Blood smear uses and results are crucial in diagnosing a wide range of health conditions. This detailed exploration delves into the process of preparing and analyzing blood smears, highlighting their importance in identifying various diseases and abnormalities. From the initial sample collection to the final interpretation of results, we’ll cover everything you need to know.
Understanding the steps involved in creating and interpreting blood smears is essential for anyone interested in the medical field. This in-depth guide will explore the techniques, equipment, and considerations needed to ensure accurate and reliable results. From the preparation techniques to the various staining methods, we’ll guide you through the complete process.
Introduction to Blood Smear
A blood smear is a thin, uniform film of blood, spread on a microscope slide, allowing for microscopic examination of blood cells. It’s a fundamental diagnostic tool in hematology, used to identify and quantify different types of blood cells, evaluate their morphology (shape and structure), and detect abnormalities. This process reveals crucial information about the overall health and potential diseases affecting the body.The basic principle behind preparing a blood smear involves carefully spreading a small drop of blood across the surface of a clean glass slide to create a thin, even layer.
This allows for clear visualization of individual blood cells under a microscope. Proper technique is paramount to ensure that the cells are adequately dispersed and not overlapping, maximizing the clarity of the analysis.
Importance of Proper Blood Smear Preparation
Proper preparation is crucial for accurate results. Improper technique can lead to overlapping cells, making identification and counting difficult or impossible. This can result in misdiagnosis or delayed diagnosis of a condition, affecting treatment and patient outcomes. For example, a poorly prepared smear might mask the presence of abnormal cells, leading to an inaccurate assessment of the patient’s blood picture.
Common Types of Blood Smears
Various types of blood smears are used in different diagnostic settings. These differences reflect the specific information sought or the nature of the patient’s condition.
| Smear Type | Sample Source | Preparation Method | Purpose |
|---|---|---|---|
| Peripheral Blood Smear | Venous blood | A drop of blood is spread thinly across a glass slide using a special technique. | Evaluation of red blood cells, white blood cells, and platelets for morphology, number, and abnormalities. |
| Bone Marrow Smear | Bone marrow aspirate | Bone marrow is aspirated, and a drop is spread across a slide. | Assessment of the cellular composition of bone marrow to diagnose various hematological disorders, such as leukemia or aplastic anemia. |
| Spun Blood Smear | Whole blood | Blood is centrifuged to separate its components. The buffy coat (a layer of white blood cells) is then spread on a slide. | Used to examine the white blood cell differential and to assess the level of different white blood cell types in the blood. |
Equipment and Materials
Preparing a blood smear involves meticulous techniques and specialized tools. The accuracy and reliability of the results hinge critically on the quality of the equipment used and the adherence to established protocols. This section will Artikel the essential equipment and materials, along with crucial considerations for their proper use and maintenance.
Essential Equipment and Materials
A comprehensive blood smear preparation necessitates a collection of specific tools and reagents. These items play distinct roles in ensuring the quality of the sample and facilitating accurate microscopic examination.
Blood smears, a simple yet powerful diagnostic tool, reveal crucial information about your blood cells. Knowing the different cell types and their counts helps doctors understand overall health. However, in cases of suspected lung cancer, blood tests can also provide clues about the progression. For instance, certain markers might indicate the presence or absence of the disease, or its stages of lung cancer , aiding in treatment strategies.
Ultimately, blood smear results, alongside other tests, are vital for a comprehensive picture of the patient’s health and treatment plan.
- Microscope: A high-quality light microscope is essential for viewing the blood smear. Different types of microscopes, such as brightfield, phase-contrast, and differential interference contrast (DIC) microscopes, offer varying capabilities in resolving cellular structures. Brightfield microscopes are commonly used for initial observation, while phase-contrast and DIC microscopes enhance the visualization of cellular details, especially in thin blood smears.
The magnification power of the microscope is crucial, typically ranging from 40x to 1000x. Appropriate magnification allows for the detailed observation of blood cells.
- Slides: Clean, properly sized glass slides are vital for preparing and holding the blood smear. Slides must be free of imperfections, scratches, or contaminants to avoid compromising the integrity of the sample. Special care must be taken to ensure slides are clean and dry before use.
- Blood Collection Tubes: Appropriate collection tubes, containing anticoagulants like EDTA or heparin, are necessary to prevent blood clotting and preserve the integrity of the blood cells. Choosing the right anticoagulant is critical for accurate results.
- Blood Smear Spreading Tools: A spreader slide or a slide with a specific angle for smear preparation is essential. These tools are designed for evenly spreading a thin layer of blood on the slide. The quality of the smear significantly impacts the visibility of cells and their morphological characteristics.
- Staining Solutions: Staining solutions like Wright’s stain or Giemsa stain are employed to color the blood cells. This coloring process enhances the contrast between different cell types and facilitates identification and analysis. Proper staining techniques and adherence to recommended staining times are critical for accurate results.
Importance of Equipment Calibration and Maintenance
Accurate measurements and consistent results in blood smear analysis heavily rely on the proper calibration and maintenance of equipment. Regular calibration ensures the precision of the microscope’s magnification and the accuracy of measurements.
- Microscope Calibration: Microscopes need periodic calibration to ensure the accuracy of their magnification. This involves using standardized calibration slides or specialized equipment. Proper calibration is critical for accurate measurement of cell dimensions and identification of anomalies. Calibration procedures should be performed according to the manufacturer’s recommendations.
- Staining Solution Maintenance: The quality of staining solutions can degrade over time. Regular monitoring of staining solution concentrations and appropriate storage conditions are necessary to maintain their effectiveness. Properly stored and maintained staining solutions ensure consistent staining intensity and color differentiation.
- Equipment Maintenance: Regular cleaning and maintenance of the microscope and other equipment is essential to prevent damage and ensure optimal performance. Proper maintenance extends the lifespan of the equipment and helps maintain consistent results. This includes cleaning optical components, checking mechanical parts, and lubricating moving parts as required by the manufacturer.
Equipment Summary Table
The table below provides a concise overview of the equipment required for blood smear preparation.
| Equipment | Description | Purpose | Precautions |
|---|---|---|---|
| Microscope | Optical instrument for viewing specimens | Visual examination of blood cells | Regular calibration and maintenance |
| Glass Slides | Flat, rectangular glass pieces | Holding the blood smear | Ensure cleanliness and absence of imperfections |
| Spreader Slide | Specialized slide for smear preparation | Creating a thin, uniform blood smear | Maintain proper angle for spreading |
| Blood Collection Tubes | Tubes containing anticoagulants | Prevent blood clotting | Use appropriate anticoagulants |
| Staining Solutions (e.g., Wright’s stain) | Solutions to color blood cells | Enhance contrast and identification | Adhere to staining protocols |
Preparation Techniques: Blood Smear Uses And Results
Crafting a high-quality blood smear is crucial for accurate microscopic analysis. A well-prepared smear allows for clear visualization of blood cells, enabling the detection of abnormalities and providing essential diagnostic information. This section delves into the meticulous procedures involved in creating a blood smear, highlighting crucial steps and potential pitfalls to avoid.Proper technique ensures the integrity of the blood sample and maintains the morphology of the cells, crucial for accurate interpretations.
This precision is vital in hematological diagnostics, where even subtle variations in cell shape and size can indicate underlying conditions.
Smear Preparation Procedures
The process of preparing a blood smear involves carefully spreading a thin layer of blood on a microscope slide. This technique is essential for visualizing blood cells under a microscope. This delicate process requires precision to yield optimal results. Suboptimal techniques can lead to overlapping cells, obscuring their morphology and potentially leading to misdiagnosis.
- Sample Collection: Collect a small drop of blood using a lancet or other appropriate method. Ensure the blood sample is fresh and representative of the patient’s condition. The use of a proper anticoagulant is essential if the blood is for further analysis. Incorrect sample collection, such as insufficient blood volume or the use of contaminated equipment, can compromise the quality of the smear.
- Slide Preparation: Clean the microscope slide with a suitable solvent and allow it to air dry. A clean slide ensures a clear background and prevents interfering artifacts. A dirty slide can lead to false positive results.
- Smear Application: Place a small drop of blood near one end of the slide. Using a second, clean slide, gently and firmly drag the second slide across the blood drop, creating a smear. The angle of the second slide and the pressure applied significantly impact the smear’s thickness. A too-thick smear may overlap cells, making analysis difficult. A too-thin smear may not contain enough cells for a meaningful analysis.
The ideal smear should have a consistent thickness, allowing for a clear visualization of individual cells without overlapping.
- Air Drying: Allow the smear to air dry completely at room temperature. Avoid using heat or a hairdryer, as this can distort cell morphology. Rapid drying can lead to shrinkage or other distortions, hindering analysis.
- Fixation: Fix the smear to preserve cell morphology. This is often achieved using a methanol or similar fixative. Improper fixation can lead to cellular damage, obscuring or distorting the features of the cells.
- Staining: Apply a suitable stain (e.g., Wright’s stain) according to the manufacturer’s instructions. This process differentiates the cells, allowing for better visualization of their components and characteristics. Insufficient staining can make cells difficult to distinguish and analyze. Excessive staining can lead to cell distortion and obscuring of important details.
Evaluating Smear Quality
A well-prepared blood smear should exhibit a smooth, even distribution of cells, with no clumps or areas of excessive density. The cells should maintain their characteristic shapes, allowing for clear visualization of their structures. The smear should be thin enough to visualize individual cells without overlapping.
- Appearance: A well-prepared smear will exhibit a smooth, tapered appearance. Areas with excessive clumping or areas of thick or thin concentration should be avoided. This visual inspection is a crucial first step in determining the suitability of the smear for analysis.
- Cell Morphology: The cells on the smear should maintain their characteristic shapes and sizes. Distorted or fragmented cells may indicate issues with preparation techniques. This visual assessment is key in identifying potential problems.
- Consistency: A high-quality smear will have a uniform distribution of cells across the entire length of the smear. This consistency helps to avoid areas with excessive or inadequate cell counts.
Impact of Improper Preparation
Improper preparation techniques can significantly affect the accuracy of the results. For example, if the smear is too thick, cells may overlap, making it difficult to identify individual cells and assess their morphology. This can lead to misdiagnosis or an incomplete assessment of the blood sample.
Staining Procedures
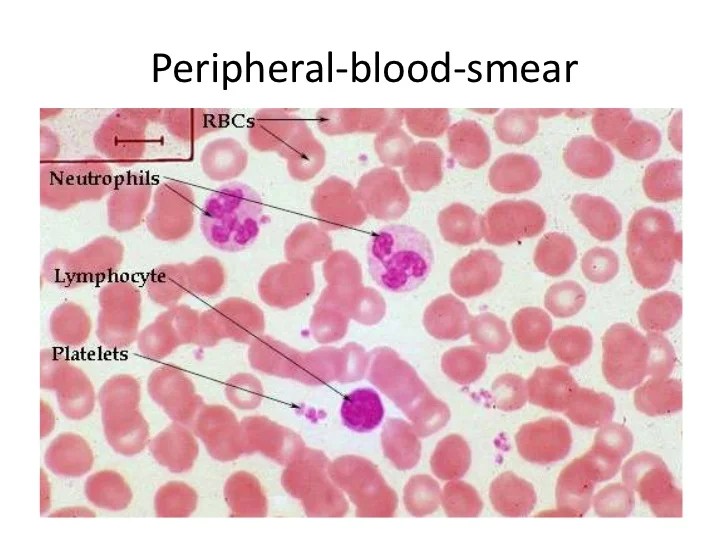
Blood smears, crucial for analyzing blood components, require proper staining to visualize and differentiate various cells. Staining procedures enhance contrast and visibility, enabling accurate identification of red blood cells, white blood cells, and platelets. Different staining techniques target specific cellular components, revealing crucial details for diagnostic purposes.
Different Staining Methods
Various staining methods exist, each with its own advantages and limitations. These methods employ different dyes and procedures to highlight specific cellular structures. Understanding these methods is essential for accurate interpretation of blood smear results.
- Wright-Giemsa Stain: This is a widely used stain for general hematological analysis. It provides a comprehensive view of blood cells, distinguishing different types of leukocytes and evaluating the morphology of red blood cells.
- Romanowsky Stains: This family of stains includes Wright-Giemsa and others, employing a combination of dyes to stain blood components. They are versatile and offer excellent differentiation of blood cell types. The differential staining of components is a crucial advantage of this family.
- May-Grünwald Stain: This stain is a precursor to Wright-Giemsa staining. It is a basic stain that prepares the blood smear for Giemsa staining by staining the cells in a specific manner.
- Giemsa Stain: This stain, often used in combination with a preparatory stain like May-Grünwald, enhances the contrast and visibility of various blood components. Its use is crucial for precise identification of parasites, like malaria parasites, within blood cells.
Comparison and Contrast of Staining Methods
Different staining methods target various components with varying degrees of specificity. Wright-Giemsa staining, for example, is a versatile method that stains a broad spectrum of blood components, while other methods might focus on specific structures or cellular abnormalities. The choice of staining method depends on the specific diagnostic question or the presence of suspected abnormalities.
Step-by-Step Guide to Wright-Giemsa Staining
This method is a cornerstone of hematological analysis, enabling visualization of blood cell morphology and differentiation. The Wright-Giemsa stain procedure is meticulously executed, and understanding each step is vital for accurate results.
Blood smears are a simple but crucial diagnostic tool, revealing a wealth of information about your blood cells. Results can pinpoint issues like anemia, infections, or even certain cancers. Interestingly, the cost of medications significantly impacts access to vital treatments, especially when comparing america versus canada drug prices , highlighting the disparities in healthcare systems.
Ultimately, a thorough blood smear analysis provides essential data for effective patient care.
- Preparation of the Blood Smear: A thin blood smear is prepared on a slide, ensuring a uniform distribution of blood cells for optimal visualization.
- Air Drying: The smear is allowed to air dry, which is crucial for proper staining adhesion and to prevent the distortion of the blood cells during the subsequent steps.
- Fixing: The smear is fixed using a methanol-based fixative, which preserves the cellular structure and morphology for accurate staining and visualization.
- Stain Application: The Wright stain is applied to the smear for a specific time, staining the cells with a differential staining procedure.
- Giemsa Stain Application: After the Wright stain is rinsed, the Giemsa stain is applied for a specific duration, further enhancing the differentiation of blood components.
- Washing and Drying: The slide is thoroughly washed and allowed to air dry, ensuring that the stain is evenly distributed and that excess stain is removed.
- Microscopic Examination: The stained blood smear is examined under a microscope to visualize and identify the different blood cells based on their morphology and staining characteristics.
Role of Each Stain in Highlighting Cellular Components
The dyes in Wright-Giemsa stain have distinct affinities for different cellular components. Methylene blue stains the nucleus and granules of certain cells a bluish-purple color, while eosin stains the cytoplasm of cells, typically appearing in a pinkish-orange shade.
Stain Properties Table
| Stain | Component Targeted | Color Produced | Purpose |
|---|---|---|---|
| Methylene blue | Nucleus, some granules | Blue-purple | Differentiates cell types, identifies nuclear characteristics |
| Eosin | Cytoplasm, granules | Pink-orange | Highlights cytoplasm, distinguishes cell types based on staining |
Analyzing Blood Smear Results
Deciphering the microscopic world of a blood smear reveals crucial insights into a patient’s health. Beyond simply counting blood cells, the analysis delves into the shape, size, and overall appearance of these cells. This detailed examination provides a comprehensive picture of the blood’s composition and function, aiding in the diagnosis of various conditions.Interpreting a blood smear goes beyond basic counting; it involves careful observation of cell morphology and structure.
Recognizing normal and abnormal characteristics allows for a more accurate assessment of the patient’s condition. This meticulous process is vital for medical professionals in making informed decisions and implementing appropriate treatments.
Components Observed in a Blood Smear
The microscopic examination of a blood smear reveals a diverse array of cellular components. Red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes) are the primary elements observed. Variations in their size, shape, and arrangement provide valuable clues about the body’s overall health.
Characteristics of Normal Blood Cells
Normal red blood cells (erythrocytes) typically exhibit a biconcave disc shape, appearing as small, round cells. Their primary function is oxygen transport. Normal white blood cells (leukocytes) display varied appearances, categorized into different types each with specific roles in the immune response. Platelets (thrombocytes) are small, irregular fragments of cells, crucial for blood clotting.
Examples of Abnormal Blood Cells and their Morphologies
Abnormal blood cells exhibit variations in size, shape, and structure, which can be indicative of various underlying conditions. For example, sickle cell anemia is characterized by the presence of sickle-shaped red blood cells. These abnormal shapes can obstruct blood flow and lead to various complications. Megaloblastic anemia presents abnormally large red blood cells, indicative of deficiencies in vitamin B12 or folate.
Similarly, abnormal white blood cell counts or morphologies can signal infections, immune disorders, or other diseases.
Identifying Different Blood Cell Types
Identifying different blood cell types relies on a combination of visual cues and specific characteristics. Red blood cells are readily distinguishable by their biconcave shape and lack of a nucleus. White blood cells are further classified based on their size, cytoplasmic granularity, and nuclear morphology. Platelets are identified as small, irregular fragments. Experience and familiarity with normal cell morphology are crucial for accurate identification.
Interpretation of Cell Counts and Morphology
Cell counts and morphological characteristics provide a wealth of information. Variations in red blood cell count can signal anemia or polycythemia. An elevated white blood cell count might indicate an infection, while a low count can suggest immunodeficiency. Abnormal platelet counts or morphology can suggest clotting disorders or bleeding problems. A comprehensive analysis considers not only cell counts but also the morphology of the cells.
This comprehensive approach helps in accurate interpretation.
Typical Cell Types and Normal Ranges
- Red Blood Cells (Erythrocytes): Normal range typically falls between 4.0 and 5.5 million per microliter (µL) of blood. Lower counts suggest anemia, while higher counts can indicate polycythemia.
- White Blood Cells (Leukocytes): The normal range is approximately 4,500 to 11,000 per µL. Lower counts can suggest immunodeficiency, while higher counts can indicate infections.
- Platelets (Thrombocytes): Normal platelet count ranges from 150,000 to 400,000 per µL. Lower counts can increase the risk of bleeding, while higher counts can suggest clotting disorders.
Clinical Applications
Blood smear analysis is a fundamental tool in hematology, providing crucial insights into the health and function of the blood. It’s a relatively inexpensive and quick procedure, making it an essential part of a comprehensive diagnostic approach. This analysis allows for the detection of a wide array of blood disorders and conditions, ultimately aiding in appropriate patient management and treatment.The clinical significance of blood smear analysis stems from its ability to reveal cellular abnormalities, assess the overall health of the blood, and identify underlying diseases.
Examining a blood smear allows clinicians to visualize red blood cells, white blood cells, and platelets, and observe any deviations from their normal appearance or relative proportions. These visual cues can be incredibly informative, offering a snapshot of the body’s internal processes and helping to pinpoint potential health concerns.
Clinical Significance of Blood Smear Analysis
Blood smears are valuable in diagnosing a range of hematological conditions. They provide vital information about cell morphology, size, shape, and the presence of unusual or abnormal cells. These observations, coupled with other clinical data, can significantly contribute to a precise diagnosis.
Role of Blood Smears in Diagnosing Diseases
Blood smears play a pivotal role in identifying various diseases. By examining the cellular components of the blood, clinicians can detect abnormalities that might indicate underlying conditions. The presence of abnormal cells, altered cell counts, or changes in cell morphology can all be indicative of specific diseases.
Examples of Diseases Detectable Through Blood Smear Analysis
Numerous diseases can be suspected or confirmed through blood smear analysis. Some prominent examples include:
- Anemia: Different types of anemia, such as iron deficiency anemia, megaloblastic anemia, and sickle cell anemia, manifest with characteristic changes in red blood cell morphology. For instance, iron deficiency anemia often shows microcytic, hypochromic red blood cells, while sickle cell anemia exhibits characteristic sickle-shaped cells.
- Leukemias: Various types of leukemia, characterized by abnormal white blood cell counts and morphology, can be identified through blood smear analysis. For example, acute lymphocytic leukemia (ALL) might show an abundance of immature lymphocytes.
- Infections: Certain infections can cause changes in white blood cell counts or the presence of abnormal cells. Bacterial infections, for instance, often lead to an elevated neutrophil count, while parasitic infections may reveal specific parasites within the blood.
- Blood Disorders: Blood smear analysis can identify various blood disorders, including thrombocytopenia (low platelet count), and thrombocytosis (high platelet count), and also reveal abnormal platelet morphology.
Correlation Between Blood Smear Findings and Specific Diagnoses
The correlation between blood smear findings and specific diagnoses is often quite strong. For instance, the presence of numerous nucleated red blood cells suggests a condition like hemolytic anemia. Similarly, the presence of immature white blood cells or specific abnormal cells can indicate specific types of leukemia. The integration of these findings with other diagnostic tests and patient history strengthens the diagnostic accuracy.
Blood Smear Analysis in a Patient’s Overall Diagnostic Workup
Blood smear analysis is an integral part of a patient’s overall diagnostic workup. It serves as a preliminary screening tool, providing crucial initial information about the blood’s cellular components. The results of the blood smear analysis are then used to direct further investigations, such as more specialized blood tests or bone marrow biopsies. The findings from a blood smear are frequently used in conjunction with other clinical data to develop a comprehensive picture of the patient’s condition.
Blood smear tests are pretty common, offering insights into your red and white blood cell counts and overall health. Understanding these results can be crucial, especially when dealing with conditions like fibromyalgia, CFS, and new injuries, which can sometimes manifest in unusual blood markers. For more information on how these conditions might affect your blood work, check out this helpful resource on fibromyalgia cfs and new injuries.
Ultimately, a blood smear can help your doctor pinpoint potential issues and guide treatment plans.
Table: Diseases, Expected Findings, and Diagnostic Relevance, Blood smear uses and results
| Disease | Expected Findings | Diagnostic Relevance |
|---|---|---|
| Iron Deficiency Anemia | Microcytic, hypochromic red blood cells; reduced red blood cell count | Suggests iron deficiency as a cause of anemia |
| Sickle Cell Anemia | Sickle-shaped red blood cells | Confirms the diagnosis of sickle cell disease |
| Acute Myeloid Leukemia (AML) | Increased immature myeloid cells, blasts, and abnormal white blood cells | Indicates the presence of AML, prompting further investigations |
| Bacterial Infection | Elevated neutrophil count | Suggests a bacterial infection and guides treatment decisions |
| Thrombocytopenia | Low platelet count, potentially abnormal platelet morphology | Indicates a potential platelet disorder, prompting further investigations |
Safety Precautions
Blood smear preparation, though seemingly straightforward, involves handling potentially hazardous biological samples. Adherence to strict safety protocols is crucial to prevent exposure to infectious agents and maintain a safe working environment. Understanding the risks and implementing appropriate safety measures safeguards both the laboratory personnel and the patients.Proper handling of blood samples and meticulous disposal of used materials are paramount.
Personal protective equipment (PPE) plays a critical role in minimizing exposure risks. The following sections detail essential safety precautions and procedures to be followed during blood smear preparation.
Handling Potentially Infectious Samples
Safe handling of blood samples is critical to prevent the transmission of infectious diseases. Blood, and other body fluids, should be treated as potentially infectious. All procedures involving blood smears must adhere to universal precautions. This includes the immediate and thorough disinfection of all surfaces and equipment that come into contact with the sample.
Proper Disposal of Used Materials
Proper disposal of used materials is essential to prevent contamination and ensure a clean working environment. Used slides, gloves, and other contaminated materials should be placed in appropriate biohazard containers. These containers should be labeled clearly and stored securely to prevent leakage and accidental exposure. Examples of appropriate containers include sharps containers for lancets and broken glass, and leak-proof bags for contaminated materials.
Proper disposal protocols vary depending on local regulations and guidelines.
Importance of Personal Protective Equipment (PPE)
Personal protective equipment (PPE) acts as a barrier against exposure to potentially infectious materials. A consistent and comprehensive PPE strategy is vital for minimizing the risk of exposure. PPE should include, but is not limited to, disposable gloves, laboratory coats, eye protection (safety glasses or face shields), and masks, depending on the specific procedure.
Safety Procedures and PPE Guidelines
- Always wear appropriate PPE, including gloves, lab coat, and eye protection, when handling blood samples. This protects against splashes and contact with potentially infectious materials.
- Use disposable gloves during all procedures involving blood samples. Change gloves between handling different samples or if they become contaminated.
- Handle all sharps with extreme care. Use appropriate sharps containers for disposal.
- Avoid direct contact with blood and other body fluids. Use appropriate tools and techniques to minimize contact.
- Immediately disinfect all surfaces and equipment that come into contact with blood samples. Follow the laboratory’s standard disinfection procedures.
- Wash hands thoroughly with antimicrobial soap and water after handling blood samples and before leaving the laboratory. This includes removing all visible contamination from the hands before washing.
- Report any suspected exposure to infectious materials immediately to the supervisor. This is essential for proper follow-up and to prevent the spread of potential infections.
- Adhere to local and national guidelines for handling and disposing of biological waste.
- Know the location and proper use of emergency eyewash stations and safety showers. These are critical in case of accidental exposure.
Illustrative Examples
Blood smears provide invaluable insights into the health of a patient’s blood. By examining the morphology and relative abundance of different blood cells, clinicians can identify various conditions, from simple anemia to life-threatening infections. These examples illustrate the types of observations one might make during a blood smear analysis.
Healthy Blood Smear
A healthy blood smear exhibits a balanced distribution of various cell types. Erythrocytes (red blood cells) are typically biconcave discs, exhibiting a smooth, uniform appearance. Their relative abundance is high, occupying the majority of the field of view. Leukocytes (white blood cells), including neutrophils, lymphocytes, monocytes, eosinophils, and basophils, are present in smaller numbers and are characterized by diverse shapes and sizes.
Platelets (thrombocytes), appearing as small, irregular fragments, are also visible, although their quantity is less than that of red blood cells. The overall appearance is one of homogeneity, with cells maintaining their typical shapes and sizes. No significant abnormalities are evident.
Anemia
Anemia is characterized by a decrease in the number or function of red blood cells. A blood smear showing anemia would display a reduced number of erythrocytes. The erythrocytes themselves might exhibit a pale or hypochromic appearance, indicating reduced hemoglobin content. Some erythrocytes might show signs of microcytosis (smaller size) or macrocytosis (larger size), depending on the type of anemia.
The red blood cell distribution may be less uniform than in a healthy sample. There might be evidence of poikilocytosis, meaning red blood cells with abnormal shapes, such as teardrops, spherocytes, or sickle cells, depending on the underlying cause. The overall density of red blood cells is noticeably reduced compared to a healthy smear.
Leukemia
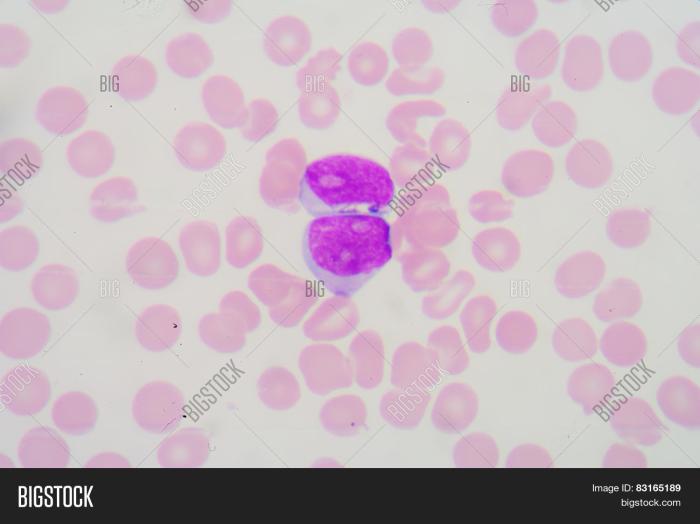
Leukemia involves an uncontrolled proliferation of white blood cells. In a blood smear exhibiting leukemia, the number of leukocytes is significantly elevated. Some white blood cells may display abnormal morphology, exhibiting atypical sizes, shapes, and nuclear structures. The nucleus of the white blood cells might be enlarged or have an unusual shape. There might be an increase in immature white blood cell forms, known as blasts, which are not normally present in significant numbers.
The balance between different types of white blood cells might be disrupted, with some types being abnormally high or low. The presence of these abnormal cells significantly alters the normal cellular composition of the blood.
Parasitic Infection
A parasitic infection, such as malaria, might manifest in a blood smear with the presence of parasites within red blood cells. Malarial parasites, for example, typically appear as distinct forms within erythrocytes. These parasites might be present in various stages of development, and their morphology could vary depending on the specific parasite species and the stage of infection.
Parasites might be present in a cluster within red blood cells or distributed throughout the smear. Besides the parasites, other blood cells might also show signs of damage or infection. For example, red blood cells might exhibit varying degrees of damage and distortion, and the number of platelets might be decreased.
Final Conclusion
In conclusion, blood smear analysis provides a powerful tool for diagnosing a multitude of diseases, from anemia to leukemia and parasitic infections. By understanding the preparation techniques, staining procedures, and interpretation of results, healthcare professionals can gain invaluable insights into a patient’s health. This comprehensive guide offers a clear understanding of the significance and applications of blood smears in modern medicine.