Is osteoporosis a disability? This question delves into the complex interplay between bone health, medical criteria, and societal impacts. We’ll explore the medical definition of osteoporosis, its effects on daily life, and how it intersects with legal frameworks and personal experiences. The discussion also considers osteoporosis in comparison to other bone-related conditions and the future of research in this area.
Osteoporosis, a condition characterized by weakened bones, is often associated with increased risk of fractures. This overview will examine the different stages of osteoporosis, potential physical limitations, and how these impact daily activities. We’ll also look at the social and functional effects, including challenges in work, education, and social interactions.
Defining Osteoporosis
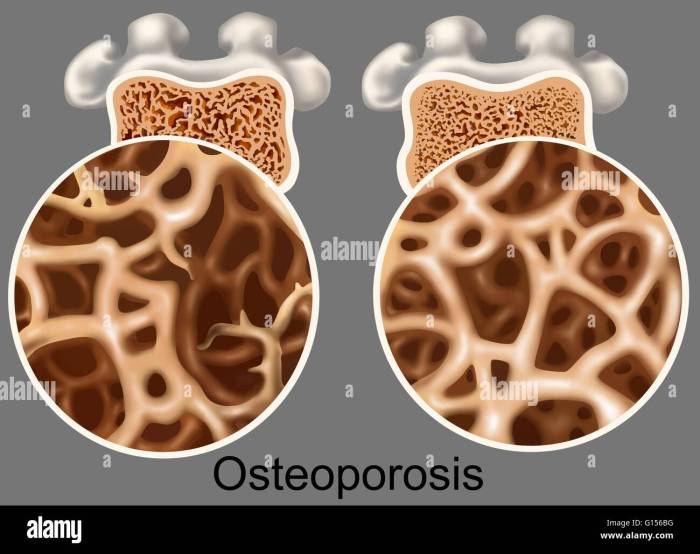
Osteoporosis is a silent disease that gradually weakens bones, making them more prone to fractures. It’s often called the “silent thief” because the bone loss occurs without noticeable symptoms until a fracture happens. Understanding the various stages, risk factors, and characteristics of osteoporosis is crucial for prevention and effective management.
Defining Osteoporosis: A Detailed Look
Osteoporosis is a skeletal disorder characterized by compromised bone strength, increasing the risk of fractures. This is primarily due to a decrease in bone density and the deterioration of bone tissue. Bone density is a measure of the mass of bone tissue per unit volume. A decrease in bone density makes bones fragile and susceptible to fractures, even from minor falls or everyday stresses.
Stages of Osteoporosis
Understanding the progression of osteoporosis helps in determining appropriate interventions. Different stages reflect varying degrees of bone loss.
| Stage | Bone Density | Symptoms | Risk Factors |
|---|---|---|---|
| Normal Bone Density | Bone density within the normal range for age and gender. | Typically no symptoms. | Genetics, diet rich in calcium and vitamin D, regular exercise, no smoking or excessive alcohol consumption. |
| Low Bone Mass (Osteopenia) | Bone density is lower than normal, but not yet severely low. This is considered a precursor to osteoporosis. | Typically no symptoms. However, some individuals may experience bone pain or discomfort. | Genetics, family history of osteoporosis, insufficient calcium and vitamin D intake, low body weight, smoking, excessive alcohol consumption, lack of exercise, certain medications (e.g., steroids). |
| Osteoporosis | Significant decrease in bone density, resulting in a higher risk of fractures. | Often no noticeable symptoms until a fracture occurs. Some individuals may experience back pain, loss of height, or a stooped posture. | Genetics, family history of osteoporosis, age (especially after menopause in women), certain medical conditions (e.g., hyperthyroidism, rheumatoid arthritis), certain medications (e.g., corticosteroids), low body weight, lack of exercise, insufficient calcium and vitamin D intake, smoking, excessive alcohol consumption, lack of estrogen (in postmenopausal women). |
| Severe Osteoporosis | Extremely low bone density, greatly increasing the risk of fractures. | Similar symptoms to osteoporosis, but the risk of fractures is significantly higher. Individuals may experience multiple fractures. | Similar risk factors as osteoporosis, but often compounded by pre-existing conditions and lifestyle choices. |
Common Risk Factors for Osteoporosis
Various factors can increase the likelihood of developing osteoporosis. Understanding these risk factors is crucial for preventive measures.
While osteoporosis itself might not be considered a disability in all cases, the impact it has on daily life can certainly be debilitating. Think about how a chronic condition like osteoporosis could affect your ability to live independently, especially considering recent advances in treatments like covid 19 and flu free test to treat that focus on combating other debilitating diseases.
Ultimately, whether or not it’s classified as a disability depends on individual circumstances and the severity of the condition.
- Genetics: Family history of osteoporosis significantly increases the risk. Individuals with a family history may experience bone loss at an earlier age and at a faster rate compared to those without a family history.
- Age: Bone density naturally decreases with age. Post-menopausal women are particularly at risk due to the decrease in estrogen levels. Men also experience bone loss with age, but at a slower rate.
- Gender: Women are at higher risk of developing osteoporosis than men, especially after menopause.
- Body Composition: Low body weight and a lack of muscle mass can contribute to osteoporosis.
- Lifestyle Factors: Smoking, excessive alcohol consumption, lack of exercise, and a diet deficient in calcium and vitamin D increase the risk.
- Medical Conditions: Certain medical conditions, such as hyperthyroidism, rheumatoid arthritis, and celiac disease, can increase the risk of osteoporosis.
- Medications: Certain medications, such as corticosteroids, can increase bone loss.
Medical Perspective on Disability Status
Osteoporosis, a condition characterized by weakened bones, can significantly impact a person’s daily life. While not always considered a disability, the degree of physical limitation it causes can vary greatly from individual to individual. Understanding the medical criteria for assessing disability is crucial to comprehending how osteoporosis fits into this framework. This section explores the medical perspective, focusing on the potential physical limitations and how they are evaluated.
Medical Criteria for Disability Assessment, Is osteoporosis a disability
Medical professionals use various criteria to evaluate disability. These criteria often involve assessing functional limitations, including the ability to perform activities of daily living (ADLs). Key components of this evaluation often include: the severity of bone loss, the presence of fractures, and the impact on mobility and overall physical function. The specific criteria and procedures can vary based on the country or region and the specific healthcare system in place.
Potential Physical Limitations Associated with Osteoporosis
Osteoporosis significantly increases the risk of fractures, particularly in the spine, hips, and wrists. These fractures can lead to a multitude of physical limitations. Reduced bone density compromises the structural integrity of the skeleton, potentially impacting posture and balance. This can manifest as chronic back pain, stooped posture (kyphosis), and an increased risk of falls. Fractures can also result in pain, loss of mobility, and reduced independence.
Impact of Osteoporosis on Daily Activities and Mobility
Osteoporosis can hinder a person’s ability to perform daily tasks. For example, individuals may experience difficulty with tasks like getting dressed, walking, climbing stairs, or lifting objects. Reduced mobility can further restrict participation in social activities and work. The severity of these limitations depends on the extent of bone loss, the presence of fractures, and individual factors like age, overall health, and support systems.
A person with multiple fractures might have more pronounced limitations than someone with only one or no fractures.
Evaluation of Limitations for Disability Status
Medical professionals evaluate limitations related to osteoporosis by considering several factors. This includes a thorough physical examination, including bone density scans (DEXA scans) and X-rays to identify fractures and assess bone density. Clinical interviews assess the impact of osteoporosis on ADLs, mobility, and overall quality of life. Furthermore, questionnaires designed to measure functional ability and pain levels are used to quantify the degree of limitation.
While osteoporosis itself might not always be considered a disability, the symptoms and limitations it can cause can significantly impact daily life. For instance, understanding the various symptoms of lung nodules, their potential causes, and how they’re diagnosed is crucial, as some underlying conditions can contribute to both lung issues and bone density problems. Exploring resources like lung nodules symptoms causes and diagnosis can offer a more comprehensive picture of the potential connections between health conditions.
Ultimately, whether or not osteoporosis constitutes a disability depends on the individual’s specific situation and the severity of their condition.
These assessments are crucial in determining the extent to which osteoporosis affects a person’s ability to function independently.
Contrasting Osteoporosis Symptoms with Disability Criteria
| Osteoporosis Symptoms | Disability Criteria (Illustrative Example) |
|---|---|
| Bone pain, particularly in the spine, hips, and wrists | Limitations in mobility, restricted movement in daily activities, inability to perform essential self-care tasks |
| Increased risk of fractures | Inability to independently perform tasks essential for living, requiring assistance with activities of daily living |
| Reduced bone density | Significant functional impairment that restricts participation in work, education, and social activities |
| Stooped posture (kyphosis) | Limitations in mobility and posture that significantly impair the ability to perform daily activities and participate in social activities |
| Loss of height | Limited ability to perform essential self-care tasks independently, requiring substantial assistance |
Social and Functional Impacts
Osteoporosis’s impact extends far beyond the medical realm. It significantly affects a person’s quality of life, impacting social interactions, daily activities, and overall independence. Understanding these social and functional consequences is crucial for comprehensive care and support.
Social Impacts on Relationships
Osteoporosis can create challenges in social interactions. The fear of falling and the resulting pain and limitations can make individuals hesitant to participate in social activities. This can lead to feelings of isolation and loneliness, potentially impacting relationships with friends and family. For example, a person with osteoporosis might avoid outings with friends due to concerns about falls, or they might find it difficult to keep up with active hobbies, affecting shared experiences.
Reduced mobility can also impact the ability to visit loved ones, thus straining familial relationships.
Impact on Participation in Activities
Osteoporosis directly impacts a person’s ability to engage in various activities. Work, education, and leisure activities all become more challenging. Tasks requiring significant physical exertion, or those involving the risk of falls, become difficult or impossible. For example, a teacher might find it increasingly hard to stand and move around for extended periods, potentially affecting their ability to teach effectively.
Or, a construction worker might be unable to continue their work due to the risk of injury from falls.
Reduced Independence and Support Needs
As osteoporosis progresses, the need for support and assistance often increases. Daily tasks that were once easily performed become more demanding, requiring significant help. This can lead to a reduced sense of independence and a reliance on others for support. For instance, a person with osteoporosis may need help with household chores like grocery shopping, or they may need assistance with dressing and bathing.
Examples of Challenging Daily Tasks
The following table illustrates how osteoporosis can affect various daily tasks:
| Task | Difficulty Level | Support Needed |
|---|---|---|
| Walking long distances | High | Possible assistance with walking aids, like walkers or canes. |
| Carrying groceries | Medium | Potential for assistance with bags or help carrying items. |
| Climbing stairs | High | Assistance or using stairlifts may be necessary. |
| Lifting heavy objects | Very High | Significant support from another person is required. |
| Dressing | Medium | Assistance with putting on certain clothing items, especially those that are difficult to reach. |
| Bathing | High | Possible need for assistance with bathing or using a chair lift. |
| Cooking | Medium | Adapting cooking methods, using assistive devices, or having help with certain tasks. |
Legal and Policy Considerations: Is Osteoporosis A Disability
Defining osteoporosis as a disability isn’t solely about medical diagnoses; it’s deeply intertwined with legal frameworks and social policies. Different jurisdictions have varying standards for disability, impacting how osteoporosis fits into those frameworks. Understanding these legal nuances is crucial for navigating the support systems available to individuals affected by this condition.
Legal Frameworks Defining Disability
Various jurisdictions employ different legal frameworks to define disability. These frameworks often encompass physical limitations, cognitive impairments, and mental health conditions. The criteria for disability recognition often include the severity and duration of limitations, along with their impact on daily life activities. This multifaceted approach is crucial for ensuring a comprehensive understanding of the individual’s needs.
Osteoporosis Meeting Disability Criteria
Osteoporosis, while not always immediately apparent, can significantly impact a person’s ability to perform daily tasks. Severe osteoporosis can lead to fractures, chronic pain, reduced mobility, and decreased independence. These limitations can potentially meet the criteria of disability in various jurisdictions, particularly when the impact on daily activities is substantial. For example, frequent falls, pain restricting movement, and difficulty with self-care tasks can all contribute to a disability determination.
Policies and Legislation Related to Disability and Health Conditions
Many countries have legislation designed to support individuals with disabilities. These policies encompass areas like housing, employment, and transportation. Examples include accessible housing requirements, workplace accommodations, and public transportation modifications. These measures are aimed at ensuring equal opportunities and social inclusion for people with disabilities. For instance, the Americans with Disabilities Act (ADA) in the United States has specific provisions related to accessibility, which are essential for individuals with osteoporosis.
Accessibility Requirements for People with Osteoporosis
Accessibility is a key component of supporting people with osteoporosis. It encompasses a broad range of factors, from building design to transportation systems. Accessibility standards typically include features such as ramps, wider doorways, accessible restrooms, and elevators. These features are essential to maintain independence and mobility.
Examples of Specific Legislation and Accessibility Standards
Numerous pieces of legislation address accessibility needs. For example, the Americans with Disabilities Act (ADA) in the United States mandates accessible design features in public spaces. This includes provisions for ramps, elevators, and accessible entrances, impacting businesses, transportation, and public accommodations. Similar legislation exists in other countries, aiming to ensure that individuals with osteoporosis can access essential services and participate fully in society.
Furthermore, some countries have specific policies aimed at supporting older adults with health conditions like osteoporosis, ensuring they can remain in their homes and communities safely and comfortably.
Patient Experiences and Perspectives
Living with osteoporosis is more than just a medical diagnosis; it’s a deeply personal journey impacting every aspect of daily life. Patients experience a wide range of physical, emotional, and social challenges that often go beyond the immediate effects of bone loss. Understanding these experiences is crucial for developing effective support systems and policies that address the needs of those affected.
Perceptions of Disability
Osteoporosis can significantly impact an individual’s sense of self and ability to participate fully in society. Many patients perceive their condition as a disability, not just because of physical limitations, but also due to the anxieties and uncertainties surrounding its progression and potential complications. This perception is shaped by factors such as the severity of bone loss, the presence of pain, and the individual’s personal expectations and social environment.
A feeling of vulnerability and dependence can develop, affecting self-esteem and overall well-being.
While osteoporosis itself might not be considered a disability in all cases, the impact it has on daily life for some is undeniable. Managing the condition often involves a complex interplay of medical treatments and lifestyle adjustments, including careful consideration of over-the-counter medications. For older adults, understanding OTC drug safety is crucial, as interactions and side effects can be more pronounced.
This highlights the importance of careful medical guidance when navigating the complexities of osteoporosis and related health concerns.
Impact on Daily Life and Quality of Life
Osteoporosis affects daily activities in numerous ways. Pain and reduced mobility can limit movement, making tasks like walking, climbing stairs, or even getting dressed more challenging and time-consuming. Fractures, a common complication, can lead to long-term pain, reduced functionality, and the need for assistive devices. The impact extends beyond physical limitations; participation in social activities, hobbies, and work may be affected, leading to decreased quality of life and a feeling of isolation.
Individuals may experience a loss of independence and a sense of decreased control over their lives.
Emotional and Psychological Impact
The diagnosis and management of osteoporosis can have a profound emotional and psychological toll. Fear of future fractures, anxiety about the progression of the disease, and concerns about the impact on personal relationships can lead to feelings of stress, depression, and isolation. The loss of independence and the need for ongoing medical care can contribute to a sense of vulnerability and powerlessness.
It is essential to acknowledge and address these emotional aspects to support patients in coping with the challenges of osteoporosis.
Patient Survey
Gathering direct insights from individuals living with osteoporosis is crucial for understanding their experiences and needs. The following survey aims to provide valuable data to improve support systems and develop more effective strategies to manage the condition.
| Question Type | Question | Response Options |
|---|---|---|
| Multiple Choice | How would you describe the impact of osteoporosis on your daily life? |
|
| Open-Ended | Describe any emotional or psychological challenges you face due to osteoporosis. | Free text response |
| Multiple Choice | How would you rate your quality of life before and after diagnosis with osteoporosis? |
|
| Multiple Choice | Do you feel that osteoporosis limits your participation in social activities? |
|
| Open-Ended | What kind of support or resources would be most helpful to you in managing your osteoporosis? | Free text response |
Differentiating Osteoporosis from Other Bone-Related Conditions
Osteoporosis, a condition characterized by weakened bones, often gets confused with other bone-related issues. Understanding the nuances between osteoporosis and conditions like osteopenia, Paget’s disease, or even some types of arthritis is crucial for proper diagnosis and effective treatment. This exploration will delve into the key differences, highlighting symptoms, treatments, and the varying impacts on daily life.
Comparison of Osteoporosis with Other Bone-Related Conditions
Differentiating osteoporosis from other bone-related conditions requires a careful analysis of symptoms, diagnostic tests, and the specific characteristics of each disease. A thorough medical evaluation is essential to establish an accurate diagnosis. This comparison aims to provide a clear understanding of the distinctions.
- Osteopenia: Osteopenia is a precursor to osteoporosis, characterized by lower bone density than normal but not yet at the severe levels seen in osteoporosis. Symptoms are often absent in the early stages. Treatment focuses on lifestyle modifications to enhance bone health, including diet and exercise, and potentially medications to slow bone loss. The impact on daily life can vary, depending on the severity of the condition.
Osteopenia is typically diagnosed through bone density testing (DEXA scan), and if left untreated, it can progress to osteoporosis.
- Paget’s Disease of Bone: Paget’s disease is a chronic condition where bone tissue is broken down and reformed more quickly than normal. This leads to weakened and misshapen bones. Symptoms can include pain, especially in the affected bones, and deformity. Treatment usually involves medications that slow the rate of bone turnover. The impact on daily life can vary significantly depending on the affected areas and severity of the disease.
Diagnosis is made through blood tests, X-rays, and bone scans.
- Rheumatoid Arthritis: While not directly a bone disease, rheumatoid arthritis can cause bone erosion and loss, especially in joints. Symptoms typically include inflammation, pain, and stiffness in multiple joints. Treatment often includes medications to manage inflammation and slow joint damage. The impact on daily life can range from mild to severe, depending on the extent of joint involvement.
A key distinction is that rheumatoid arthritis primarily affects the joints, whereas osteoporosis affects the entire bone structure.
Distinguishing Osteoporosis from Osteopenia
Osteopenia and osteoporosis are closely related but distinct conditions. Both involve a decrease in bone density, but the degree of decrease determines the classification. Osteopenia signifies lower-than-normal bone density, while osteoporosis represents a significant loss of bone mass, making bones fragile and susceptible to fractures.
Osteoporosis is defined as a bone mineral density (BMD) 2.5 standard deviations below the mean for young adult women.
A key difference lies in the diagnostic criteria, with osteopenia often being a precursor to osteoporosis, and thus a preventive measure for osteoporosis is necessary. Bone density testing (DEXA scan) is used to measure bone mineral density and assess the risk of fractures.
Case Studies: Illustrative Examples
While general comparisons are helpful, real-life examples provide a richer understanding. It’s important to note that individual experiences with these conditions vary greatly.
- Patient A (Osteoporosis): A 65-year-old woman experienced a painful fracture in her hip after a minor fall. Bone density testing revealed severe osteoporosis. Treatment involved medication to increase bone density and physical therapy to improve mobility. The patient’s daily life was significantly impacted, requiring assistance with daily activities.
- Patient B (Osteopenia): A 50-year-old woman with osteopenia was identified through routine screening. She made lifestyle changes, focusing on calcium-rich foods and weight-bearing exercises, and was monitored closely. The patient’s lifestyle remained largely unaffected, but ongoing monitoring and preventive measures were crucial.
Comparison Table
| Characteristic | Osteoporosis | Osteopenia | Paget’s Disease | Rheumatoid Arthritis |
|---|---|---|---|---|
| Bone Density | Significantly low | Lower than normal | Abnormal bone remodeling | Joint erosion, bone loss in affected joints |
| Symptoms | Pain, fractures, loss of height | Often asymptomatic | Pain, deformity, increased risk of fractures | Inflammation, pain, stiffness in joints |
| Treatment | Medications, lifestyle changes | Lifestyle changes, potential medications | Medications to slow bone turnover | Medications to manage inflammation, physical therapy |
Future Trends and Research
Osteoporosis, a condition affecting millions worldwide, continues to be a subject of intense research. Advancements in understanding its mechanisms, coupled with innovative treatment strategies, offer hope for improved outcomes and a better quality of life for those affected. The focus is shifting towards personalized approaches, targeting specific risk factors and individual needs.Ongoing research is vital in tackling the multifaceted challenges posed by osteoporosis.
This includes exploring new avenues for prevention, more effective treatments, and improving the long-term management of the condition, with a significant emphasis on preventing disability.
Ongoing Research on Osteoporosis and Disability
Research into osteoporosis’s impact on disability is crucial for developing targeted interventions. Researchers are exploring the relationship between bone density loss, falls, and subsequent disability, including the development of tools for early detection of individuals at high risk. This includes investigating genetic predispositions and environmental factors contributing to bone fragility.
Advancements in Treatment and Management Strategies
Significant progress is being made in the development and refinement of osteoporosis treatments. These advancements aim to enhance bone density, reduce the risk of fractures, and minimize the impact on patients’ daily lives. A key area of research is the exploration of novel drugs with improved safety profiles and greater efficacy. Moreover, ongoing studies focus on the optimal timing and duration of treatments to maximize benefits while minimizing potential side effects.
Innovative Approaches to Improve Quality of Life
Innovative approaches are being explored to address the non-pharmacological aspects of osteoporosis management. This includes the development of targeted exercise programs, tailored to individual needs and abilities, to improve bone health and maintain muscle strength. Furthermore, research is focusing on the creation of assistive devices and technologies to enhance mobility and independence for individuals with osteoporosis.
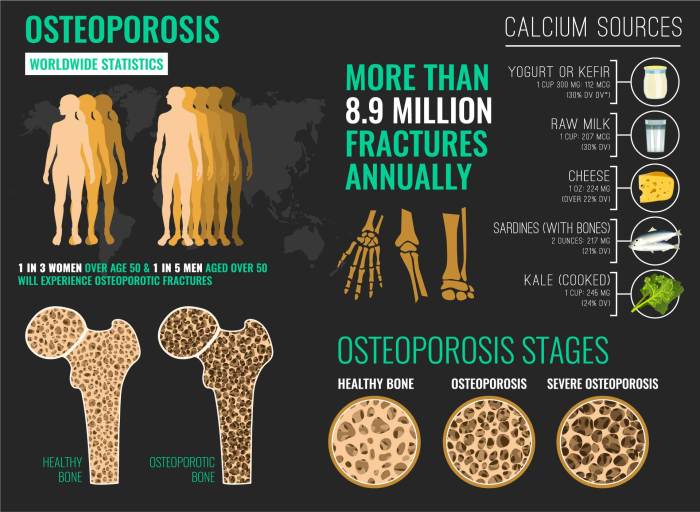
Prevalence and Projected Future Impact of Osteoporosis
The global prevalence of osteoporosis is substantial, and projections indicate a continued rise in affected populations, particularly in aging societies. This necessitates a proactive approach to prevention, early detection, and improved treatment. The economic burden of osteoporosis, including healthcare costs and lost productivity, is substantial and will likely increase as the population ages. For instance, in some developed countries, the number of hip fractures related to osteoporosis is rising, impacting healthcare systems and individual lives.
Key Areas of Research and Development in Osteoporosis Treatment
| Area of Research | Description | Potential Impact |
|---|---|---|
| Pharmacological Interventions | Developing novel drugs with enhanced efficacy and reduced side effects, optimizing existing therapies. | Improved bone density, reduced fracture risk, and enhanced quality of life. |
| Non-Pharmacological Interventions | Tailored exercise programs, dietary interventions, and the development of assistive technologies. | Improved muscle strength, enhanced mobility, and reduced risk of falls. |
| Early Detection and Risk Assessment | Development of accurate diagnostic tools and risk assessment models for early identification of individuals at high risk. | Improved preventive strategies, timely intervention, and reduced fracture incidence. |
| Personalized Medicine | Tailoring treatment strategies to individual patient needs and characteristics. | Maximizing treatment efficacy, minimizing adverse effects, and improving patient outcomes. |
Final Review
In conclusion, determining whether osteoporosis constitutes a disability is multifaceted and depends on individual circumstances, medical evaluations, and legal frameworks. While osteoporosis itself is a medical condition, its impact on daily life and access to resources can vary significantly, potentially meeting the criteria for disability in certain contexts. The ongoing research and evolving understanding of the condition will undoubtedly lead to improvements in treatment and support systems for those affected.