What are platelet function disorders? They’re conditions affecting the tiny blood cells crucial for clotting. Understanding these disorders involves exploring the intricate role platelets play in normal blood clotting, the various types of these disorders, their prevalence, and the often-complex symptoms and diagnosis processes. We’ll also delve into the causes, treatment options, potential complications, and preventative measures.
Platelets, often overlooked, are essential components of our blood’s ability to stop bleeding. Disruptions in their function can lead to a range of problems, impacting everything from minor cuts to major surgical procedures. This exploration will cover the entire spectrum of platelet function disorders, from the initial signs and symptoms to the long-term implications and the treatments available.
Introduction to Platelet Function Disorders
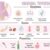
Platelet function disorders are conditions that affect the ability of platelets, also known as thrombocytes, to perform their crucial role in blood clotting. These disorders can range from mild to severe, impacting the individual’s overall health and necessitating careful management. Understanding the intricacies of platelet function and the diverse types of disorders is vital for diagnosis and appropriate treatment.Platelets are small, irregular-shaped cell fragments that circulate in the bloodstream.
They play a critical role in hemostasis, the process of stopping bleeding. When a blood vessel is injured, platelets adhere to the damaged site and aggregate, forming a plug that temporarily seals the break. This process, along with the coagulation cascade, is essential for preventing excessive blood loss. Disruptions in any step of this process can lead to bleeding tendencies.
Platelet Function Disorder Types
Platelet function disorders can be broadly categorized into two main types: qualitative and quantitative. Qualitative disorders involve a problem with the platelet’s ability to function normally, despite being present in adequate numbers. Quantitative disorders, on the other hand, relate to a reduced number of platelets in the blood. These categories encompass a wide spectrum of disorders, each with its own set of symptoms and underlying causes.
Prevalence and Impact
The prevalence of platelet function disorders varies significantly depending on the specific disorder. While some are relatively rare, others occur more frequently. The impact of these disorders can range from mild bleeding episodes to life-threatening complications, depending on the severity and the individual’s overall health. For example, a mild disorder might manifest as frequent nosebleeds or easy bruising, whereas a severe disorder could lead to significant internal bleeding or even life-threatening hemorrhages.
The long-term impact can include difficulties in daily activities and increased risk of complications during surgical procedures.
Detailed Overview of Platelet Function Disorders
| Disorder Type | Symptoms | Common Causes |
|---|---|---|
| Qualitative Disorders | Easy bruising, prolonged bleeding after minor cuts or injuries, nosebleeds, heavy menstrual bleeding, bleeding gums, internal bleeding, petechiae (tiny red spots on skin), purpura (larger purple patches on skin), prolonged bleeding after dental procedures. | Genetic defects in platelet proteins, medications (e.g., aspirin, NSAIDs), certain medical conditions (e.g., uremia, some cancers), acquired immune disorders affecting platelets. |
| Quantitative Disorders | Easy bruising, prolonged bleeding, spontaneous bleeding, petechiae, purpura, nosebleeds, bleeding gums, internal bleeding, heavy menstrual bleeding, bleeding after dental procedures. | Inherited bone marrow disorders, autoimmune diseases, infections, certain medications, and exposure to certain chemicals. |
Symptoms and Diagnosis: What Are Platelet Function Disorders
Platelet function disorders are a diverse group of conditions, each presenting a unique array of symptoms and challenges in diagnosis. Understanding the common signs and the various diagnostic methods is crucial for timely and accurate intervention. A detailed evaluation, incorporating patient history, physical examination findings, and specific laboratory tests, is essential to pinpoint the specific disorder and develop an effective treatment plan.Platelet function disorders manifest in a range of ways, often mimicking other bleeding conditions.
The severity of symptoms can vary widely, depending on the specific type and degree of platelet dysfunction. Recognizing these symptoms is the first step toward proper diagnosis and treatment.
Common Symptoms
Recognizing the spectrum of symptoms associated with platelet function disorders is vital for early diagnosis. These symptoms can range from mild to severe and often include:
- Frequent or prolonged bleeding from minor cuts or injuries.
- Easy bruising (purpura) that appears spontaneously or after minor trauma.
- Bleeding into joints (hemarthrosis), causing pain and swelling.
- Bleeding into the skin (petechiae), appearing as tiny red or purple spots.
- Nosebleeds (epistaxis) that are frequent or severe.
- Bleeding from the gums (gingival bleeding).
- Heavy menstrual bleeding (menorrhagia) in women.
- Gastrointestinal bleeding, manifesting as blood in the stool (melena).
The frequency and severity of these symptoms can provide valuable clues to the underlying platelet dysfunction.
Diagnostic Methods
Diagnosing platelet function disorders requires a multi-faceted approach, combining patient history, physical examination, and specific laboratory tests. These methods provide a comprehensive picture of the patient’s condition, enabling accurate diagnosis and subsequent treatment.
Laboratory Tests
A panel of laboratory tests is crucial in evaluating platelet function. These tests assess various aspects of platelet function, providing valuable data for diagnosis.
- Complete Blood Count (CBC): This provides information on platelet count, size, and morphology. A low platelet count (thrombocytopenia) is not always present, but may indicate a more serious underlying condition.
- Platelet Function Assays: These tests directly evaluate the ability of platelets to aggregate (stick together) and form clots. Different assays measure various aspects of platelet function, such as the response to agonists (substances that stimulate platelet activation).
Examples include PFA-100 (Platelet Function Analyzer) and bleeding time tests.
- Coagulation Tests: While not specific to platelet function disorders, these tests (e.g., prothrombin time (PT) and activated partial thromboplastin time (aPTT)) help differentiate platelet disorders from other bleeding disorders involving clotting factors.
Physical Examination
A thorough physical examination plays a vital role in the diagnostic process. It complements laboratory findings by assessing the presence and extent of bleeding manifestations.
- Skin Inspection: Careful examination of the skin for petechiae, purpura, and ecchymoses (bruises) can reveal the extent of bleeding tendencies. The location and size of the lesions can offer clues to the underlying cause.
- Assessment of Bleeding Sites: Evaluation of bleeding from the gums, nose, or other sites can provide crucial information regarding the severity and frequency of bleeding episodes. Careful questioning about bleeding history can help determine the duration and nature of these episodes.
- Joint Evaluation: Examination of joints for swelling and pain can indicate bleeding into the joint spaces, which is a hallmark symptom of certain platelet function disorders.
Comparison of Diagnostic Tests
| Test | Accuracy | Limitations |
|---|---|---|
| Platelet Function Analyzer (PFA-100) | Generally accurate in identifying platelet dysfunction. | May not detect all types of platelet function defects and can be affected by other factors. |
| Bleeding Time | Provides a general assessment of platelet function. | Less sensitive and specific than newer tests and affected by other factors like vascular integrity. |
| Platelet Aggregation Tests | Highly specific for evaluating platelet aggregation. | Complex and require specialized expertise; may not be readily available in all settings. |
This table provides a general comparison; specific accuracy and limitations may vary depending on the laboratory and the specific test used. Consulting with a hematologist is crucial for accurate interpretation and tailored management strategies.
Causes and Risk Factors
Platelet function disorders can stem from a variety of factors, both intrinsic and extrinsic. Understanding these causes is crucial for proper diagnosis and treatment. Genetic predispositions play a significant role, but environmental influences and lifestyle choices can also contribute to the development of these disorders.Genetic variations and acquired conditions can disrupt the delicate balance of platelet function, leading to either a deficiency in their production or a problem with their ability to adhere, aggregate, or release important substances.
The consequences of these disruptions can range from mild bleeding tendencies to life-threatening complications.
Genetic Causes
Genetic mutations are a primary cause of some platelet function disorders. These mutations can affect the genes responsible for producing or regulating proteins involved in platelet function. For instance, defects in genes coding for glycoproteins, which are essential components of the platelet surface, can lead to impaired platelet adhesion and aggregation.
Acquired Causes
Acquired platelet function disorders are less common than genetic forms, but they are equally important to recognize. These disorders develop as a result of external factors rather than inherited genetic defects. Medications, such as aspirin or other nonsteroidal anti-inflammatory drugs (NSAIDs), can interfere with platelet function, leading to increased bleeding risk. Certain medical conditions, such as liver disease or kidney disease, can also impact platelet function.
Furthermore, infections, especially some viral infections, can sometimes affect platelet function, although this is less frequently a direct cause.
Risk Factors
Several factors can increase the likelihood of developing a platelet function disorder. Identifying these risk factors can aid in preventative measures.
| Category | Potential Risk Factors |
|---|---|
| Medications | Aspirin, NSAIDs, anticoagulants |
| Medical Conditions | Liver disease, kidney disease, cancer, autoimmune disorders |
| Lifestyle | Excessive alcohol consumption, smoking, poor diet |
| Genetics | Family history of bleeding disorders |
Lifestyle Influences
Lifestyle choices can significantly impact platelet function. A diet deficient in essential nutrients, such as vitamin K, can compromise platelet function. Excessive alcohol consumption is linked to impaired platelet production and function. Smoking also negatively affects platelet function, contributing to increased risk of bleeding.
Regular exercise and a balanced diet, rich in fruits, vegetables, and whole grains, can promote healthy platelet function. Conversely, a sedentary lifestyle and poor dietary habits can increase the risk of developing platelet function disorders.
Treatment Options and Management
Platelet function disorders, while often manageable, require careful monitoring and tailored treatment plans. Effective management hinges on understanding the specific type of disorder and its severity, allowing for the most appropriate and effective intervention. This section will explore the various treatment options available, from medications to lifestyle adjustments, and emphasize the critical role of ongoing monitoring.Treatment for platelet function disorders focuses on addressing the underlying cause if possible, and managing the symptoms to prevent complications.
Platelet function disorders are conditions where your blood’s platelets don’t work properly, impacting blood clotting. Sometimes, these issues can be linked to other health problems, like the potential causes of sudden hearing loss, as explored in detail in this article on cause of hearing loss sudden deafness. Understanding these connections is crucial for proper diagnosis and treatment of platelet function disorders.
This often involves a combination of approaches, aiming to increase platelet function or prevent bleeding episodes.
Medication Options
Medications play a crucial role in managing platelet function disorders. They can be broadly categorized into those that stimulate platelet production, and those that help control bleeding episodes.
- Platelet Aggregation Inhibitors: Some medications, such as aspirin, can reduce platelet aggregation, making them less likely to clump together and form blood clots. This can be beneficial in certain cases, but it’s important to understand that prolonged use of such drugs can increase the risk of bleeding. For instance, in patients with a history of bleeding disorders, the risk of uncontrolled bleeding must be carefully weighed against the benefits of using these medications.
- Desmopressin: This medication is sometimes used to increase the body’s production of von Willebrand factor, a protein that helps platelets stick together. It can be particularly effective in some types of von Willebrand disease. Its efficacy depends on the specific type and severity of the disorder.
- Tranexamic Acid: This medication helps to reduce the breakdown of blood clots and is often effective in managing bleeding episodes. It works by interfering with the enzymes that break down clots. Its use is particularly important in situations where there is significant bleeding, and its effectiveness can vary depending on the specific type and severity of the disorder.
- Other Medications: Depending on the specific platelet function disorder, other medications may be prescribed, such as specific clotting factors, or antifibrinolytic agents. The choice of medication and dosage will be tailored to the individual patient’s needs and the severity of the condition.
Monitoring and Long-Term Management
Regular monitoring is essential for managing platelet function disorders effectively. This includes frequent blood tests to assess platelet counts and function, and careful tracking of bleeding episodes. Early intervention is key in preventing complications.
- Monitoring for Bleeding Episodes: Regular check-ups are crucial for detecting and addressing any bleeding issues promptly. The frequency of monitoring depends on the severity and type of the disorder. Patients with a history of severe bleeding episodes may require more frequent monitoring than those with milder symptoms.
- Lifestyle Adjustments: Lifestyle modifications can play a supportive role. Avoiding activities that could increase the risk of injury, such as contact sports, is often advised. Similarly, careful attention to diet and avoiding medications that can interfere with platelet function are important lifestyle factors to consider.
- Proactive Management: A personalized management strategy is crucial. This includes understanding the individual’s risk factors and potential triggers for bleeding episodes, which can be tailored to reduce the likelihood of severe bleeding episodes.
Potential Complications and Management
Complications of platelet function disorders can range from minor bleeding episodes to more serious issues, like internal bleeding or organ damage. Early diagnosis and treatment are crucial to minimizing the risk of complications.
- Severe Bleeding: Significant bleeding, especially in joints or internal organs, can be life-threatening. Prompt medical intervention is essential in such cases. Emergency care protocols and the availability of blood transfusions are crucial in managing severe bleeding episodes.
- Delayed Diagnosis: Delayed diagnosis can lead to more severe complications. Symptoms such as prolonged bleeding after minor injuries, frequent nosebleeds, or heavy menstrual bleeding should be taken seriously. Early diagnosis allows for prompt intervention and prevents potentially serious consequences.
- Chronic Issues: Some patients may experience chronic bleeding issues, necessitating ongoing management strategies to minimize the risk of complications. Continuous monitoring and careful adjustment of treatment plans can significantly improve the patient’s quality of life.
Treatment Effectiveness Table
| Treatment Option | Mechanism of Action | Effectiveness in Different Cases |
|---|---|---|
| Platelet Aggregation Inhibitors | Reduces platelet clumping | Effective for some disorders but may increase bleeding risk |
| Desmopressin | Increases von Willebrand factor | Effective in von Willebrand disease, less effective in other disorders |
| Tranexamic Acid | Reduces clot breakdown | Effective in managing bleeding episodes, particularly in cases of heavy bleeding |
| Other Medications | Addresses specific underlying issues | Effectiveness varies depending on the specific medication and disorder |
Complications and Long-Term Effects
Platelet function disorders, while often manageable, can lead to a range of complications and long-term effects impacting patients’ overall health and quality of life. Understanding these potential issues is crucial for proactive management and appropriate support. Early recognition and intervention can significantly reduce the severity and impact of these complications.These disorders can create various challenges, from frequent bleeding episodes to more serious systemic issues.
Platelet function disorders can be tricky, impacting how your blood clots. Understanding these conditions is key, especially when considering hormonal contraception after age 40, as certain medications can influence platelet function. For more detailed information on the nuances of hormonal contraception after age 40, check out this resource: hormonal contraception after age 40. Ultimately, it’s vital to discuss any concerns with your doctor about these disorders and their potential interactions with your current health regime.
The long-term consequences can vary depending on the specific disorder, its severity, and the individual’s response to treatment. This section delves into the potential complications and long-term effects, highlighting their impact on daily life and specific organ systems.
Potential Bleeding Complications
Bleeding complications are a hallmark of platelet function disorders. These range from minor bruising and nosebleeds to more severe and potentially life-threatening episodes. The frequency and severity of bleeding episodes can fluctuate, making accurate prediction and consistent management a significant challenge.
Platelet function disorders happen when your platelets don’t work properly, impacting blood clotting. This can lead to unusual bleeding, like easy bruising or heavy periods. Interestingly, similar to how specific exercises can strengthen muscles around a herniated disc, like the ones detailed in exercises for herniated disc , certain lifestyle choices and treatments can help manage platelet function disorders.
Ultimately, understanding these disorders and their potential solutions is key to overall health.
- Frequent nosebleeds (epistaxis): Recurring nosebleeds can be distressing and disrupt daily activities. They may necessitate frequent medical intervention and can impact a patient’s self-confidence.
- Easy bruising (purpura): Frequent bruising, often with minimal trauma, is a common symptom. This can lead to significant physical discomfort and, in severe cases, can cause pain and hinder mobility.
- Gastrointestinal bleeding: Bleeding within the gastrointestinal tract can cause significant blood loss, leading to anemia and potentially requiring hospitalization and blood transfusions. Symptoms can range from mild discomfort to severe pain and even shock.
- Intracranial bleeding: Bleeding within the brain (intracranial hemorrhage) is a potentially life-threatening complication. Symptoms may include headache, seizures, altered consciousness, and neurological deficits. Prompt medical attention is crucial.
Impact on Daily Life and Quality of Life
Platelet function disorders can significantly impact patients’ daily lives and quality of life. The unpredictability of bleeding episodes can create anxiety, limit participation in social activities, and restrict physical activities. Emotional well-being can be profoundly affected by the constant worry and fear of bleeding episodes.
- Social isolation: Fear of bleeding in public settings can lead to social withdrawal and isolation, impacting the patient’s social interactions and relationships.
- Limited physical activity: Concerns about potential bleeding episodes can restrict participation in sports, exercise, and other physical activities, hindering physical health and overall well-being.
- Financial burden: The cost of treatment, medications, and potential hospitalizations can place a significant financial burden on patients and their families.
- Psychological distress: The chronic nature of the disorder and the unpredictable bleeding episodes can cause anxiety, depression, and other psychological distress. Mental health support is often essential for patients.
Impact on Specific Organ Systems
Certain platelet function disorders can affect specific organ systems, leading to more complex complications. The extent of these impacts can vary depending on the particular disorder.
- Cardiovascular system: Some platelet disorders may increase the risk of cardiovascular complications, including thrombosis (blood clots). This is due to the inability of the body to form clots effectively.
- Gastrointestinal system: Bleeding in the gastrointestinal tract is a frequent complication. This can lead to chronic anemia and long-term health problems.
- Neurological system: Bleeding in the brain (intracranial hemorrhage) is a significant concern. This can result in long-term neurological impairments, such as paralysis, speech difficulties, and cognitive problems.
Potential Complications Table
| Potential Complications | Severity Level | Description |
|---|---|---|
| Frequent nosebleeds | Mild | Recurring episodes of epistaxis. |
| Easy bruising | Mild to Moderate | Bruising easily with minimal trauma. |
| Gastrointestinal bleeding | Moderate to Severe | Bleeding within the gastrointestinal tract. |
| Intracranial bleeding | Severe | Bleeding within the brain. |
| Cardiovascular complications | Moderate to Severe | Increased risk of thrombosis or other heart-related problems. |
Prevention and Prognosis
Platelet function disorders, while often not preventable, can be managed effectively with proactive measures. Understanding the prognosis, however, hinges on factors like the specific type of disorder, its severity, and the promptness of diagnosis and treatment. Prognosis also relies heavily on ongoing monitoring and adherence to management plans.Early intervention and consistent management are crucial in shaping the long-term outlook for individuals with platelet function disorders.
By understanding the factors influencing prognosis, individuals and healthcare professionals can work together to maximize positive outcomes.
Preventive Measures
Many platelet function disorders are not currently preventable. Lifestyle choices, while not directly preventing the underlying causes, can influence overall health and potentially reduce the risk of complications. A balanced diet, regular exercise, and avoiding smoking or excessive alcohol consumption contribute to a healthier body and can potentially lower the risk of certain secondary conditions.
- Maintaining a healthy lifestyle, including a balanced diet and regular exercise, can positively influence overall health, potentially reducing the risk of complications associated with some platelet disorders.
- Avoiding tobacco use and excessive alcohol consumption can help maintain overall health, and potentially reduce the risk of exacerbating existing conditions.
- Following recommended vaccinations and practicing good hygiene to prevent infections is important, as infections can trigger or worsen symptoms in some cases.
Prognosis Factors
The prognosis for platelet function disorders varies significantly based on several key factors. The type of disorder, its severity, and the presence of any co-existing conditions all play a role in determining the potential outcome. Prompt and accurate diagnosis is essential for effective treatment and improved prognosis. Early intervention allows for the initiation of targeted therapies, which can significantly impact long-term outcomes.
- Type of Disorder: Hereditary disorders often have a more established prognosis, allowing for earlier preventative measures and tailored management strategies. Acquired disorders, however, can have a more unpredictable prognosis, depending on the underlying cause.
- Severity of Disorder: Mild cases typically have a favorable prognosis, with effective management often leading to minimal impact on daily life. Severe cases, however, can pose significant challenges, requiring intensive medical intervention and ongoing monitoring.
- Promptness of Diagnosis and Treatment: Early diagnosis and initiation of appropriate treatment are critical to improving prognosis. Delayed diagnosis can lead to complications and potentially impact long-term outcomes.
Ongoing Monitoring and Management, What are platelet function disorders
Ongoing monitoring and management play a critical role in improving the prognosis for individuals with platelet function disorders. Regular check-ups, blood tests, and adherence to prescribed medications are crucial components of long-term management. Adjustments to treatment plans based on ongoing assessments are vital for maintaining optimal health and preventing complications. This proactive approach can significantly improve the quality of life for those affected.
- Regular Monitoring: Blood tests, physical examinations, and other assessments allow for ongoing monitoring of platelet function and the identification of potential complications.
- Adherence to Treatment: Following prescribed medications and treatment plans is essential for managing symptoms and preventing complications. This includes medication schedules and dietary restrictions.
- Management Adjustments: Healthcare providers adjust treatment plans based on the patient’s response to therapy and any emerging complications. This individualized approach is crucial for optimal outcomes.
Efficacy of Preventive Measures
While not all platelet function disorders are preventable, several lifestyle choices can contribute to overall health and potentially reduce the risk of complications. A well-balanced diet, regular exercise, and avoidance of smoking and excessive alcohol consumption can positively impact overall health.
| Preventive Measure | Efficacy |
|---|---|
| Healthy Diet | High |
| Regular Exercise | High |
| Smoking Cessation | High |
| Moderation in Alcohol Consumption | Moderate |
| Vaccinations and Hygiene | High |
Case Studies and Examples
Understanding platelet function disorders requires looking at real-world examples. These cases highlight the diverse presentations, diagnostic challenges, and the importance of personalized care in managing these conditions. Each individual experience shapes the course of treatment and long-term management.
Real-World Experiences of Individuals with Platelet Function Disorders
Platelet function disorders affect individuals in various ways. Some experience frequent or severe bleeding episodes, while others may have milder symptoms. These differences arise from the specific type of disorder, its severity, and the individual’s overall health. For example, a person with a mild disorder might experience only occasional nosebleeds or easy bruising, while someone with a severe disorder might face significant bleeding after minor injuries or even spontaneously.
This variability underscores the importance of individualized treatment plans.
Diagnostic and Treatment Processes in Case Studies
The diagnostic process for platelet function disorders often involves a series of tests. These tests may include complete blood counts (CBCs), bleeding time tests, platelet aggregation studies, and specialized genetic testing. The diagnostic process can be complex and time-consuming, as the symptoms can overlap with other conditions. Successful treatment relies on accurate diagnosis. Treatment options for platelet function disorders are diverse, ranging from medications to lifestyle adjustments.
For instance, some individuals may benefit from medications that help regulate platelet function, while others might require platelet transfusions during significant bleeding episodes.
Successful Treatment Outcomes for Specific Types of Platelet Function Disorders
Numerous case studies demonstrate successful treatment outcomes for specific types of platelet function disorders. For example, individuals with Glanzmann thrombasthenia, a genetic disorder affecting platelet function, have shown positive responses to treatments that support platelet production or enhance platelet function through medications. Another example is Bernard-Soulier syndrome, where a combination of medications and platelet transfusions can help manage symptoms and prevent severe bleeding complications.
Comparison of Case Studies
| Case Study | Type of Disorder | Symptoms | Diagnostic Process | Treatment Approach | Outcome |
|---|---|---|---|---|---|
| Case 1 | Glanzmann Thrombasthenia | Frequent nosebleeds, easy bruising, prolonged bleeding after minor cuts | CBC, bleeding time, platelet aggregation studies, genetic testing | Platelet transfusions, medications to stimulate platelet production | Significant improvement in bleeding episodes, reduced need for transfusions |
| Case 2 | Bernard-Soulier Syndrome | Large bruises, prolonged bleeding from wounds, significant bleeding after dental procedures | CBC, bleeding time, platelet aggregation studies, flow cytometry | Platelet transfusions, supportive care, avoidance of medications that affect platelet function | Controlled bleeding episodes, improved quality of life |
| Case 3 | Acquired Platelet Dysfunction | Bleeding after surgery, spontaneous bleeding | CBC, bleeding time, platelet aggregation studies, medication review | Identifying and removing the underlying cause (e.g., medication), platelet transfusions | Resolution of bleeding, prevention of further complications |
This table illustrates the key characteristics of different case studies, showcasing the diversity of platelet function disorders and their associated management strategies. Each case highlights the importance of a personalized approach to care, tailoring treatment to the specific needs of the individual.
Conclusive Thoughts
In summary, platelet function disorders present a multifaceted challenge to patients and healthcare providers. The intricate interplay of symptoms, causes, and treatment options requires a nuanced understanding. From the initial diagnosis to the long-term management, these disorders demand a personalized approach. This overview provides a comprehensive foundation for understanding these disorders, equipping readers with knowledge to navigate this complex medical landscape.