Surgery for peptic ulcers is a crucial treatment option for those experiencing persistent pain and discomfort. This comprehensive guide explores the various aspects of this procedure, from understanding the condition itself to the recovery process and potential alternatives. We’ll delve into the causes, diagnostics, surgical techniques, and even the pre- and post-operative care to provide a thorough understanding of this medical journey.
This in-depth look at surgery for peptic ulcers will equip you with the knowledge to make informed decisions about your health. We’ll cover the different types of ulcers, the diagnostic methods used, and the various surgical procedures available, helping you understand the pros and cons of each approach. We’ll also address alternative treatments, potential complications, and the importance of post-operative care.
Introduction to Peptic Ulcers
Peptic ulcers are sores that develop on the lining of the stomach or the duodenum, the first part of the small intestine. These sores can cause significant discomfort and, if left untreated, can lead to complications. Understanding the causes, symptoms, and types of peptic ulcers is crucial for early detection and effective management.A peptic ulcer forms when the digestive acids in the stomach erode the protective lining of the stomach or duodenum.
This erosion can occur due to various factors, including bacterial infections, certain medications, and underlying medical conditions. Common symptoms include abdominal pain, heartburn, nausea, and vomiting.
Causes of Peptic Ulcers
Several factors contribute to the development of peptic ulcers. Bacterial infections, primarily by Helicobacter pylori, are a significant cause. This bacteria produces substances that damage the protective lining of the stomach and duodenum. Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can also irritate the lining, increasing the risk of ulcer development. Other factors include stress, smoking, and alcohol consumption, which can weaken the protective mechanisms in the digestive tract.
Types of Peptic Ulcers
Peptic ulcers are broadly categorized into gastric ulcers and duodenal ulcers. Gastric ulcers are sores that form on the lining of the stomach, while duodenal ulcers are located in the duodenum. The different locations influence the presentation of symptoms and the risk factors associated with each type.
Risk Factors
Several risk factors increase the likelihood of developing peptic ulcers. One prominent factor is infection with Helicobacter pylori bacteria, which significantly increases the risk. Regular use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or aspirin, also significantly raises the risk. Smoking and excessive alcohol consumption are also considered risk factors. Certain medical conditions, such as Zollinger-Ellison syndrome, can increase stomach acid production, contributing to ulcer formation.
Comparison of Gastric and Duodenal Ulcers
| Feature | Gastric Ulcer | Duodenal Ulcer |
|---|---|---|
| Location | Stomach lining | Duodenum |
| Symptoms | Often associated with pain that worsens after meals, sometimes occurring in the middle of the night. May also exhibit nausea, vomiting, or bloating. | Typically characterized by pain that is relieved by eating. Pain often occurs several hours after meals or during the night, and can be described as gnawing or burning. |
| Typical Causes | Infection with Helicobacter pylori, NSAID use, stress, Zollinger-Ellison syndrome | Infection with Helicobacter pylori, NSAID use, stress, possibly less common association with Zollinger-Ellison syndrome |
Diagnostic Methods for Peptic Ulcers
Peptic ulcers, sores that develop on the lining of the stomach or duodenum, can cause significant discomfort and potentially lead to severe complications. Accurate diagnosis is crucial for appropriate treatment and preventing long-term issues. Several diagnostic methods are employed to identify peptic ulcers and determine their severity.Identifying the presence and characteristics of a peptic ulcer requires a multi-faceted approach involving various tests.
These tests help pinpoint the ulcer’s location, size, and potential complications. This process usually starts with a thorough medical history and physical examination, followed by specific diagnostic procedures.
Common Diagnostic Tests
A range of tests are employed to confirm the presence of a peptic ulcer. These tests vary in their invasiveness, cost, and accuracy, each with its own set of advantages and disadvantages. The most common tests include upper gastrointestinal (GI) series and endoscopy.
- Upper GI Series (Barium Swallow): This non-invasive test uses a contrast agent (barium) to coat the esophagus, stomach, and duodenum. X-rays are taken to visualize the digestive tract. The barium highlights any irregularities or abnormalities, including ulcers, in the lining of the digestive tract. It is relatively inexpensive and readily available, making it a useful initial screening tool. However, it may not detect subtle ulcers or provide detailed views of the ulcer’s characteristics, sometimes requiring follow-up endoscopy.
- Endoscopy: Endoscopy, particularly esophagogastroduodenoscopy (EGD), is a more invasive but highly accurate diagnostic tool. A thin, flexible tube with a camera (endoscope) is inserted through the mouth and into the esophagus, stomach, and duodenum. This allows direct visualization of the lining of the digestive tract, enabling clinicians to directly view the ulcer, assess its size and location, and take biopsies.
Surgery for peptic ulcers is a serious procedure, often a last resort when medication fails. While focusing on the physical discomfort, it’s important to consider the overall health picture, including potential sexually transmitted infections (STIs). Identifying and treating STIs early is crucial, as outlined in resources like this comprehensive guide on std symptoms in women identification diagnosis treatment.
Ultimately, a thorough understanding of potential co-occurring conditions helps ensure the best possible surgical outcomes and long-term health for patients.
Endoscopy provides detailed images, allowing for precise identification of the ulcer and assessment of its severity. However, it carries a small risk of complications such as bleeding or perforation, and it requires specialized equipment and trained personnel.
Role of Biopsies in Diagnosis
Biopsies are crucial in diagnosing peptic ulcers, particularly in cases where the exact cause or nature of the ulcer is uncertain. A small tissue sample is taken from the ulcerated area during endoscopy. The tissue sample is then examined under a microscope by a pathologist to identify the presence of inflammation, infection (such as Helicobacter pylori), or other abnormalities.
This microscopic analysis helps determine the underlying cause of the ulcer, guiding treatment decisions and monitoring for potential complications.
Comparison of Diagnostic Procedures
| Diagnostic Procedure | Advantages | Disadvantages |
|---|---|---|
| Upper GI Series | Non-invasive, relatively inexpensive, readily available | May not detect subtle ulcers, does not provide detailed views, may require follow-up endoscopy |
| Endoscopy | Provides detailed visualization, allows for direct assessment of ulcer characteristics, biopsies can be taken | More invasive, carries a small risk of complications (bleeding, perforation), requires specialized equipment and trained personnel |
Steps in a Typical Endoscopic Procedure for Peptic Ulcer Diagnosis
- Preparation: Patients are typically asked to fast for several hours before the procedure to minimize the risk of aspiration during the procedure.
- Sedation: The patient is given medication to induce mild sedation, ensuring comfort and minimizing discomfort.
- Insertion of Endoscope: A thin, flexible endoscope is carefully passed through the patient’s mouth and into the esophagus, stomach, and duodenum.
- Visualization: The endoscope allows the physician to visualize the lining of the digestive tract.
- Biopsy (if needed): If indicated, a small tissue sample (biopsy) is taken from the ulcerated area.
- Procedure Completion: The endoscope is carefully withdrawn, and the patient is monitored until the effects of sedation wear off.
Surgical Procedures for Peptic Ulcers: Surgery For Peptic Ulcers
Surgical interventions for peptic ulcers are typically reserved for cases where medical management fails to alleviate symptoms or complications arise. These procedures aim to address the underlying cause of the ulcer, promote healing, and prevent recurrence. The choice of surgical procedure depends on several factors, including the location and severity of the ulcer, the presence of complications, and the patient’s overall health.Surgical approaches for peptic ulcers generally involve either reducing the amount of acid produced by the stomach or altering the structure of the digestive tract to improve the healing process.
The selection of the optimal surgical technique often necessitates a thorough assessment of the patient’s medical history, physical examination, and diagnostic test results.
Antrectomy
Antrectomy involves the surgical removal of the antrum, the lower part of the stomach. This procedure is primarily targeted at reducing the production of gastric acid, as the antrum contains cells responsible for producing gastrin, a hormone that stimulates acid secretion. The rationale behind antrectomy is to decrease the amount of acid available to damage the ulcer site. Potential complications include dumping syndrome, characterized by rapid emptying of stomach contents into the small intestine, leading to symptoms like nausea, vomiting, and diarrhea.
Postoperative recovery can take several weeks, with a typical recovery time of 6-8 weeks. Long-term outcomes are generally positive, with a reduction in ulcer recurrence. However, the potential for malabsorption, resulting in nutrient deficiencies, requires ongoing monitoring.
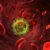
Vagotomy
Vagotomy involves severing the vagus nerves, which transmit signals to the stomach that stimulate acid secretion. The procedure aims to decrease the amount of acid produced by the stomach. Various types of vagotomy exist, including truncal, selective, and highly selective vagotomy. The rationale is to disrupt the neural pathway that triggers acid production. Potential complications include dumping syndrome, similar to those observed after antrectomy, and potentially, delayed gastric emptying.
So, I’ve been researching surgery for peptic ulcers lately, and it’s fascinating how much attention to detail is needed. It’s a similar kind of meticulousness you need when grocery shopping for people with food allergies – checking labels carefully and understanding ingredient lists is crucial. Grocery shopping for people with food allergies requires a lot of planning, and it’s really important to avoid cross-contamination.
Ultimately, surgery for peptic ulcers is a serious matter, but careful planning can make a huge difference in both cases.
Recovery time typically ranges from 4-6 weeks. Long-term outcomes often show a significant reduction in ulcer recurrence, although occasional complications like diarrhea and bloating may persist.
Pyloroplasty
Pyloroplasty involves widening the pyloric sphincter, the valve between the stomach and the small intestine. This procedure aims to improve the emptying of the stomach, which can be crucial in cases where the stomach empties too slowly. The rationale is to allow the stomach contents to pass more readily into the small intestine, thus reducing the likelihood of ulcer recurrence and promoting healing.
Potential complications include gastric reflux, a condition where stomach acid backs up into the esophagus, and possible obstruction. Recovery time generally ranges from 2-4 weeks. Long-term outcomes are usually good, with improved gastric emptying and reduced ulcer recurrence rates.
Comparison of Surgical Procedures
| Procedure | Effectiveness | Invasiveness | Recovery Time |
|---|---|---|---|
| Antrectomy | High | Moderate | 6-8 weeks |
| Vagotomy | High | Moderate | 4-6 weeks |
| Pyloroplasty | Moderate to High | Low | 2-4 weeks |
Pre- and Post-Operative Care

Preparing for surgery for peptic ulcers involves careful planning and meticulous attention to detail. This phase encompasses not only the physical preparations but also the emotional and mental well-being of the patient. A thorough understanding of pre- and post-operative care is crucial for a successful outcome and a smooth recovery.
Pre-Operative Preparations
Pre-operative preparations are essential for ensuring the safety and efficacy of the surgical procedure. These preparations involve a series of steps to optimize the patient’s physical condition and minimize potential risks. Proper preparation helps the surgical team to perform the procedure safely and efficiently, while reducing the risk of complications.
- Medical History Review: A comprehensive review of the patient’s medical history, including allergies, previous surgeries, and current medications, is critical. This allows the surgical team to identify potential risks and adjust the surgical plan accordingly. For instance, a patient with a history of bleeding disorders may require specific pre-operative blood work and medication adjustments.
- Dietary Restrictions: Strict adherence to a prescribed diet before surgery is vital. This usually involves a clear liquid diet and, in some cases, a complete fast for a specific duration before the procedure. This prevents complications from the presence of food in the stomach during surgery.
- Medications and Supplements: Patients must inform their doctors about all medications and supplements they are taking, including over-the-counter drugs and herbal remedies. This is because some medications can interfere with anesthesia or increase the risk of bleeding. The doctor will advise on which medications to discontinue or adjust before surgery.
- Blood Tests and Imaging: Various blood tests, including complete blood counts and clotting studies, are performed to assess the patient’s overall health and to evaluate their ability to heal. Imaging studies, such as X-rays or endoscopies, may also be conducted to provide a clear picture of the ulcer and its location.
- Emotional and Psychological Support: The emotional and psychological well-being of the patient is paramount. Preparing the patient mentally for the procedure, answering their questions, and offering reassurance can significantly reduce anxiety and improve the overall outcome.
Post-Operative Care
Post-operative care focuses on facilitating a smooth recovery and minimizing complications. This period demands close monitoring and diligent adherence to the prescribed care plan. The goal is to promote healing, manage pain, and prevent potential problems.
Surgery for peptic ulcers can be a necessary option, but it’s important to remember the potential side effects of the medications used to manage the condition. For example, some of these medications, like those used to reduce stomach acid, can cause hair loss, as detailed in this helpful resource on these medications can cause hair loss. While surgery can offer a long-term solution, careful consideration of all potential impacts, including medication side effects, is crucial for a complete understanding of the treatment process.
- Pain Management: Pain management is a critical aspect of post-operative care. Patients are typically provided with pain medication to manage discomfort. The type and dosage of medication will be determined by the patient’s individual needs and the nature of the surgery.
- Dietary Progression: Following surgery, the patient’s diet is gradually progressed from clear liquids to a regular diet, based on the recovery process and doctor’s instructions. This gradual introduction of food allows the digestive system to adjust and prevents complications from sudden changes in the diet.
- Activity Restrictions: Post-operative activity restrictions are typically implemented to allow the surgical site to heal properly. These restrictions may involve avoiding strenuous activities and lifting heavy objects. Following these guidelines helps to minimize the risk of complications.
- Monitoring for Complications: Post-operative monitoring is essential to detect and address potential complications early. This includes regular vital sign checks, observation for signs of infection, and evaluation of the surgical site.
- Follow-up Appointments: Scheduled follow-up appointments with the surgeon are essential for monitoring healing and addressing any concerns. This allows for early detection of potential complications and ensures the patient receives the necessary support and care.
Potential Complications
While surgery for peptic ulcers is generally safe, potential complications can occur. Recognizing and managing these complications promptly is crucial for a positive outcome.
- Bleeding: Post-operative bleeding is a possible complication, although less common with modern surgical techniques. Prompt intervention is required to control any bleeding.
- Infection: Surgical sites can become infected, requiring antibiotics to treat the infection.
- Nerve Damage: Nerve damage is a rare but possible complication, depending on the specific surgical approach. This is usually temporary and resolves with time.
- Adverse Reactions to Medications: Patients might experience adverse reactions to anesthesia or pain medications. These reactions are usually mild and treatable.
- Delayed Healing: Delayed healing at the surgical site can occur, requiring additional medical interventions.
Explaining Pre- and Post-Operative Care to Patients
Explaining pre- and post-operative care to patients in simple terms is crucial for ensuring they understand their role in the recovery process. Clear and concise communication builds trust and empowers patients to actively participate in their care. Using everyday language and avoiding medical jargon is important for effective communication.
| Aspect | Pre-Operative Care | Post-Operative Care |
|---|---|---|
| Preparation | Review of medical history, medications, diet, and blood tests | Pain management, gradual return to diet, activity restrictions |
| Diet | Clear liquid diet, fasting before surgery | Gradual progression from clear liquids to a regular diet |
| Activity | Rest and preparation for surgery | Limited activity to allow healing |
| Follow-up | Blood tests and imaging before surgery | Regular check-ups and monitoring for complications |
Alternatives to Surgery
Peptic ulcers, while sometimes requiring surgical intervention, are often treatable with non-surgical methods. These methods, focusing on medication and lifestyle changes, offer a less invasive approach to managing symptoms and promoting healing. Understanding the efficacy of these alternatives is crucial for patients considering surgical options.
Non-Surgical Treatment Options
Non-surgical treatments for peptic ulcers primarily involve medications and lifestyle modifications. These approaches aim to address the underlying causes of the ulcers, such as Helicobacter pylori infection or excessive stomach acid production, and alleviate symptoms. Medication plays a significant role in both symptom relief and healing, while lifestyle changes help maintain a healthy environment conducive to ulcer healing.
Medication for Peptic Ulcers
Medications are essential in the management of peptic ulcers. They can neutralize stomach acid, reduce acid production, or eradicate H. pylori infection, thereby promoting healing and preventing further ulcer development. Proton pump inhibitors (PPIs) are frequently prescribed to reduce stomach acid production. Antacids, often used for immediate symptom relief, neutralize existing acid. Antibiotics are used to treat H. pylori infections, a common cause of peptic ulcers.
Lifestyle Modifications for Ulcer Prevention
Adopting healthy lifestyle choices can significantly reduce the risk of developing peptic ulcers and promote healing. These lifestyle modifications include maintaining a balanced diet, avoiding smoking and excessive alcohol consumption, and managing stress effectively. Regular exercise and sufficient sleep contribute to overall well-being, which can indirectly influence the healing process.
Effectiveness Comparison: Medication vs. Surgery, Surgery for peptic ulcers
Medication, when properly administered and followed, is often highly effective in treating peptic ulcers. In many cases, it can successfully manage symptoms and promote healing, avoiding the need for surgery. Surgery is typically reserved for cases where medication fails to effectively control symptoms or where complications arise. The choice between medication and surgery depends on individual circumstances, the severity of the condition, and the patient’s response to medical treatment.
Role of Medications in Ulcer Management
Medications play a crucial role in managing symptoms and promoting ulcer healing. By reducing stomach acid production, neutralizing existing acid, or eradicating H. pylori, medications directly address the root causes of ulcer formation. This targeted approach allows for healing without the need for more invasive procedures.
Summary Table: Surgical vs. Non-Surgical Treatments
| Treatment Type | Pros | Cons |
|---|---|---|
| Surgical | Effective for severe cases or complications; quicker healing in some instances; potentially curative. | Invasive procedure; risk of complications (e.g., bleeding, infection); longer recovery time; higher cost. |
| Non-Surgical (Medication & Lifestyle Changes) | Less invasive; lower risk of complications; shorter recovery time; lower cost; often first-line treatment. | May not be effective for all cases; requires patient compliance with medication and lifestyle changes; healing process may take longer in some instances. |
Potential Complications and Outcomes
Surgery for peptic ulcers, while often effective, carries potential risks and complications. Understanding these risks is crucial for patients and healthcare providers to make informed decisions. Proper management and post-operative care can significantly reduce the likelihood of complications and improve long-term outcomes.The journey to recovery after peptic ulcer surgery isn’t always smooth sailing. While most patients experience a successful outcome, a range of potential complications can arise.
These complications, varying in severity, can impact recovery time and overall well-being. Proactive management of these potential complications is key to ensuring the best possible recovery.
Potential Complications
Post-operative complications, although relatively infrequent, can significantly impact recovery. They necessitate prompt diagnosis and treatment to prevent prolonged morbidity or even mortality. The likelihood of complications is influenced by factors like the patient’s overall health, the surgical approach, and the specific type of peptic ulcer.
- Bleeding: Post-operative bleeding is a serious concern, potentially requiring further intervention. Factors contributing to bleeding include inadequate hemostasis during the initial procedure, or the development of blood clots. Immediate medical attention is crucial to control bleeding and prevent significant blood loss. The severity of bleeding can range from minor to life-threatening.
- Infection: Infection at the surgical site is a common complication, and is often related to bacterial colonization. Prompt antibiotic treatment and meticulous wound care are essential for controlling infection. The infection may present as redness, swelling, or pus formation at the incision site, and requires immediate medical attention to prevent it from spreading.
- Gastrointestinal Issues: Problems like strictures (narrowing of the digestive tract) or fistulas (abnormal connections between organs) can develop after surgery. These issues can cause persistent discomfort and potentially require further surgical intervention. These complications may arise due to scar tissue formation, which can narrow or block the passageway of the gastrointestinal tract.
- Nerve Damage: In some cases, surgical procedures can inadvertently damage surrounding nerves, leading to pain, numbness, or other sensory disturbances in the abdominal area. Minimally invasive techniques are often employed to reduce the risk of nerve damage.
Long-Term Outcomes
The long-term success of peptic ulcer surgery hinges on a variety of factors. Proper management of underlying causes of ulcers, along with adherence to post-operative recommendations, significantly influences the long-term health of patients.
- Recurrence: A significant concern is the potential for peptic ulcers to recur. Factors like lifestyle choices, stress levels, and medication use can play a role in ulcer recurrence. Strict adherence to medical advice and lifestyle modifications are often crucial in preventing recurrence.
- Quality of Life: Surgical intervention aims to improve quality of life by reducing symptoms and preventing future complications. Long-term outcomes are often measured by a patient’s ability to resume normal activities and experience reduced discomfort.
- Follow-up Care: Regular follow-up appointments are critical to monitor for complications and adjust treatment plans as needed. This ensures that any issues are identified and addressed promptly. These follow-ups allow for ongoing assessment of the patient’s health and allow for adjustments to any medical or lifestyle factors.
Importance of Follow-up Care
Post-operative follow-up care is vital to monitor for potential complications, adjust treatment plans, and ensure the patient’s long-term well-being. It allows for ongoing assessment of the patient’s health and adjustment of medical or lifestyle factors to prevent recurrence.
Factors Influencing Long-Term Success
Various factors play a crucial role in determining the long-term success of surgical intervention for peptic ulcers. These factors include the patient’s overall health, adherence to post-operative recommendations, and the management of any underlying conditions.
- Patient Compliance: The patient’s active participation in their recovery and adherence to prescribed medications and lifestyle changes significantly impact long-term outcomes. This includes taking medications as directed, and following dietary recommendations.
- Underlying Conditions: The presence of other medical conditions can influence the course of recovery and the risk of complications. This highlights the importance of thorough pre-operative assessments.
- Surgical Technique: The expertise and skill of the surgical team play a role in minimizing complications and maximizing the chances of a successful outcome. The specific surgical technique employed can affect the long-term success rate.
Potential Complications Table
This table provides an overview of potential complications and their estimated likelihood following surgery for peptic ulcers.
| Potential Complication | Likelihood (Estimated) |
|---|---|
| Bleeding | Low to moderate |
| Infection | Moderate |
| Gastrointestinal Issues (strictures/fistulas) | Low to moderate |
| Nerve Damage | Low |
Illustrations and Visual Aids
Visual aids are crucial for understanding complex medical conditions like peptic ulcers. Illustrations, diagrams, and even simple anatomical drawings can make abstract concepts more tangible, aiding both patient comprehension and physician communication. These visual tools facilitate a more informed decision-making process, bridging the gap between technical information and patient understanding.
Stomach and Duodenum Anatomy
Understanding the location of peptic ulcers requires a clear visualization of the stomach and duodenum. The stomach, a J-shaped organ, is situated in the upper left quadrant of the abdomen, connected to the duodenum, the first part of the small intestine. Peptic ulcers can occur anywhere along the lining of the stomach and duodenum. A diagram would show the stomach and duodenum in relation to other abdominal organs, highlighting the precise locations where ulcers commonly develop.
The diagram would also label the various layers of the stomach and duodenum, such as the mucosa, submucosa, and muscularis.
Endoscopic View of a Peptic Ulcer
A detailed endoscopic view of a peptic ulcer provides a direct visualization of the ulcer’s appearance. A typical endoscopic image would showcase a crater-like lesion, often with irregular edges, in the lining of the stomach or duodenum. The ulcer’s size, depth, and surrounding inflammation would be clearly depicted. The surrounding tissues would be marked, and the ulcer’s location in relation to the surrounding structures would be highlighted.
Surgical Procedure Steps
Illustrating the steps involved in a surgical procedure for a peptic ulcer, such as a partial gastrectomy, is essential. A step-by-step diagram would depict the incisions, the mobilization of the stomach and/or duodenum, the surgical resection of the affected tissue, and the reconstruction of the digestive tract. Each step would be labeled clearly with a concise description. This would help surgeons visualize the procedure, and allow patients to understand the surgical approach.
Explaining Surgical Approaches to Patients
Visual aids are key to explaining different surgical approaches to patients. A series of diagrams comparing different surgical techniques, such as laparoscopic versus open surgery, would be helpful. The diagrams would showcase the incisions involved in each technique, the instruments used, and the overall approach. These illustrations would help patients grasp the differences between the procedures and make informed decisions about their treatment.
An additional diagram could illustrate the potential benefits and risks of each approach.
Comparing Surgical Techniques
A visual comparison of different surgical techniques, such as laparoscopic versus open surgery, would be presented in a table format. The table would compare the surgical approach, length of recovery, and potential complications for each technique. A chart or graphic would also be useful to illustrate the comparative success rates and long-term outcomes of each procedure. This visual aid would help patients weigh the pros and cons of each approach and make an informed decision.
Examples of patients who underwent each procedure would help support the information.
Closure
In conclusion, surgery for peptic ulcers can be a life-changing intervention for individuals suffering from this condition. By understanding the various aspects of this procedure, from diagnosis to recovery, you can approach this journey with greater confidence and clarity. Remember, this information is for educational purposes only and should not replace professional medical advice. Consult with your healthcare provider to discuss the best course of action for your specific needs.