well-being, potentially reducing the likelihood of headaches.
Hydration is also critical, as dehydration can sometimes exacerbate headache symptoms.
Importance of Adequate Sleep
Adequate sleep is essential for overall health and can directly impact headache frequency. Sleep deprivation can lead to muscle tension and stress hormones, making individuals more susceptible to headaches. Aiming for 7-9 hours of quality sleep each night can significantly reduce the risk of headaches. Establishing a consistent sleep schedule and creating a relaxing bedtime routine can promote better sleep quality.
Creating a dark, quiet, and cool sleep environment is also beneficial.
Significance of Hydration
Proper hydration is critical for many bodily functions, including headache prevention. Dehydration can trigger or worsen headaches. Drinking plenty of water throughout the day is essential. Carry a reusable water bottle and sip on water regularly, especially during periods of activity or when experiencing a headache onset.
Lifestyle Adjustments and Headache Frequency
| Lifestyle Adjustment | Impact on Headache Frequency |
|---|---|
| Stress Management (meditation, yoga, relaxation techniques) | Potentially reduces headache frequency and intensity |
| Balanced Diet (fruits, vegetables, whole grains) | May reduce triggers and improve overall health |
| Adequate Sleep (7-9 hours) | Reduces risk of headaches due to sleep deprivation |
| Hydration (regular water intake) | Reduces risk of dehydration-related headaches |
| Avoidance of Headache Triggers (processed foods, caffeine, alcohol) | Reduces exposure to potential triggers |
When to Seek Medical Attention: 15 Types Of Headaches
Headaches, while a common ailment, can sometimes signal a more serious underlying health issue. Knowing when to seek immediate medical attention is crucial for ensuring prompt diagnosis and treatment, potentially preventing complications. Ignoring warning signs can delay necessary intervention, potentially impacting the outcome.
Urgent Situations Requiring Immediate Medical Attention
Certain headache characteristics necessitate immediate medical evaluation. These include sudden, severe headaches, especially if accompanied by other symptoms, or headaches that significantly deviate from a person’s usual pattern. Understanding these indicators is vital for timely intervention.
Warning Signs of Potential Serious Conditions
A sudden, severe headache, unlike a typical headache, can be a symptom of a serious medical issue. Several warning signs can indicate the need for immediate medical attention. These include:
- Sudden, severe headache accompanied by stiff neck, fever, or a rash.
- Headache accompanied by vision changes, numbness, weakness, or loss of coordination.
- Headache that develops suddenly and intensely, with no known cause or prior headache history.
- Headache associated with a recent head injury, even if seemingly minor.
- Headache that worsens rapidly or is significantly different from previous headaches.
- Headache that occurs with a fever, stiff neck, or other symptoms of infection.
Steps to Take if Experiencing a Sudden or Severe Headache
If you experience a sudden or severe headache, it’s essential to take immediate action. First, assess your surroundings and ensure your safety. Next, try to remain calm and assess the symptoms. Document any associated symptoms and the time the headache began.
- Stay hydrated: Drink plenty of fluids, as dehydration can sometimes worsen headaches.
- Lie down in a quiet, dark room: A calm environment can help alleviate discomfort.
- Seek immediate medical attention: If the headache is severe, sudden, or accompanied by concerning symptoms, contact emergency services or seek immediate medical attention.
Table of Situations Warranting Immediate Medical Intervention
The following table Artikels situations demanding immediate medical intervention and the appropriate actions to take:
| Situation | Actions |
|---|---|
| Sudden, severe headache with stiff neck, fever, or rash | Immediately contact emergency services or seek immediate medical attention. |
| Headache with vision changes, numbness, weakness, or loss of coordination | Immediately contact emergency services or seek immediate medical attention. |
| Severe headache with no known cause or prior history | Immediately contact emergency services or seek immediate medical attention. |
| Headache following a recent head injury, even a minor one | Seek immediate medical attention. |
| Headache that worsens rapidly or is significantly different from previous headaches | Seek immediate medical attention. |
| Headache with fever, stiff neck, or other infection-related symptoms | Seek immediate medical attention. |
Prevention Strategies

Preventing headaches involves a multifaceted approach that goes beyond simply treating symptoms. Proactive measures can significantly reduce the frequency and intensity of headaches, improving overall quality of life. Understanding triggers and implementing lifestyle adjustments are key components of effective headache prevention.Effective headache prevention hinges on identifying and managing potential triggers. This often requires careful observation of personal habits and environmental factors.
Ever wondered about the 15 different types of headaches? It’s fascinating how many variations there are! Sometimes, a nagging cough can trigger a headache, and choosing the right over-the-counter cough medications choosing over the counter cough medications can make a big difference in managing symptoms. But remember, understanding the different types of headaches is key to proper diagnosis and treatment.
By recognizing patterns and addressing the root causes, individuals can actively reduce their vulnerability to headaches. Stress management techniques also play a crucial role in headache prevention, as stress is frequently linked to increased headache frequency. These strategies, combined with appropriate lifestyle modifications, can lead to a substantial decrease in headache episodes.
Identifying and Managing Triggers
Headache triggers can vary significantly from person to person. Common triggers include stress, lack of sleep, certain foods and drinks, environmental factors, and changes in routine. Regularly documenting headache episodes and associated factors can aid in identifying patterns and pinpointing potential triggers. This proactive approach allows individuals to take preventive measures to minimize future headaches.
Stress Reduction Techniques
Stress is a significant contributor to various types of headaches. Incorporating stress reduction techniques into daily routines can effectively mitigate headache frequency. These techniques may include mindfulness exercises, meditation, deep breathing exercises, yoga, or engaging in hobbies that promote relaxation. Consistency in these practices is key to experiencing the full benefits.
Preventive Measures by Headache Type
- Tension-type headaches: Strategies to manage stress, such as regular exercise, adequate sleep, and relaxation techniques, can be highly effective. Maintaining a healthy diet and avoiding trigger foods, such as caffeine or alcohol, can also contribute to reducing tension headaches.
- Migraines: Identifying and avoiding triggers like specific foods, odors, weather changes, or stress is crucial. Maintaining a consistent sleep schedule, regular exercise, and stress management techniques can be vital. Ergonomic adjustments to posture and work habits can also help prevent migraines.
- Cluster headaches: While triggers for cluster headaches aren’t always completely understood, avoiding known triggers, such as smoking, alcohol, or changes in barometric pressure, is important. Lifestyle adjustments, such as maintaining a consistent sleep schedule and minimizing stress, can play a supportive role. Regular medical follow-up is also essential for managing cluster headaches effectively.
Lifestyle Considerations for Headache Prevention
Maintaining a healthy lifestyle significantly impacts headache frequency. Sufficient sleep, regular exercise, a balanced diet, and hydration are essential. Adequate sleep is particularly crucial for preventing headaches, as sleep deprivation can often trigger or worsen various types of headaches. Regular exercise can reduce stress and improve overall well-being, contributing to fewer headache episodes. A balanced diet rich in fruits, vegetables, and whole grains provides essential nutrients, while staying hydrated keeps the body functioning optimally.
These lifestyle factors are fundamental components of a comprehensive headache prevention strategy.
Examples of Preventive Measures and Their Effectiveness
Numerous preventive measures can be implemented to reduce the risk of headaches. Stress management techniques, like meditation or yoga, can significantly reduce the frequency and intensity of tension-type headaches. Avoiding trigger foods or environmental factors can help prevent migraines. For cluster headaches, maintaining a consistent sleep schedule and avoiding triggers can be effective. The effectiveness of each measure can vary depending on individual factors and the type of headache.
Consistency in implementing these measures is key to achieving long-term benefits.
Illustrative Case Studies
Understanding headaches requires more than just knowing the types. Real-world examples of how headaches manifest, progress, and respond to treatment offer valuable insights. These case studies illustrate the diverse presentations and outcomes associated with various headache disorders, providing a tangible connection between the theoretical and the practical.Case studies, meticulously documented, offer a deeper understanding of individual experiences with headaches.
They showcase the nuances of symptoms, the challenges of diagnosis, and the effectiveness of various treatment strategies. Each scenario, though unique, can offer patterns and insights that help us better understand and manage headaches in patients.
Common Scenarios of Tension-Type Headaches
Tension-type headaches, often described as a band-like tightness across the head, are frequently triggered by stress and poor posture. These headaches typically present with a mild to moderate intensity and are usually not accompanied by nausea or sensitivity to light or sound.
- Case Study 1: Sarah, a 35-year-old office worker, experiences recurring tension-type headaches. Her symptoms typically begin with a mild, dull ache in her temples and forehead, progressing to a constant tightness across her head. The pain is often aggravated by prolonged periods of sitting at her desk, poor posture, and high levels of stress at work. She found relief through relaxation techniques, including deep breathing exercises and mindfulness practices, coupled with over-the-counter pain relievers.
This demonstrates a successful approach to managing chronic tension-type headaches.
- Case Study 2: Mark, a 48-year-old accountant, experiences frequent tension headaches that intensify when he works on complex spreadsheets. His symptoms are characterized by a throbbing, band-like sensation around his head, accompanied by mild neck stiffness. He found that incorporating regular neck stretches and ergonomic adjustments to his workspace significantly reduced the frequency and severity of his headaches.
Migraine Case Studies
Migraines are often characterized by severe throbbing pain, typically on one side of the head, accompanied by nausea, vomiting, and sensitivity to light and sound.
- Case Study 3: Emily, a 28-year-old student, experiences migraine attacks that are preceded by visual auras. Her headaches are severe and debilitating, often requiring her to miss classes. After identifying triggers like caffeine withdrawal and stress, she implemented a consistent sleep schedule and a stress management plan, which significantly reduced the frequency and intensity of her migraines.
- Case Study 4: David, a 32-year-old lawyer, suffers from debilitating migraines. His attacks are accompanied by nausea and vomiting, which often prevent him from performing his job duties. He found that preventive medications, combined with biofeedback therapy, have successfully reduced the frequency and severity of his migraines.
Illustrative Table of Case Studies
| Case Study | Headache Type | Symptoms | Treatment | Outcome |
|---|---|---|---|---|
| Case Study 1 | Tension-type | Mild to moderate band-like tightness, aggravated by stress and posture | Relaxation techniques, pain relievers | Reduced frequency and severity |
| Case Study 2 | Tension-type | Throbbing, band-like sensation, neck stiffness, aggravated by work | Neck stretches, ergonomic adjustments | Reduced frequency and severity |
| Case Study 3 | Migraine | Severe throbbing pain, visual aura, nausea, sensitivity to light and sound | Consistent sleep schedule, stress management, preventive medication | Reduced frequency and intensity |
| Case Study 4 | Migraine | Debilitating throbbing pain, nausea, vomiting | Preventive medications, biofeedback therapy | Reduced frequency and severity |
Resources and Support

Navigating the world of headaches can feel isolating. Fortunately, there are numerous resources and support systems available to help you understand, manage, and cope with these often debilitating conditions. This section will explore the various avenues for support, from online communities to professional organizations and personal connections.Reliable resources provide crucial information, allowing you to make informed decisions about your health.
Support groups offer a sense of community and shared experience, while online platforms connect you with others facing similar challenges. Recognizing the significance of these resources and building a support network can be a powerful tool in managing headaches effectively.
Reliable Headache Information Resources
Understanding headaches requires access to accurate and reliable information. A wealth of resources exist to guide you through various aspects of headache management. These resources range from reputable websites to informative books. Consulting these sources can provide valuable insights into understanding your specific type of headache and the available treatment options.
- The National Headache Foundation (NHF): A leading organization dedicated to headache research and support. Their website offers a wealth of information, including articles, educational materials, and a directory of headache specialists.
- The American Migraine Foundation (AMF): Focused on migraine research, treatment, and support. They provide valuable resources on migraine management, including educational materials, support groups, and information on current research.
- The Mayo Clinic: A well-regarded medical institution offering comprehensive information on various health conditions, including headaches. Their website contains detailed explanations of different headache types, potential causes, and treatment strategies.
Support Groups and Organizations
Connecting with others who share similar experiences can provide invaluable support and a sense of community. Support groups offer a platform for sharing coping strategies, discussing challenges, and gaining encouragement.
- Headache support groups: Many local hospitals and community centers host support groups for individuals experiencing headaches. These groups offer a space for open communication and sharing of experiences with others facing similar challenges. You can find these groups through your local medical center, community centers, or online.
- Online support communities: Online forums and social media groups dedicated to headaches offer a virtual space for support and connection. These platforms allow individuals to share their experiences, ask questions, and gain insights from others facing similar challenges. Be mindful of the diversity of information found in online forums and verify it with a medical professional if needed.
Seeking Support from Family and Friends
Building a strong support network is vital in managing any health condition, including headaches. Open communication with family and friends is crucial. They can provide emotional support, help with daily tasks, and offer practical assistance.
- Open communication: Discussing your experiences with family and friends can foster understanding and support. Explain how headaches impact your daily life and seek their help in managing your responsibilities.
- Practical assistance: Ask for help with tasks that might be difficult to manage when experiencing a headache. This could include household chores, childcare, or transportation.
Online Resources and Communities
The internet offers a vast array of online resources and communities dedicated to headache support. These platforms provide access to information, support groups, and connections with others experiencing similar issues.
- Online forums and message boards: These platforms allow individuals to share their experiences, ask questions, and connect with others. Be cautious about the credibility of information found online, and always consult with a healthcare professional before making any decisions based on online information.
- Social media groups: Social media groups can be valuable for connecting with others who understand the challenges of living with headaches. These groups often offer a space for sharing experiences and providing mutual support.
Table of Resources and Support Groups
| Headache Type | Reputable Resources | Support Groups |
|---|---|---|
| Migraine | American Migraine Foundation, Mayo Clinic | Online Migraine Support Groups, Local Support Groups |
| Tension-type headache | National Headache Foundation, Mayo Clinic | Online Tension Headache Support Groups, Local Support Groups |
| Cluster headache | National Headache Foundation, Mayo Clinic | Online Cluster Headache Support Groups, Local Support Groups |
| Other headache types (e.g., chronic daily headache, etc.) | National Headache Foundation, Mayo Clinic | Online Support Groups for specific headache type, Local Support Groups |
Last Word
In conclusion, understanding the 15 types of headaches is a significant step toward effective pain management. By recognizing the specific symptoms, causes, and treatment options for each type, you can proactively address your head pain and improve your overall well-being. This comprehensive guide provides a valuable resource for anyone experiencing headaches, empowering you to make informed decisions about your health.