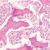
Types of macular degeneration sets the stage for this enthralling narrative, offering readers a glimpse into the various forms of this debilitating eye condition. Macular degeneration significantly impacts vision, affecting daily life in profound ways. Understanding the different types, from the gradual progression of dry macular degeneration to the sudden onset of wet macular degeneration, is crucial for proactive management and seeking appropriate support.
This exploration will delve into the causes, symptoms, and potential treatments for each type, empowering readers with knowledge and hope.
This comprehensive guide will cover the different types of macular degeneration, including dry and wet forms, as well as other less common variations. We’ll examine the causes, progression, symptoms, and treatment options for each type. A detailed table format will illustrate the differences in prevalence, symptoms, and impact on vision for easier comparison. Armed with this information, you can better understand your own risk and make informed decisions about your eye health.
Introduction to Macular Degeneration
Macular degeneration is a progressive eye disease that affects the macula, the central part of the retina responsible for sharp, detailed vision. This area of the retina is crucial for tasks like reading, driving, and recognizing faces. Damage to the macula leads to a gradual loss of central vision, making everyday activities more challenging. Understanding the different types of macular degeneration is vital for early diagnosis and appropriate management.The impact of macular degeneration on vision varies significantly depending on the type and progression.
It can range from subtle blurring to a complete loss of central vision, impacting an individual’s ability to perform daily tasks, participate in social activities, and maintain their independence. Different types of macular degeneration affect the macula in unique ways, leading to different patterns of vision loss. Early detection and management strategies can slow the progression and help maintain functional vision.
Types of Macular Degeneration
Macular degeneration presents in several forms, each with distinct characteristics. Understanding these variations is critical for appropriate treatment and management.
Dry Macular Degeneration
Dry macular degeneration, the most common type, is characterized by a gradual thinning and deterioration of the macula. This process involves the loss of light-sensitive cells in the macula, which results in blurry or distorted central vision. The progression is typically slow, with vision loss occurring gradually over time. Small, yellowish deposits called drusen can accumulate under the macula, and these can contribute to the thinning and deterioration.
Wet Macular Degeneration
Wet macular degeneration, a more severe form, involves abnormal blood vessel growth under the macula. These new, fragile vessels leak fluid and blood, causing rapid and substantial vision loss. The leakage damages the light-sensitive cells, leading to sudden and significant vision impairment. This type requires prompt medical intervention to prevent further damage.
Prevalence of Macular Degeneration Types
The prevalence of macular degeneration varies by type and population. Data from various studies indicates that dry macular degeneration is significantly more prevalent than wet macular degeneration.
| Type | Description | Prevalence |
|---|---|---|
| Dry Macular Degeneration | Gradual thinning and deterioration of the macula, characterized by the loss of light-sensitive cells and the accumulation of drusen. | More prevalent, often progresses slowly. |
| Wet Macular Degeneration | Abnormal blood vessel growth under the macula, leading to fluid and blood leakage, causing rapid vision loss. | Less prevalent, but more severe and progressive. |
Dry Macular Degeneration
Dry macular degeneration, a more common form of age-related macular degeneration, is characterized by the gradual thinning and deterioration of the macula, the central part of the retina responsible for sharp, central vision. Unlike wet macular degeneration, which involves abnormal blood vessel growth, dry macular degeneration progresses more subtly, often with less dramatic initial symptoms. Understanding the causes, stages, and progression of dry AMD is crucial for early detection and management.
Causes of Dry Macular Degeneration
The precise causes of dry macular degeneration are not fully understood, but several factors contribute to its development. Age is a significant risk factor, and genetic predisposition likely plays a role. Exposure to sunlight and oxidative stress are also suspected contributors. Smoking and a diet lacking in essential nutrients may exacerbate the degenerative process. Research suggests that a combination of these factors, rather than a single cause, likely underlies the development of dry AMD.
Stages of Dry Macular Degeneration
Dry macular degeneration progresses through several stages, each with its own visual impact. These stages are generally classified as early, intermediate, and late dry macular degeneration. The progression is often gradual and may not be noticeable in the early stages.
Early Dry Macular Degeneration
Early dry macular degeneration is characterized by the gradual loss of small retinal pigment epithelial cells. This initial stage may not significantly affect vision. The loss of these cells can cause small, blurry or distorted areas in the central vision, and some patients may experience difficulty with fine detail, such as reading or recognizing faces.
Intermediate Dry Macular Degeneration
Intermediate dry macular degeneration is marked by a greater loss of retinal pigment epithelial cells, leading to the formation of small, yellowish deposits called drusen. These drusen deposits are typically visible with an ophthalmoscopic examination. Visual distortions or loss of detail become more apparent. Patients may experience difficulty reading small print or distinguishing subtle colors.
Late Dry Macular Degeneration
Late dry macular degeneration, also known as geographic atrophy, involves a more substantial loss of retinal pigment epithelial cells. The central part of the macula shows a distinctive, dry, atrophic area. This leads to significant vision loss and difficulty with tasks requiring sharp central vision, such as driving or recognizing faces.
Progression of Dry Macular Degeneration
The progression of dry macular degeneration is typically slow and gradual. It can take many years for the condition to significantly impair vision. The rate of progression varies greatly among individuals, influenced by genetic factors, lifestyle choices, and other health conditions. Some patients experience a relatively stable visual function over extended periods, while others may experience more rapid deterioration.
Risk Factors for Dry Macular Degeneration
Several risk factors are associated with the development of dry macular degeneration. Age is the most significant risk factor, as the risk increases substantially with advancing age. Genetic predisposition also plays a crucial role, with a family history of macular degeneration increasing the risk. Smoking is a major risk factor and negatively impacts overall eye health. A diet deficient in essential nutrients, such as vitamins C and E, may increase susceptibility.
Certain medical conditions, such as high blood pressure and high cholesterol, might also contribute to the development of dry macular degeneration.
Visual Acuity Loss in Dry Macular Degeneration
| Stage | Visual Acuity Loss Description |
|---|---|
| Early | Minimal or no noticeable vision loss; may experience slight blurring or distortion in central vision. |
| Intermediate | Increasing difficulty with fine details, reading, and distinguishing subtle colors; noticeable visual distortions. |
| Late (Geographic Atrophy) | Significant vision loss in the central visual field; difficulty with everyday tasks requiring sharp central vision. |
Wet Macular Degeneration
Wet macular degeneration, a more aggressive form of macular degeneration, is characterized by the abnormal growth of blood vessels behind the macula. These fragile new vessels leak fluid and blood, damaging the light-sensitive cells in the macula, leading to rapid and significant vision loss. Understanding the causes, mechanisms, and symptoms of wet macular degeneration is crucial for timely diagnosis and treatment.
Causes of Wet Macular Degeneration
The exact cause of wet macular degeneration remains unknown. However, several risk factors contribute to its development. Age is a significant factor, with the prevalence increasing with advancing years. Genetics play a role, as individuals with a family history of macular degeneration are at a higher risk. Smoking is a well-established risk factor, and uncontrolled high blood pressure, diabetes, and obesity have also been linked to the condition.
Exposure to intense sunlight or ultraviolet radiation over a lifetime may also be a contributing factor.
Mechanisms of New Blood Vessel Formation
The formation of abnormal blood vessels in wet macular degeneration is a complex process involving multiple signaling pathways. Vascular endothelial growth factor (VEGF) is a key protein in this process. Elevated levels of VEGF stimulate the growth of new blood vessels, which penetrate the retina and leak fluid and blood into the macula. This process is often triggered by chronic inflammation and oxidative stress, both of which are implicated in the aging process and other diseases.
These new vessels are fragile and prone to leakage, leading to the vision loss associated with wet macular degeneration.
Rapid Progression of Vision Loss
The rapid progression of vision loss in wet macular degeneration is a distinguishing feature from dry macular degeneration. The leakage of fluid and blood into the macula damages the photoreceptor cells, leading to a rapid decline in central vision. The extent of vision loss varies between individuals, but the progression can be swift, impacting daily activities like reading, driving, and recognizing faces.
The rapid nature of the vision loss in wet macular degeneration necessitates prompt medical attention and treatment.
Learning about the different types of macular degeneration is crucial for understanding eye health. While researching this, I stumbled across an interesting question: should I take vitamins during cancer treatment? This led me to a great resource that dives deep into the potential benefits and risks of vitamin supplementation during cancer treatment – check out should i take vitamins during cancer treatment.
Ultimately, understanding the various forms of macular degeneration, from wet to dry, helps you make informed decisions about your eye care and overall health.
Symptoms of Wet Macular Degeneration
Symptoms of wet macular degeneration typically include a sudden or gradual blurring or distortion of central vision. Individuals may experience a dark or blurry spot in their central vision, or straight lines might appear wavy. This distortion can affect reading, driving, or recognizing faces. The symptoms can vary in severity and progression. In some cases, the vision loss can be severe, leading to legal blindness.
Comparison of Dry and Wet Macular Degeneration
| Feature | Dry Macular Degeneration | Wet Macular Degeneration |
|---|---|---|
| Cause | Age-related changes in the macula, genetic factors, oxidative stress | Elevated VEGF levels, chronic inflammation, oxidative stress |
| Progression | Slow, gradual vision loss | Rapid, significant vision loss |
| Symptoms | Blurring, reduced detail, central vision loss | Blurring, distortion, dark spots, wavy lines, rapid vision loss |
| Treatment | Often involves monitoring and managing risk factors | Often involves anti-VEGF therapy and other treatments |
Other Forms of Macular Degeneration
Beyond the common dry and wet macular degeneration, several less prevalent forms exist, each with unique characteristics impacting vision. Understanding these variations is crucial for comprehensive eye health management and tailored treatment strategies. These lesser-known types often require specialized expertise for diagnosis and management.
Geographic Atrophy
Geographic atrophy (GA) is a progressive form of macular degeneration characterized by the gradual loss of retinal pigment epithelium (RPE) cells in specific areas of the macula. This loss leads to the formation of characteristic, clearly defined, and often pigmented areas of atrophy. The progression of GA typically involves the gradual enlargement of these atrophic regions, resulting in a significant decline in central vision.
- Description: GA is characterized by the loss of the retinal pigment epithelium (RPE) cells in specific areas of the macula, leading to the formation of visible atrophic regions. These regions are often pigmented and well-defined.
- Impact on Vision: GA typically results in a progressive loss of central vision, impairing tasks that require sharp focus, such as reading, driving, and recognizing faces.
- Progression Rate: The progression of GA is often slower compared to wet macular degeneration, but it can still lead to significant visual impairment over time. It’s crucial to monitor patients with GA closely to track the progression of the disease. Some individuals may experience periods of slower progression or even stability, while others may experience more rapid deterioration.
Central Serous Chorioretinopathy (CSCR)
Central serous chorioretinopathy (CSCR) is a condition where fluid builds up beneath the macula, causing a temporary swelling. While often considered a type of macular edema, the underlying cause and clinical course differ from other macular degenerations. In most cases, CSCR resolves without permanent vision loss. However, it’s important to monitor individuals with CSCR to ensure that no complications arise.
- Description: CSCR involves fluid accumulation beneath the macula, leading to swelling. The fluid is typically serous (clear), not blood-filled, and the condition is often associated with stress or other systemic factors.
- Impact on Vision: Fluid accumulation can temporarily blur central vision, but in most cases, the vision returns to near normal as the fluid resolves. However, some individuals may experience persistent vision changes or scarring that can lead to permanent vision loss.
- Progression Rate: CSCR often resolves spontaneously, and vision loss is usually temporary. However, the condition may recur in some individuals, potentially leading to permanent vision loss if not managed appropriately. Careful monitoring is crucial to identify and manage potential complications.
Other Less Common Forms
Several other, less common, forms of macular degeneration exist, including those related to systemic conditions like Stargardt disease or Best disease. These conditions, while impacting the macula, have distinct genetic or developmental origins, and management approaches.
- Stargardt Disease: This inherited retinal disorder is characterized by progressive vision loss in the central visual field, usually affecting individuals during childhood or adolescence. It is a type of macular dystrophy.
- Best Disease: Best disease is another inherited macular dystrophy. It is characterized by macular pigmentary changes and progressive vision loss. These conditions, while impacting the macula, have distinct genetic or developmental origins, and management approaches.
Symptoms and Diagnosis: Types Of Macular Degeneration
Understanding the symptoms and diagnostic process of macular degeneration is crucial for early intervention and management. Early detection significantly improves treatment options and can help preserve vision. A comprehensive understanding of the symptoms and how they manifest in different types of macular degeneration is essential for accurate diagnosis.
Common Symptoms of Macular Degeneration
Macular degeneration, affecting the central part of the retina, often presents with subtle changes in vision initially. Patients may notice difficulty with tasks requiring detailed vision, such as reading, driving, or recognizing faces. Gradual blurring or distortion of central vision are common initial symptoms. These subtle changes can sometimes be overlooked, leading to delayed diagnosis. Peripheral vision, however, typically remains unaffected in the early stages.
Diagnostic Methods for Macular Degeneration
Accurate diagnosis of macular degeneration involves a combination of thorough eye examinations and specialized tests. Comprehensive eye exams are fundamental to detecting early signs of macular damage. These exams typically include visual acuity testing, assessing the sharpness of vision, and dilated fundus examinations, which provide a detailed view of the retina. Additional tests might be necessary to confirm the diagnosis and differentiate between dry and wet forms.
Comparing Symptoms in Different Types
| Feature | Dry Macular Degeneration | Wet Macular Degeneration ||—|—|—|| Initial Symptoms | Gradual blurring or distortion of central vision, difficulty with fine details | Sudden vision changes, distorted or blurred central vision, straight lines appearing wavy || Progression | Slow and gradual | Rapid and potentially severe || Visual Acuity | Typically reduced over time | May experience a sudden and significant drop in visual acuity || Appearance of the Macula | Often appears normal or slightly affected in early stages.
May show drusen (small deposits) | May show abnormal blood vessel growth or leakage (neovascularization) in the macula. |
Role of Eye Exams in Diagnosis
Comprehensive eye exams are pivotal in diagnosing macular degeneration. These exams evaluate the health of the retina, specifically the macula. During a dilated fundus examination, an ophthalmologist or optometrist uses special eye drops to widen the pupils, allowing for a clear view of the retina. This examination allows for the detection of characteristic signs, such as drusen (small yellow deposits) in dry AMD or abnormal blood vessel growth in wet AMD.
The doctor meticulously examines the macula for any abnormalities.
Step-by-Step Procedure for Diagnosis
Step 1: Comprehensive eye examination, including visual acuity testing. Step 2: Dilated fundus examination using an ophthalmoscope to visualize the retina and macula. The doctor will carefully assess the macula for signs of drusen, neovascularization, or other abnormalities. Step 3: Specialized tests, such as optical coherence tomography (OCT), may be used to obtain cross-sectional images of the retina. These images help in identifying the presence and extent of macular damage.
Step 4: Further investigations, including fluorescein angiography (FA), may be performed to visualize the blood vessels in the retina. This helps identify any leakage or abnormal blood vessel growth, characteristic of wet macular degeneration. Step 5: Discussion with the patient about their medical history and family history. The doctor will also inquire about any recent changes in vision. Step 6: A diagnosis is made based on the findings from the comprehensive eye examination, the specialized tests, and the patient’s medical history.
Treatment Options
Unfortunately, there’s no cure for macular degeneration, but several treatment options can help slow its progression and preserve vision. The specific approach depends heavily on the type of macular degeneration and its stage. Early intervention is crucial for maximizing the effectiveness of these treatments.Effective treatment for macular degeneration often involves a multifaceted approach, combining various strategies to address the underlying causes and symptoms.
This tailored approach is designed to help slow the progression of vision loss and maintain the best possible visual function.
Current Treatment Options for Dry Macular Degeneration
Dry macular degeneration, the most common form, typically doesn’t require immediate treatment, as the damage is often slow and gradual. However, lifestyle modifications, such as a healthy diet rich in antioxidants and vitamins, and regular exercise, can help slow the progression of the disease. Nutritional supplements, particularly those containing antioxidants like lutein and zeaxanthin, may also play a beneficial role.
Current Treatment Options for Wet Macular Degeneration
Wet macular degeneration, characterized by abnormal blood vessel growth, is often treated with anti-VEGF injections. These injections target and neutralize vascular endothelial growth factor (VEGF), a protein that promotes the growth of these problematic vessels. Regular injections are typically required to maintain the benefits.
Importance of Early Intervention
Early diagnosis and treatment are critical in managing macular degeneration. Early intervention can significantly impact the course of the disease, potentially delaying or even preventing further vision loss. The sooner treatment begins, the more likely it is that vision can be preserved.
Understanding the different types of macular degeneration is crucial for effective treatment. While exploring these eye conditions, it’s interesting to consider the similarities and differences between antibiotics like azithromycin and amoxicillin, which can be used to treat various infections. For a deeper dive into azithromycin vs amoxicillin, check out this helpful comparison: azithromycin vs amoxicillin similarities and differences.
Ultimately, recognizing the various forms of macular degeneration remains paramount for proactive eye health management.
Preserving Vision with Treatments
The goal of treatment for macular degeneration is to slow the progression of vision loss and, in some cases, to potentially improve or stabilize existing vision. By targeting the specific underlying causes and symptoms, treatments aim to minimize the impact of the disease on daily life and maintain the best possible quality of life.
Treatment Comparison Table
| Treatment Type | Description | Suitability for Dry Macular Degeneration | Suitability for Wet Macular Degeneration |
|---|---|---|---|
| Anti-VEGF injections | Injections targeting vascular endothelial growth factor (VEGF) to stop abnormal blood vessel growth. | Not typically used, as dry macular degeneration is not characterized by abnormal blood vessel growth. | Highly effective, often used to stop progression and reduce leakage. |
| Nutritional Supplements (e.g., antioxidants) | Supplements containing antioxidants like lutein and zeaxanthin. | Potentially beneficial to slow progression. | May be beneficial as an adjunct therapy, but not a primary treatment. |
| Lifestyle Modifications | Adopting a healthy lifestyle, including a balanced diet and regular exercise. | Highly recommended to slow the progression. | Helpful to manage overall health and reduce other risk factors. |
Prevention and Management
Protecting your vision from macular degeneration involves a proactive approach that combines lifestyle choices, preventative measures, and diligent monitoring. Early detection and management play a crucial role in preserving your vision and maintaining an active lifestyle. While there’s no guaranteed cure for macular degeneration, many strategies can mitigate its progression and its impact on daily life.Understanding the risk factors and adopting a healthier lifestyle can significantly reduce your chances of developing macular degeneration.
This includes maintaining a balanced diet, staying physically active, and protecting your eyes from harmful UV radiation. Consistent eye exams are equally important in detecting early signs and enabling timely intervention.
Risk Factors
Age is a significant risk factor for macular degeneration. Genetics also plays a role, with a family history of the condition increasing the likelihood of developing it. Smoking, high blood pressure, and high cholesterol levels can increase the risk of macular degeneration. Certain medical conditions, such as diabetes and obesity, can also contribute to the development of the disease.
Exposure to intense sunlight over a lifetime, without adequate eye protection, can increase the risk. A diet deficient in certain nutrients, like antioxidants and vitamins, may also contribute to the development of age-related macular degeneration.
Lifestyle Choices
Adopting a healthy lifestyle can reduce the risk of macular degeneration. Maintaining a balanced diet rich in fruits, vegetables, and omega-3 fatty acids can be beneficial. Regular physical activity helps manage weight and blood pressure, reducing the strain on the cardiovascular system. Quitting smoking is a crucial step in lowering the risk, as smoking significantly increases the chances of developing the condition.
Protecting your eyes from UV radiation through sunglasses or hats is important to prevent further damage to the macula.
Managing Macular Degeneration
Managing macular degeneration focuses on slowing its progression and alleviating its symptoms. This involves adhering to prescribed treatment plans, if any, and making lifestyle adjustments to maintain overall health. Regular monitoring of the condition through comprehensive eye exams is vital. Patients may benefit from support groups or counseling services to cope with the emotional and practical challenges of the disease.
Adapting to visual changes may involve assistive devices and technologies.
Understanding the different types of macular degeneration is crucial for effective treatment. One key aspect to consider is how the immune system might play a role. For example, sometimes the body’s own immune response, triggered by a foreign substance like an antigen, what is an antigen , can damage the cells in the macula. This understanding is important for exploring potential treatments that target the immune system and ultimately prevent or slow the progression of macular degeneration.
Importance of Regular Eye Exams
Regular eye exams are essential for early detection of macular degeneration. Early diagnosis allows for prompt intervention and management, which can significantly slow the progression of the disease and preserve vision. During an eye exam, an ophthalmologist or optometrist will perform tests to assess the health of the macula. These tests can detect subtle changes in vision and identify potential signs of macular degeneration before significant vision loss occurs.
Preventative Measures
- Maintaining a healthy weight and blood pressure levels is crucial. Studies show a strong correlation between these factors and a reduced risk of age-related macular degeneration.
- Adopting a balanced diet rich in fruits, vegetables, and omega-3 fatty acids can help maintain eye health and reduce the risk of macular degeneration.
- Quitting smoking is a vital preventative step. Smoking significantly increases the risk of developing macular degeneration, so quitting smoking can drastically lower the likelihood of the condition.
- Protecting your eyes from UV radiation through the use of sunglasses and hats is essential to prevent further damage to the macula.
- Regular eye exams are critical for early detection and management of macular degeneration. Early intervention can significantly slow the progression of the disease and preserve vision.
Visual Impact and Quality of Life
Macular degeneration significantly impacts a person’s daily life, affecting their ability to perform routine tasks and impacting their overall well-being. The visual changes can lead to profound emotional and psychological challenges, requiring adjustments and support systems to maintain a good quality of life. This section explores the multifaceted effects of macular degeneration on daily activities, emotional states, and available resources.
Impact on Daily Activities
The progressive loss of central vision in macular degeneration can make everyday tasks challenging. Reading, driving, recognizing faces, and performing fine motor skills like buttoning clothes become increasingly difficult. Simple activities like cooking or preparing meals can become cumbersome due to the inability to clearly see ingredients or the stovetop. These limitations can lead to feelings of isolation and dependence, potentially impacting a person’s independence and participation in social activities.
Emotional and Psychological Effects
The visual changes associated with macular degeneration can evoke a range of emotional responses. Depression, anxiety, and feelings of isolation are common among individuals experiencing vision loss. The loss of independence and the inability to perform familiar tasks can lead to frustration and grief. It’s crucial to acknowledge and address these emotional responses, providing support and resources to cope with the challenges.
Support Systems
A strong support system is vital for individuals with macular degeneration. Family, friends, and support groups can provide emotional comfort and practical assistance. Local organizations dedicated to vision loss often offer valuable resources, including information, support groups, and practical advice. Furthermore, ophthalmologists and other healthcare professionals can play a critical role in guiding patients through the process and connecting them with relevant resources.
Assistive Technologies, Types of macular degeneration
Assistive technologies can significantly improve the quality of life for individuals with macular degeneration. Magnifying glasses, large-print materials, and screen readers are common examples that can help compensate for visual impairment. Advanced technologies like optical character recognition software and specialized computer programs can assist with reading and navigating digital content. These tools can help maintain independence and participation in daily life.
Infographic: Impact of Macular Degeneration on Daily Life
| Activity | Impact | Example |
|---|---|---|
| Reading | Difficulty with fine print, reduced comprehension | Struggling to read books or newspapers, requiring larger fonts or assistive technologies. |
| Driving | Impaired ability to see road signs and other critical visual cues. | Increased risk of accidents and difficulty navigating intersections. |
| Cooking | Inability to see ingredients clearly, increased risk of accidents. | Difficulty measuring ingredients, potentially leading to burns or mistakes in recipes. |
| Social Interactions | Difficulty recognizing faces, potentially leading to feelings of isolation. | Reduced participation in social events, leading to feelings of loneliness and isolation. |
| Daily tasks | Significant impairment in performing tasks that require precise vision. | Difficulty buttoning clothes, using utensils, and performing other daily tasks. |
Summary
In conclusion, macular degeneration, though a serious condition, is not insurmountable. Understanding the different types, their unique characteristics, and available treatment options is paramount. This knowledge empowers individuals to proactively manage their vision and seek necessary support. By fostering awareness and promoting early intervention, we can work towards a future where individuals living with macular degeneration maintain a high quality of life.
Remember, regular eye exams are critical in early detection and management. This journey of understanding macular degeneration is a vital step toward better eye care and well-being.