Diabetes and liver disease are intertwined conditions impacting global health. This exploration delves into the complex relationship between these two diseases, examining their commonalities, mechanisms of interaction, diagnosis, management, complications, and preventative strategies. We’ll uncover the stages of progression, the role of insulin resistance, and the importance of early intervention.
From understanding the fundamental definitions of both diabetes and liver disease to exploring the latest research on diagnosis and treatment, this comprehensive overview aims to provide a thorough understanding of the interconnected nature of these conditions. We will analyze the physiological mechanisms, potential complications, and discuss crucial strategies for prevention and management.
Introduction to Diabetes and Liver Disease
Diabetes and liver disease are two significant health concerns globally, often intertwined and impacting millions. Both conditions are characterized by complex biological mechanisms and can lead to severe complications if not managed effectively. Understanding their commonalities, prevalence, and potential overlaps is crucial for effective prevention and treatment strategies.
Definitions of Diabetes and Liver Disease
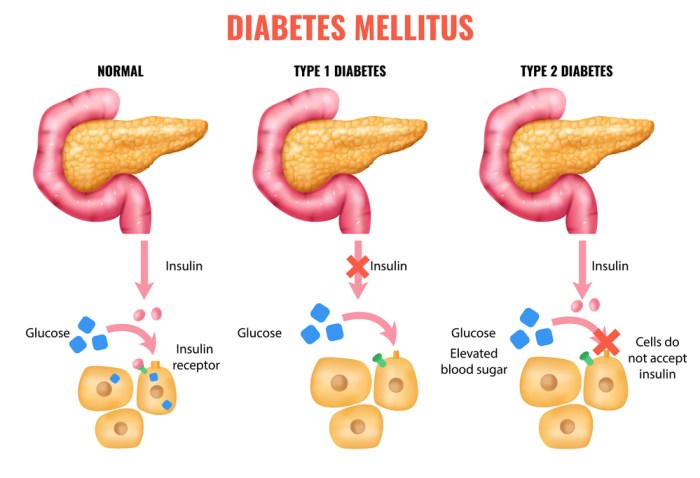
Diabetes is a chronic metabolic disorder characterized by elevated blood glucose levels. This elevation results from either insufficient insulin production by the pancreas or impaired insulin action in the body’s cells. There are various types of diabetes, including type 1, type 2, and gestational diabetes, each with its unique causes and characteristics. Liver disease encompasses a wide range of conditions affecting the liver’s structure and function.
These conditions can be caused by various factors, including viral infections, alcohol abuse, non-alcoholic fatty liver disease (NAFLD), and autoimmune disorders. The liver’s role in metabolism, detoxification, and blood filtration makes its dysfunction a significant health concern.
Commonalities and Overlap
A key commonality between diabetes and liver disease is their significant impact on metabolic processes. Both conditions often share risk factors, such as obesity, a sedentary lifestyle, and poor dietary habits. Insulin resistance, a hallmark of type 2 diabetes, is frequently associated with non-alcoholic fatty liver disease (NAFLD), a leading cause of chronic liver disease. The liver plays a critical role in regulating blood glucose levels, and its dysfunction can exacerbate diabetes complications.
Conversely, uncontrolled diabetes can also contribute to liver damage, further complicating the conditions.
Prevalence and Global Impact
Diabetes and liver disease are prevalent globally, impacting millions of lives. The World Health Organization (WHO) reports a significant increase in the prevalence of diabetes, largely due to lifestyle factors and population aging. Similarly, liver disease, encompassing various forms, also represents a substantial global health burden. The prevalence and impact of these conditions are particularly high in regions with high rates of obesity and poor nutrition.
For example, studies have shown a correlation between high fructose corn syrup consumption and increased risk of both conditions in specific populations.
Stages of Progression and Complications
Both diabetes and liver disease progress through stages, with early detection and management crucial for preventing complications. Diabetes, if left uncontrolled, can lead to severe complications such as cardiovascular disease, kidney damage, nerve damage, and blindness. Similarly, liver disease, if untreated, can progress to cirrhosis, liver failure, and hepatocellular carcinoma (liver cancer). The stages of progression often vary depending on the specific type of liver disease and the individual’s overall health.
Table: Diabetes and Liver Disease
| Disease | Symptoms | Risk Factors | Treatments |
|---|---|---|---|
| Diabetes | Frequent urination, excessive thirst, unexplained weight loss, blurred vision, slow-healing sores | Family history, obesity, lack of physical activity, unhealthy diet, certain medications | Dietary changes, exercise, medication (insulin or oral hypoglycemics), blood glucose monitoring |
| Liver Disease | Fatigue, abdominal pain, jaundice (yellowing of the skin and eyes), swelling in the legs and abdomen, loss of appetite | Alcohol abuse, viral infections (hepatitis), obesity, certain medications, genetics | Lifestyle changes (diet and exercise), medications, liver transplant (in severe cases) |
Mechanisms of Disease Interaction
The intricate dance between diabetes and liver disease involves a complex interplay of physiological mechanisms. Both conditions share overlapping risk factors and detrimental consequences, highlighting the importance of understanding their interconnectedness. Understanding these mechanisms is crucial for developing targeted interventions and improving patient outcomes.
Insulin Resistance and Liver Function
Insulin resistance, a hallmark of type 2 diabetes, directly impacts liver function. In this state, cells fail to respond adequately to insulin, leading to elevated blood glucose levels. The liver, normally a key player in glucose homeostasis, becomes overwhelmed. It compensates by producing more glucose, exacerbating hyperglycemia and further contributing to insulin resistance. This vicious cycle perpetuates the progression of both diabetes and liver disease.
Impact of Hyperglycemia on Liver Metabolism and Structure
Chronic hyperglycemia damages the liver at multiple levels. Sustained high blood glucose levels promote the formation of advanced glycation end products (AGEs). These molecules accumulate in liver tissue, causing structural damage and impairing normal liver function. Further, hyperglycemia can lead to oxidative stress, a process that triggers cellular damage and inflammation, contributing to the development of non-alcoholic fatty liver disease (NAFLD) and cirrhosis.
Diabetes and liver disease can be a tough combo, impacting each other in complex ways. Managing blood sugar levels is crucial, but sometimes medications like benzodiazepines are used to help. Understanding the uses types and risks of benzodiazepines is important for anyone navigating these conditions. Ultimately, a holistic approach to care, considering the potential interactions of various treatments, is key to effectively managing both diabetes and liver health.
Inflammatory Processes in Liver Disease and Diabetes
Inflammation plays a crucial role in the development and progression of both diabetes and liver disease. Chronic inflammation, triggered by various factors including insulin resistance and hyperglycemia, contributes to liver damage and dysfunction. This inflammatory response creates a pro-inflammatory environment, further exacerbating the cycle of damage. The inflammatory mediators released during this process also contribute to systemic inflammation, potentially affecting other organs.
Role of Oxidative Stress
Oxidative stress, characterized by an imbalance between reactive oxygen species (ROS) and antioxidant defenses, is a common thread linking diabetes and liver disease. ROS damage cellular components, including DNA, proteins, and lipids, leading to liver cell damage and dysfunction. In the context of diabetes, oxidative stress contributes to insulin resistance and β-cell dysfunction. This heightened oxidative stress is also implicated in the progression of liver damage, contributing to the development of NAFLD and its progression to cirrhosis.
Mechanism Table
| Mechanism | Impact on Diabetes | Impact on Liver | Potential Interventions |
|---|---|---|---|
| Insulin Resistance | Elevated blood glucose levels, impaired insulin signaling | Increased glucose production, fatty infiltration | Lifestyle modifications (diet, exercise), medications to improve insulin sensitivity |
| Hyperglycemia | Damage to blood vessels, nerve cells, and other tissues | Formation of AGEs, oxidative stress, inflammation, liver fibrosis | Tight glycemic control, medications to lower blood glucose levels |
| Inflammation | Systemic inflammation, potential for other complications | Liver damage, fibrosis, cirrhosis | Anti-inflammatory medications, lifestyle modifications to reduce inflammation |
| Oxidative Stress | Insulin resistance, β-cell dysfunction | Cellular damage, liver injury, fibrosis | Antioxidant therapies, lifestyle modifications to reduce oxidative stress |
Diagnosis and Assessment
Pinpointing the presence and severity of both diabetes and liver disease requires a meticulous approach. Accurate diagnosis enables timely interventions and personalized treatment plans, maximizing positive outcomes. This crucial step involves a combination of diagnostic criteria, specialized tests, and ongoing monitoring.The interplay between these two conditions often necessitates a multifaceted evaluation. A thorough understanding of diagnostic tools and assessment procedures is essential for healthcare professionals to effectively manage patients with both diabetes and liver disease.
Diabetes and liver disease can be a tough combo, impacting everything from energy levels to overall well-being. One often overlooked aspect is the connection to mental health, specifically anxiety. Understanding the different types of anxiety disorders can help in navigating these challenges. Managing these anxieties, along with the physical aspects of diabetes and liver disease, is crucial for a healthier lifestyle.
This involves recognizing specific symptoms, conducting appropriate tests, and interpreting results within the context of the patient’s overall health.
Diagnostic Criteria for Diabetes
Diabetes is diagnosed based on criteria established by organizations like the American Diabetes Association (ADA). These criteria typically include fasting plasma glucose levels, oral glucose tolerance tests, and HbA1c levels. A diagnosis is often made when a patient demonstrates persistently elevated blood sugar levels, exceeding established thresholds.
Diagnostic Criteria for Liver Disease
Liver disease diagnosis relies on various factors. These include physical examination findings, blood tests to assess liver function, and potentially imaging studies like ultrasound or MRI. Specific liver enzymes, bilirubin levels, and other markers provide crucial insights into the health of the liver.
Liver Function Tests in Diabetic Patients
Assessment of liver function in diabetic patients necessitates specific attention due to the potential for complications. Liver function tests are critical, providing insights into liver health. These tests typically include alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), and bilirubin levels. Elevations in these enzymes may signal liver damage.
Evaluating Liver Damage in Patients with Diabetes
Liver damage in diabetic patients can manifest in various ways. Regular monitoring of liver function tests is essential. Healthcare professionals must consider factors such as duration and severity of diabetes, medication usage, and other underlying health conditions. Additional tests might include Fibroscan or liver biopsies to assess the extent of fibrosis or inflammation.
Common Markers and Indicators
Several markers and indicators aid in diagnosing and monitoring both conditions. Blood glucose levels, HbA1c, liver enzymes (ALT, AST, ALP), bilirubin, and imaging studies are common examples. The interpretation of these results is crucial, often requiring a comprehensive evaluation of the patient’s medical history.
Importance of Regular Monitoring and Follow-up
Ongoing monitoring and follow-up are vital for both diabetes and liver disease. Regular blood tests and check-ups allow for early detection of complications and adjustments to treatment plans. This proactive approach is crucial for managing these conditions effectively and improving patient outcomes.
Comparison of Diagnostic Tests
| Test Type | Purpose | Procedure | Results |
|---|---|---|---|
| Fasting Plasma Glucose | Assess blood glucose levels after an overnight fast. | Blood sample collected after an overnight fast. | Elevated levels may indicate diabetes. |
| Oral Glucose Tolerance Test | Assess blood glucose response to a glucose load. | Patient ingests a specific amount of glucose, and blood samples are taken at intervals. | Elevated glucose levels at specific time points suggest impaired glucose tolerance. |
| HbA1c | Reflect average blood glucose levels over the past 2-3 months. | Blood sample analysis. | High HbA1c levels indicate poor glucose control. |
| ALT/AST | Assess liver cell damage. | Blood sample analysis. | Elevated levels may suggest liver inflammation or damage. |
| Bilirubin | Evaluate liver function and potential obstruction. | Blood sample analysis. | Elevated levels may indicate liver dysfunction or blockage. |
| Fibroscan | Assess liver fibrosis. | Non-invasive ultrasound-based test. | Provides a measure of liver stiffness. |
Management Strategies
Managing both diabetes and liver disease requires a multifaceted approach that prioritizes lifestyle modifications, appropriate medications, and consistent monitoring. Successful management hinges on a strong patient-physician partnership, enabling proactive adjustments to treatment plans as needed. Understanding the interplay between these conditions is crucial for developing effective strategies that address the unique challenges faced by those affected.
Lifestyle Modifications
Adopting healthy lifestyle choices forms the cornerstone of management for both diabetes and liver disease. These modifications significantly impact disease progression and overall well-being. A balanced diet low in processed foods, sugar, and saturated fats is essential. Regular physical activity, such as brisk walking, swimming, or cycling, helps regulate blood glucose levels and improve liver function. Maintaining a healthy weight through diet and exercise is also critical.
Smoking cessation and limiting alcohol consumption are equally important for improving liver health and reducing the risk of complications in diabetes.
Treatment Options
Various treatment options are available for both diabetes and liver disease, each with its own mechanism of action, potential side effects, and patient considerations. The selection of appropriate therapies depends on the specific type and severity of each condition. Insulin therapy is often a key component in managing diabetes, especially in type 1 diabetes or uncontrolled type 2 diabetes.
Oral medications, such as metformin, sulfonylureas, and DPP-4 inhibitors, are also used to regulate blood sugar levels. For liver disease, treatments may include medications to reduce inflammation, protect liver cells, and manage complications. Dietary changes, along with medications, are often prescribed for managing non-alcoholic fatty liver disease (NAFLD).
Diabetes and liver disease often go hand-in-hand, impacting each other negatively. Understanding how diseases like these interact is crucial. It’s also important to consider how other illnesses can affect these conditions. For instance, how does bird flu spread to humans? how does bird flu spread to humans This can have implications for overall health, particularly when it comes to managing diabetes and liver issues, highlighting the interconnectedness of various health concerns.
Learning more about the different ways these conditions affect the body can help us develop better strategies for prevention and treatment.
Medication and Therapies
Medications play a vital role in managing both diabetes and liver disease. For diabetes, medications like metformin, insulin, and various oral agents help control blood sugar levels, reducing the risk of long-term complications. For liver disease, medications may target inflammation, fibrosis, or viral infections, depending on the underlying cause. In some cases, therapies like liver transplantation may be necessary to address severe liver damage.
The choice of medication and therapy is tailored to individual needs and disease severity.
Long-Term Management and Prevention
Long-term management of diabetes and liver disease requires ongoing monitoring, consistent adherence to treatment plans, and proactive identification and management of potential complications. Regular check-ups, blood tests, and lifestyle adjustments are vital. Early detection and treatment of complications such as kidney disease, cardiovascular disease, and nerve damage are essential for preventing further deterioration. Proactive lifestyle choices, such as healthy eating, regular exercise, and avoidance of harmful substances, are critical preventive measures for both conditions.
Table of Treatment Options
| Treatment Type | Mechanism of Action | Potential Side Effects | Patient Considerations |
|---|---|---|---|
| Metformin (Diabetes) | Reduces glucose production in the liver, improves insulin sensitivity | Gastrointestinal upset (nausea, diarrhea), vitamin B12 deficiency | May not be suitable for patients with kidney disease or liver impairment. |
| Insulin (Diabetes) | Replaces or supplements the body’s insulin production | Hypoglycemia (low blood sugar), weight gain | Requires careful monitoring of blood sugar levels and potential adjustments to dosage. |
| Antivirals (Hepatitis C) | Target and eliminate the hepatitis C virus | Possible flu-like symptoms, skin rash, fatigue | Requires close monitoring for side effects and adherence to the prescribed regimen. |
| Lifestyle Modifications (Both) | Improve overall health, regulate blood sugar and liver function | Requires consistent effort and lifestyle adjustments | Long-term commitment is crucial for sustained improvements. |
Complications and Prognosis: Diabetes And Liver Disease
The combination of diabetes and liver disease creates a complex interplay of risks, significantly impacting a patient’s overall health and well-being. Understanding the potential complications, their severity, and the impact on prognosis is crucial for effective management and preventative strategies. This knowledge empowers both patients and healthcare providers to make informed decisions and strive for improved outcomes.
Potential Complications
The simultaneous presence of diabetes and liver disease creates a synergistic effect, increasing the likelihood and severity of various complications. These conditions can exacerbate existing vulnerabilities and introduce new challenges to health management. A critical aspect of managing these conditions is proactive identification and management of potential complications.
- Cardiovascular Disease: Both diabetes and liver disease are independent risk factors for cardiovascular complications. The combination significantly elevates the risk of heart attack, stroke, and peripheral artery disease. For example, a patient with both conditions might experience a heart attack at a younger age compared to someone with only diabetes or only liver disease.
- Kidney Disease (Nephropathy): Diabetic nephropathy is a serious complication of diabetes, and liver disease can accelerate its progression. The kidneys work harder to filter toxins when the liver isn’t functioning optimally, increasing the risk of kidney failure. This is particularly important in long-term management.
- Peripheral Neuropathy: Damage to the nerves, a common complication of diabetes, can be further aggravated by liver disease. This can lead to numbness, tingling, and pain in the extremities, impacting mobility and daily activities.
- Hepatic Encephalopathy: This complication, characterized by impaired brain function, can occur in individuals with advanced liver disease. Diabetes can exacerbate this condition, potentially leading to confusion, lethargy, and even coma. The interaction between the two conditions requires careful monitoring and management.
- Increased Risk of Infections: Both diabetes and liver disease compromise the immune system, increasing susceptibility to infections. This can range from simple colds to more serious complications.
Impact on Overall Health and Quality of Life
The combined effect of diabetes and liver disease profoundly impacts a patient’s quality of life. Chronic pain, fatigue, limited mobility, and cognitive impairment can significantly reduce their ability to participate in daily activities and maintain a sense of well-being.
Organ Damage Potential
The interaction of diabetes and liver disease can lead to progressive organ damage. The liver, kidneys, and heart are particularly vulnerable. The severity of organ damage varies significantly based on the individual’s condition, treatment adherence, and lifestyle choices.
Prognosis Comparison
The prognosis for patients with both diabetes and liver disease is often more guarded than for those with either condition alone. Factors such as the severity of each condition, the presence of other comorbidities, and the patient’s adherence to treatment plans influence the outcome. Early intervention and lifestyle modifications can significantly improve the prognosis. For instance, a patient diagnosed early and committed to a strict treatment plan may experience a more favorable prognosis than one with advanced disease and poor adherence.
Importance of Early Intervention and Prevention, Diabetes and liver disease
Early diagnosis and prompt intervention are critical in managing the combined effects of diabetes and liver disease. Preventive measures, such as maintaining a healthy weight, following a balanced diet, exercising regularly, and managing stress, can reduce the risk of complications and improve the overall prognosis.
Potential Complications, Severity, and Treatment Approaches
| Potential Complications | Severity (Mild, Moderate, Severe) | Treatment Approaches |
|---|---|---|
| Cardiovascular Disease | Moderate to Severe | Aggressive management of blood sugar, blood pressure, and cholesterol levels; lifestyle modifications, medications |
| Kidney Disease | Moderate to Severe | Management of blood sugar and blood pressure; medications to protect kidney function; dialysis |
| Peripheral Neuropathy | Mild to Moderate | Pain management; nerve-protective medications; lifestyle modifications to improve blood sugar control |
| Hepatic Encephalopathy | Moderate to Severe | Management of liver function; medications; dietary restrictions; liver transplant in advanced cases |
| Increased Risk of Infections | Mild to Severe | Vaccination; prophylactic antibiotics; meticulous hygiene; close monitoring |
Prevention and Risk Reduction
Preventing both diabetes and liver disease requires a proactive approach focusing on lifestyle modifications and early detection. A combination of healthy eating, regular physical activity, and maintaining a healthy weight can significantly reduce the risk of developing these conditions. Early intervention is crucial to mitigate the progression of these diseases and prevent severe complications.
Risk Factors for Diabetes and Liver Disease
Understanding the risk factors for both diabetes and liver disease is paramount for developing effective preventive strategies. Multiple factors contribute to the development of these conditions, and a holistic approach is necessary for comprehensive risk reduction. Identifying and addressing these factors empowers individuals to make informed choices about their health.
| Risk Factor | Description | Prevention Strategies | Impact |
|---|---|---|---|
| Family History | A strong family history of diabetes or liver disease increases an individual’s susceptibility to these conditions. Genetic predisposition plays a role in the development of these diseases. | Regular check-ups with a healthcare professional to monitor for early signs and symptoms. Genetic counseling may be beneficial to understand potential risks. | Increased likelihood of developing diabetes or liver disease. Early monitoring and proactive management can significantly mitigate risks. |
| Unhealthy Diet | A diet high in processed foods, saturated fats, and sugary drinks contributes to weight gain and insulin resistance, increasing the risk of diabetes. A poor diet can also damage the liver over time. | Prioritize whole, unprocessed foods, lean proteins, fruits, and vegetables. Limit consumption of sugary drinks and processed foods. Consult a registered dietitian for personalized dietary guidance. | Elevated risk of insulin resistance, weight gain, and liver damage. A balanced diet can significantly reduce these risks. |
| Sedentary Lifestyle | Lack of physical activity contributes to weight gain and insulin resistance, increasing the risk of developing both conditions. | Incorporate regular physical activity into daily routines, such as brisk walking, cycling, or swimming. Aim for at least 150 minutes of moderate-intensity aerobic activity per week. | Increased risk of weight gain, insulin resistance, and potential complications associated with these conditions. Regular exercise can substantially reduce these risks. |
| Obesity | Excess body weight is a major risk factor for both diabetes and liver disease. Adipose tissue can contribute to insulin resistance and liver damage. | Maintain a healthy weight through a combination of balanced diet and regular exercise. Consult a healthcare professional for personalized weight management plans. | Increased risk of insulin resistance, type 2 diabetes, non-alcoholic fatty liver disease, and associated complications. Weight management is crucial in mitigating these risks. |
| High Blood Pressure | High blood pressure can damage blood vessels throughout the body, including those in the liver and pancreas. | Maintain a healthy lifestyle, including a balanced diet and regular exercise. Manage blood pressure through medication if necessary, following a doctor’s advice. | Increased risk of damage to blood vessels in the liver and pancreas, potentially exacerbating conditions like diabetes and liver disease. Controlling blood pressure reduces the risks of complications. |
| High Cholesterol | High cholesterol levels can contribute to the development of fatty deposits in the liver, leading to non-alcoholic fatty liver disease. | Adopt a heart-healthy diet low in saturated and trans fats. Engage in regular physical activity. Consider medication if cholesterol levels remain high, following a doctor’s guidance. | Increased risk of non-alcoholic fatty liver disease (NAFLD) and potential progression to more severe liver conditions. Managing cholesterol levels reduces the risks. |
| Excessive Alcohol Consumption | Chronic alcohol abuse is a significant risk factor for liver disease, including alcoholic hepatitis and cirrhosis. | Limit alcohol consumption to recommended guidelines or abstain completely. Seek support from healthcare professionals or support groups if struggling with alcohol dependence. | Direct damage to the liver, increased risk of liver inflammation and scarring (cirrhosis). Abstaining or limiting alcohol consumption is crucial in preventing liver damage. |
Lifestyle Modifications for Prevention
Implementing lifestyle modifications is a cornerstone of prevention for both diabetes and liver disease. These changes not only reduce the risk of developing these conditions but also improve overall health and well-being. Making sustainable lifestyle changes can significantly impact long-term health outcomes.
- Healthy Diet: Prioritizing a balanced diet rich in fruits, vegetables, whole grains, and lean proteins is crucial. Reducing processed foods, sugary drinks, and excessive saturated fats is equally important. This dietary approach supports overall health and reduces the risk of developing both conditions.
- Regular Exercise: Regular physical activity helps regulate blood sugar levels, maintain a healthy weight, and reduce the risk of insulin resistance. Aim for at least 150 minutes of moderate-intensity aerobic activity per week.
- Weight Management: Maintaining a healthy weight through a balanced diet and regular exercise is essential. Excess weight contributes to insulin resistance and liver damage. Professional guidance from healthcare providers is often beneficial.
Importance of Early Detection and Intervention
Early detection and prompt intervention are critical for managing both diabetes and liver disease effectively. Early diagnosis allows for timely intervention, potentially slowing the progression of the disease and reducing the risk of complications. Prompt medical attention can lead to better management and outcomes.
Strategies for Reducing Complications
Implementing strategies to reduce complications is an integral part of preventative care. Managing blood sugar levels, blood pressure, and cholesterol levels, along with regular monitoring and follow-up care, can help prevent complications associated with these diseases. A proactive approach to managing risk factors and early intervention are essential.
Illustrative Case Studies
Understanding the complex interplay between diabetes and liver disease requires careful examination of real-world cases. These case studies illuminate the diverse presentation of these conditions, the challenges in diagnosis, and the effectiveness of various treatment strategies. They provide invaluable insights into the long-term management and potential outcomes for individuals facing these intertwined health concerns.
A Case Study of Diabetic Hepatic Steatosis
This case study details a patient with a long history of type 2 diabetes who developed non-alcoholic fatty liver disease (NAFLD). The interplay of these conditions underscores the importance of proactive screening and comprehensive management.
A 55-year-old female presented with increasing fatigue, abdominal discomfort, and elevated liver enzymes. She had a 10-year history of type 2 diabetes, well-controlled with metformin and lifestyle modifications. Her family history included a strong predisposition to both diabetes and liver disease. Initial blood work revealed elevated alanine aminotransferase (ALT) and aspartate aminotransferase (AST) levels, indicative of liver dysfunction.
Further testing confirmed the presence of hepatic steatosis, a key feature of NAFLD.
The patient’s diagnosis included type 2 diabetes, NAFLD, and metabolic syndrome. The treatment plan emphasized lifestyle modifications, including a balanced diet, regular exercise, and weight management. Medical nutrition therapy (MNT) was crucial in helping the patient understand the importance of carbohydrate counting and portion control. Metformin, already part of her diabetes management regimen, was continued. In addition, the patient was prescribed a statin to manage lipid levels and a vitamin E supplement to support liver health.
Regular follow-up appointments were scheduled to monitor liver function and glycemic control.
Patient Response to Treatment
The patient showed a remarkable response to the comprehensive treatment plan. Within three months, her liver enzyme levels normalized, and her fatigue subsided. Regular monitoring of blood glucose levels ensured that the diabetes remained well-controlled. The patient’s weight gradually decreased as she adhered to the dietary and exercise recommendations.
Long-Term Outcomes and Management Strategies
Long-term management focused on sustained lifestyle changes and regular monitoring. The patient continued to receive MNT, and her diabetes was maintained with metformin. Regular blood tests monitored liver function and glycemic control. Annual screenings for complications, such as cirrhosis and cardiovascular disease, were incorporated into her healthcare routine.
Comprehensive Analysis of the Case Study
This case study illustrates the insidious nature of NAFLD in individuals with diabetes. The prompt diagnosis and a multi-pronged treatment approach were crucial in achieving positive outcomes. The successful management highlighted the significance of early detection, lifestyle interventions, and close medical supervision in improving patient well-being and reducing the risk of long-term complications.
Summary Table
| Patient Information | Diagnosis | Treatment | Outcome |
|---|---|---|---|
| 55-year-old female, type 2 diabetes (10 years), family history of diabetes and liver disease | Type 2 diabetes, NAFLD, Metabolic Syndrome | Lifestyle modifications (diet, exercise, weight management), MNT, Metformin, Statin, Vitamin E | Normalized liver enzymes, reduced fatigue, sustained glycemic control, gradual weight loss, successful long-term management |
Ending Remarks
In conclusion, diabetes and liver disease present a significant health challenge requiring comprehensive understanding and proactive management. By grasping the intricate relationship between these conditions, individuals and healthcare providers can develop personalized strategies to mitigate risks and improve outcomes. Early detection, lifestyle modifications, and appropriate medical interventions are crucial for effective management and preventing serious complications. Ultimately, a holistic approach encompassing both medical care and lifestyle changes is essential for optimal health and well-being.










