Types of surgery pain can significantly impact a patient’s experience, from the initial procedure to the long-term recovery. Understanding the different kinds of pain, how they’re managed, and how patients perceive them is crucial for providing effective care. This exploration will cover everything from acute post-operative discomfort to chronic pain conditions, and the unique needs of diverse patient groups.
This in-depth look at surgical pain will help readers grasp the complexities involved in pain management. We’ll discuss various pain pathways, physiological responses, and different pain assessment methods, equipping you with a better understanding of the science behind surgical pain and how it affects patients.
Types of Surgical Pain
Surgical procedures, while essential for restoring health, often involve pain. Understanding the various types of surgical pain, their pathways, and physiological responses is crucial for effective pain management. This knowledge allows healthcare professionals to tailor treatment strategies for optimal patient outcomes.
Different surgeries bring different kinds of pain, from the sharp, immediate sting of a small incision to the dull, lingering ache of a major procedure. Managing post-operative discomfort is crucial, and understanding the various types of pain can help in effective pain management strategies. For instance, some chronic conditions, like those related to vitamin b12 and multiple sclerosis , can also influence pain perception after surgery.
Ultimately, open communication with your healthcare team is key to navigating the pain experience after any surgical procedure.
Classification of Surgical Pain
Surgical pain can be broadly classified into acute and chronic pain. Acute pain arises immediately after surgery and typically subsides within a few weeks. Chronic pain, on the other hand, persists beyond the expected healing period, sometimes lasting for months or years. The transition from acute to chronic pain can be influenced by various factors, including the surgical procedure, the patient’s pre-existing conditions, and their individual pain response.
Pain Pathways in Surgical Procedures
Surgical procedures activate different pain pathways in the body. These pathways involve nociceptors, specialized nerve endings that detect noxious stimuli. Nociceptors transmit pain signals through the peripheral nerves to the spinal cord and then to the brain. The specific pathways involved vary depending on the location and type of surgery. For example, orthopedic procedures might involve pathways related to musculoskeletal tissues, while cardiac surgeries may engage pathways related to the heart and surrounding structures.
The differences in activation of these pathways lead to varying experiences of pain intensity and location.
Post-surgery pain comes in various forms, from sharp, stabbing aches to dull, throbbing sensations. Understanding how your body heals is key, and that includes the vital role of protein in tissue repair. Knowing what does protein do is crucial for recovery, and a better understanding of your body’s nutritional needs during this time can help manage pain more effectively.
So, if you’re looking for ways to support your body’s natural healing process, explore what does protein do to learn more about the critical role of protein in post-surgical recovery. Ultimately, managing these different types of surgery pain often requires a multifaceted approach.
Physiological Responses to Surgical Pain
The body responds physiologically to surgical pain, often triggering a stress response. This response involves the release of hormones like cortisol and adrenaline, which can lead to increased heart rate, blood pressure, and respiratory rate. These physiological changes are a natural defense mechanism but can also contribute to the perception of pain and discomfort. Understanding these responses is crucial for implementing strategies to mitigate their negative effects.
Post-Operative Pain in Different Surgical Specialties
Post-operative pain characteristics differ depending on the surgical specialty. In orthopedic surgeries, pain often manifests as localized tenderness and stiffness, particularly in the affected joint. Cardiac surgeries, while potentially leading to chest pain, might also involve pain in the arms or shoulders. Abdominal surgeries can result in a variety of pain sensations, from diffuse abdominal cramping to sharp, localized pain, depending on the specific procedure and involved organs.
These differences highlight the importance of personalized pain management strategies tailored to the individual procedure.
Table of Common Types of Surgical Pain
| Type of Pain | Characteristics | Potential Causes |
|---|---|---|
| Acute Post-Operative Pain | Sharp, localized pain immediately following surgery; typically subsides within a few weeks. | Surgical incision, tissue trauma, inflammation, and surgical manipulation. |
| Chronic Post-Operative Pain | Persistent pain lasting beyond the expected healing period. | Neurological damage, nerve compression, scar tissue formation, psychological factors. |
| Phantom Limb Pain | Pain felt in a limb that has been amputated. | Abnormal nerve activity in the remaining nerves and psychological factors. |
| Neuropathic Pain | Pain that arises from damage to the nerves themselves, often described as burning, tingling, or shooting pain. | Nerve damage from surgery, nerve compression, or diabetes. |
Pain Management Strategies
Surgical procedures, while essential for patient well-being, often lead to varying degrees of postoperative pain. Effective pain management is crucial for a smooth recovery and minimizing long-term complications. This involves a multifaceted approach that encompasses pharmacological and non-pharmacological strategies, tailored to the individual patient’s needs.A comprehensive pain management plan is essential to ensure patient comfort and facilitate a faster recovery.
This approach acknowledges the diverse needs of each patient and employs a combination of medication and non-medication techniques to address pain effectively. Careful consideration of individual factors, including the type of surgery, the patient’s medical history, and their preferences, is critical to optimize the plan’s success.
Pharmacological Approaches to Surgical Pain Management
Pharmacological strategies play a vital role in managing surgical pain. Different classes of medications are employed, each with unique mechanisms of action and potential side effects. Opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and adjuvants are commonly used in various combinations.
Non-Pharmacological Methods for Managing Surgical Pain
Non-pharmacological approaches to pain management are often complementary to pharmacological interventions. These methods aim to reduce pain perception and improve overall well-being. Physical therapy, for instance, helps restore mobility and function, promoting recovery and reducing pain. Psychological interventions, including relaxation techniques and cognitive behavioral therapy (CBT), can address anxiety and stress, which are frequently linked to heightened pain perception.
Principles of Multimodal Analgesia in Surgical Pain Management
Multimodal analgesia represents a sophisticated approach to pain management. It involves the strategic combination of different analgesic agents with distinct mechanisms of action. This approach aims to achieve a synergistic effect, reducing the overall dosage of individual medications while maximizing pain relief and minimizing side effects. The goal is to target multiple pain pathways, providing comprehensive pain control.
Comparison of Analgesic Medications
| Medication | Mechanism of Action | Potential Side Effects |
|---|---|---|
| Opioids (e.g., Morphine, Fentanyl) | Bind to opioid receptors in the central nervous system, reducing pain signals. | Respiratory depression, nausea, constipation, sedation, tolerance, and dependence. |
| NSAIDs (e.g., Ibuprofen, Naproxen) | Inhibit cyclooxygenase enzymes, reducing inflammation and pain. | Gastrointestinal upset, kidney damage, allergic reactions. |
| Local Anesthetics (e.g., Lidocaine, Bupivacaine) | Block nerve impulses, providing pain relief in a specific area. | Local tissue reactions, allergic reactions, and in high doses, cardiovascular effects. |
| Adjuvants (e.g., Gabapentin, Pregabalin) | Modulate neurotransmission, reducing neuropathic pain and enhancing the effects of other analgesics. | Drowsiness, dizziness, swelling, and in rare cases, allergic reactions. |
Developing a Personalized Pain Management Plan, Types of surgery pain
Developing a personalized pain management plan involves a collaborative effort between the surgeon, anesthesiologist, and the patient. The plan should consider the patient’s specific needs, including their medical history, surgical procedure, and pain tolerance. Individualized pain management plans take into account factors like the type of surgery, the patient’s overall health, and their previous experiences with pain management.
This personalized approach ensures that the most appropriate and effective pain relief strategies are implemented.
Patient Experience and Pain Perception

The journey through surgery is not just about the physical procedure; it’s deeply intertwined with the patient’s emotional and psychological response. Understanding how individuals perceive and react to pain is crucial for effective pain management. This section delves into the multifaceted factors influencing surgical pain, from pre-operative anxiety to the role of patient education and pain assessment tools. It aims to equip both patients and healthcare providers with a deeper understanding of the complexities of surgical pain.Individual responses to surgical pain are highly variable.
Several factors contribute to this variability, including pre-existing pain conditions, genetics, and the patient’s overall health. The patient’s psychological state, expectations, and coping mechanisms significantly influence their perception of pain.
Factors Influencing Individual Patient Responses
Variability in surgical pain response stems from a combination of biological and psychological factors. Pre-existing pain conditions, chronic illnesses, and even individual genetic predispositions can influence how a patient experiences pain. Physiological factors, such as the patient’s overall health status and the specific surgical procedure, also play a significant role. The individual’s emotional state, including anxiety and fear, profoundly affects their pain perception.
Role of Psychological Factors in Pain Perception
Anxiety and fear are potent factors in escalating pain perception. A patient’s psychological state can significantly influence their experience of surgical pain. For example, high levels of anxiety can lead to a heightened awareness of pain signals, making the experience more intense. Similarly, fear of the unknown or the potential complications of the procedure can exacerbate pain perception.
A patient’s coping mechanisms, their ability to manage stress, and their previous experiences with pain also play a crucial role.
Impact of Pre-operative Education
Thorough pre-operative education plays a vital role in empowering patients to manage surgical pain effectively. This education should encompass not only the surgical procedure itself but also pain management strategies, expectations of post-operative discomfort, and available resources. Providing clear and concise information helps patients feel more prepared and in control, reducing anxiety and potentially decreasing the intensity of pain perception.
Pain Scales Used to Assess Surgical Pain
Various pain scales are used to objectively quantify surgical pain. The visual analog scale (VAS), a simple tool, involves a straight line with descriptors at each end (e.g., “no pain” and “worst pain imaginable”). The patient marks the point on the line that best reflects their pain intensity. Another commonly used scale is the numerical rating scale (NRS), where patients rate their pain on a scale of 0 to 10.
These scales provide a standardized way to assess pain, enabling healthcare professionals to track pain levels over time and tailor pain management strategies accordingly. The Wong-Baker FACES pain rating scale, particularly useful for children and those with communication difficulties, uses faces to represent different levels of pain.
Questionnaire to Evaluate Patient Pain Experience
Evaluating patient pain experience after surgery requires a structured approach. The following questionnaire aims to gather comprehensive information about the patient’s pain perception.
| Question | Possible Responses |
|---|---|
| Describe your pain (e.g., sharp, dull, throbbing). | Options: sharp, dull, throbbing, aching, etc. |
| Rate your pain intensity on a scale of 0 to 10. | Numerical values from 0 to 10. |
| Where is the pain located? | Specific anatomical locations. |
| How does the pain affect your daily activities? | Options: interferes significantly, moderately, minimally, not at all. |
| How would you rate your overall pain experience (from 1-5)? | Numerical values from 1 to 5 (e.g., 1=Excellent, 5=Poor). |
| Are there any other symptoms you’re experiencing? | Open-ended response. |
Pain Assessment and Monitoring
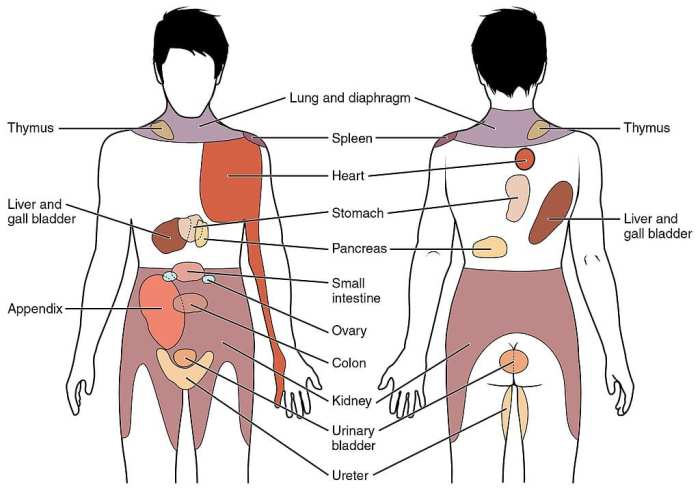
Surgical pain management hinges on accurate assessment and diligent monitoring. Effective pain control relies heavily on knowing the patient’s experience, which necessitates a systematic approach to evaluating and tracking pain levels. This allows for timely adjustments to treatment plans, optimizing patient comfort and recovery.Pain assessment isn’t a one-size-fits-all process. Different individuals react to pain differently, and the type of surgery significantly impacts the experience.
Surgery pain comes in various forms, from sharp, stabbing sensations to a dull, throbbing ache. Understanding these different types can help patients and doctors better manage recovery. Interestingly, similar diagnostic methods used to determine the presence and severity of lead poisoning, such as blood tests and X-rays, can also be crucial in pinpointing the specific type and intensity of surgical pain.
For more on how lead poisoning is diagnosed, check out this helpful resource: how lead poisoning is diagnosed. Ultimately, knowing the different kinds of post-operative pain is key to a smooth recovery.
A tailored approach is crucial to ensuring accurate pain measurement and appropriate interventions.
Validated Pain Scales
Various validated pain scales are essential tools in surgical settings. These standardized instruments provide a consistent method for assessing pain intensity, enabling objective comparisons and facilitating communication between healthcare professionals and patients. Using a consistent scale across patients allows for better data analysis and treatment evaluation.
- The Numerical Rating Scale (NRS): This is a simple, widely used scale where patients rate their pain on a scale of 0 to 10, with 0 representing no pain and 10 representing the worst imaginable pain. It’s easily understood by patients of various backgrounds and literacy levels.
- The Visual Analog Scale (VAS): This scale presents a horizontal line, and patients mark the point that best represents their pain level. The length of the line represents the range of pain intensity. It allows for a more precise assessment of pain intensity than the NRS.
- The Wong-Baker FACES pain rating scale: This scale utilizes faces to represent different levels of pain. It’s particularly useful for children and patients who have difficulty expressing their pain verbally.
Postoperative Pain Monitoring
Monitoring pain levels throughout the postoperative period is crucial to ensure optimal recovery. This involves regular assessments and recording of pain scores, alongside observation of other vital signs and patient behaviors.
- Regular assessments: Pain should be assessed at predetermined intervals (e.g., every 2-4 hours) after surgery, and the frequency adjusted as needed based on the patient’s response and the nature of the procedure.
- Documentation: Accurate documentation of pain scores and any other relevant observations (such as changes in behavior, vital signs, or medication administration) is essential for tracking trends and identifying potential complications.
- Patient reports: Active listening to the patient’s subjective experiences and reports is equally important. Patients’ verbalizations about their pain should be recorded and considered along with objective pain measurements.
Pain Assessment and Management Flowchart
A standardized flowchart facilitates a systematic approach to pain assessment and management in a surgical setting. This approach helps ensure consistency and optimizes patient care.
| Step | Action |
|---|---|
| 1 | Preoperative Assessment: Evaluate patient history, pain tolerance, and potential risk factors. Obtain informed consent for pain management. |
| 2 | Postoperative Pain Assessment: Immediately after surgery, assess pain using a validated scale. |
| 3 | Regular Monitoring: Continuously monitor pain levels at defined intervals. Record pain scores, vital signs, and any observed changes in behavior. |
| 4 | Pain Management Adjustment: Adjust pain medication regimen as needed based on the patient’s response. |
| 5 | Post-discharge Instructions: Provide clear instructions on pain management, follow-up appointments, and potential warning signs to the patient and their family. |
Special Considerations in Different Patient Groups
Surgical pain management requires careful consideration of individual patient characteristics. Age, pre-existing conditions, and even cultural factors can significantly impact a patient’s experience and response to pain relief strategies. Understanding these nuances is crucial for tailoring treatment plans to optimize outcomes and patient well-being.Pain management strategies need to be adapted to different patient groups. Elderly patients, children, and those with pre-existing conditions may experience surgery-related pain differently and require adjusted approaches.
Recognizing these variations allows healthcare providers to deliver more effective and personalized care.
Pain Management Strategies for the Elderly
Elderly patients often exhibit unique physiological responses to surgery and pain. Decreased metabolism, altered drug absorption, and potential cognitive impairment can complicate pain management. Tailoring analgesic regimens to accommodate these factors is essential. For example, slower release medications might be more suitable than rapid-onset ones, to avoid potential adverse effects related to drug accumulation.
Pain Management Strategies for Children
Managing pain in children presents specific challenges. Children’s pain perception and communication differ significantly from adults. Non-pharmacological methods, such as distraction and relaxation techniques, play a crucial role in pediatric pain management. Pharmacological approaches should be carefully selected and administered based on the child’s age, weight, and specific condition. Careful monitoring and adjustment of medication dosages are paramount.
Pain Management Strategies for Patients with Pre-existing Conditions
Patients with pre-existing conditions, such as cardiovascular disease or respiratory issues, require individualized pain management strategies. These conditions can affect the patient’s ability to tolerate certain medications or anesthetic agents. Careful evaluation of potential drug interactions and close monitoring of vital signs during and after surgery are essential. For instance, patients with kidney disease may require adjusted dosages of certain pain medications.
Pain Management in Minimally Invasive Surgery
Minimally invasive surgery (MIS) often results in less acute postoperative pain compared to traditional open procedures. However, the unique characteristics of MIS, such as the use of specialized instruments and smaller incisions, can lead to specific pain patterns. Patients undergoing MIS may experience localized discomfort or soreness around the incision site. Postoperative pain management in MIS often relies on targeted analgesics and regional anesthetic techniques.
Patient-Specific Considerations for Surgical Pain Management
Pain tolerance levels vary significantly among individuals. Some patients may require higher doses of analgesics to achieve adequate pain relief. Conversely, others may experience adverse effects from even low doses. Cultural influences also play a role in pain perception and management preferences. For example, some cultures may emphasize the importance of stoicism, which could affect how patients express their pain.
Open communication with patients, understanding their cultural background, and actively involving them in their pain management plan are crucial.
Comparison of Pain Management Strategies
Different pain management strategies exhibit varying degrees of effectiveness in different patient groups. For instance, while non-pharmacological methods like guided imagery may be effective for some elderly patients, others might require stronger pharmacological interventions. Factors like the surgical procedure, the patient’s overall health, and their pain tolerance must be considered when choosing the most appropriate strategy. Furthermore, the potential side effects and cost-effectiveness of each method should be evaluated in relation to the individual patient.
A comprehensive assessment is vital to tailor pain management for optimal results.
Future Directions in Surgical Pain Management: Types Of Surgery Pain
Surgical pain management is constantly evolving, driven by advancements in technology and a deeper understanding of pain mechanisms. The quest for more effective, less invasive, and patient-centered approaches is paramount. This evolution promises to significantly improve the patient experience and reduce the long-term impact of surgical procedures.The future of surgical pain management is focused on personalized strategies, leveraging individual patient characteristics and pain responses to tailor treatment plans.
This shift recognizes that “one size fits all” approaches are insufficient, and instead, anticipates the need for precise and targeted interventions.
Emerging Trends and Technologies
The field is witnessing a surge in innovative technologies, including advanced pain assessment tools and novel drug delivery systems. These advancements aim to improve pain management efficacy while minimizing side effects. Examples include real-time monitoring of pain signals, enabling prompt and precise interventions, and targeted drug delivery systems that release medications at the site of pain, maximizing efficacy and reducing systemic side effects.
Advancements in Pain Assessment and Treatment
Pain assessment methodologies are progressing to incorporate more objective measures. This includes the use of physiological markers, such as heart rate variability and skin conductance, to provide a more comprehensive picture of pain intensity and response to treatment. Furthermore, advancements in imaging techniques are allowing for better visualization of pain pathways and their modulation, leading to more accurate and personalized pain management strategies.
Future Research Areas
Several research areas hold significant promise for improving surgical pain management. One key area is exploring the role of the gut microbiome in postoperative pain. Another area focuses on identifying specific genetic markers that predict an individual’s susceptibility to postoperative pain, allowing for personalized preventative measures. This understanding would enable proactive interventions, potentially preventing chronic pain issues.
Patient-Reported Outcomes in Evaluating Effectiveness
Patient-reported outcomes (PROs) are increasingly recognized as essential for evaluating the effectiveness of pain management strategies. PROs provide a direct assessment of the patient’s experience, including pain intensity, interference with daily activities, and overall quality of life. By integrating patient perspectives, researchers can gain a holistic view of the impact of pain management interventions and tailor treatments to individual needs.
Examples of PROs include visual analog scales (VAS), numeric rating scales (NRS), and questionnaires that evaluate the patient’s emotional well-being and functional capacity. This patient-centric approach is crucial for optimizing treatment outcomes and improving the quality of life for surgical patients.
Conclusion
In conclusion, managing surgical pain is a multifaceted process, demanding a personalized approach. From pharmacological interventions to non-pharmacological techniques, and patient-specific considerations, effective pain management hinges on a comprehensive understanding of the diverse types of pain, their underlying mechanisms, and individual patient experiences. The future of surgical pain management promises exciting advancements, emphasizing the crucial role of ongoing research and patient-centered care.