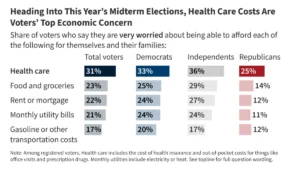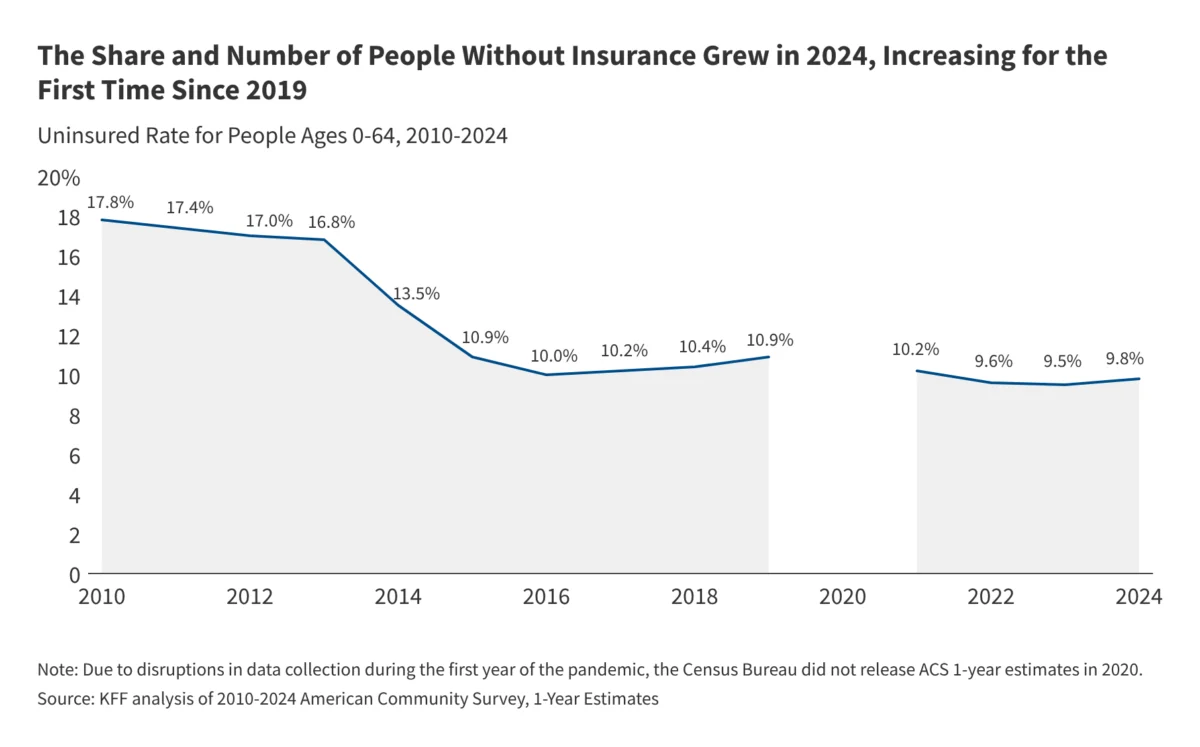
The United States health insurance landscape underwent a significant and sobering shift in 2024, marking the first time since 2019 that the national uninsured rate has seen a measurable increase. According to an extensive analysis of the American Community Survey (ACS) and supplemental health policy data, the number of individuals under the age of 65 without health insurance grew by more than 1.3 million people, bringing the total uninsured population in this demographic to 26.7 million. This shift represents an increase in the uninsured rate from 9.5% in 2023 to 9.8% in 2024, signaling an end to the steady coverage gains observed during the height of the COVID-19 pandemic.
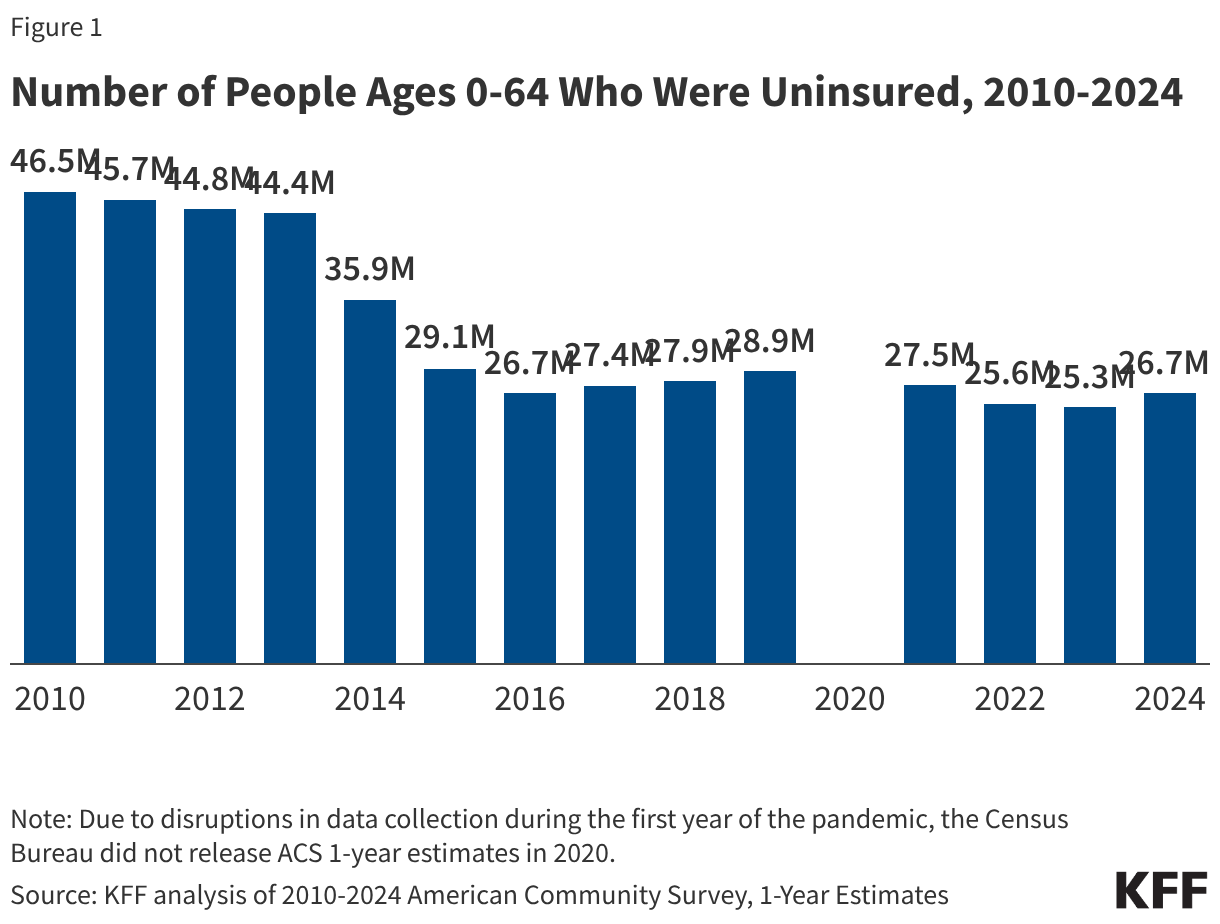
The reversal of these trends is largely attributed to a convergence of policy shifts, most notably the "unwinding" of Medicaid continuous enrollment protections, the persistent high cost of private insurance, and the continued refusal of several large states to expand Medicaid under the Affordable Care Act (ACA). As the nation moves further away from pandemic-era emergency measures, the structural complexities and fragmentation of the American healthcare system are once again leaving millions of low-income individuals and working families at risk of financial and medical catastrophe.
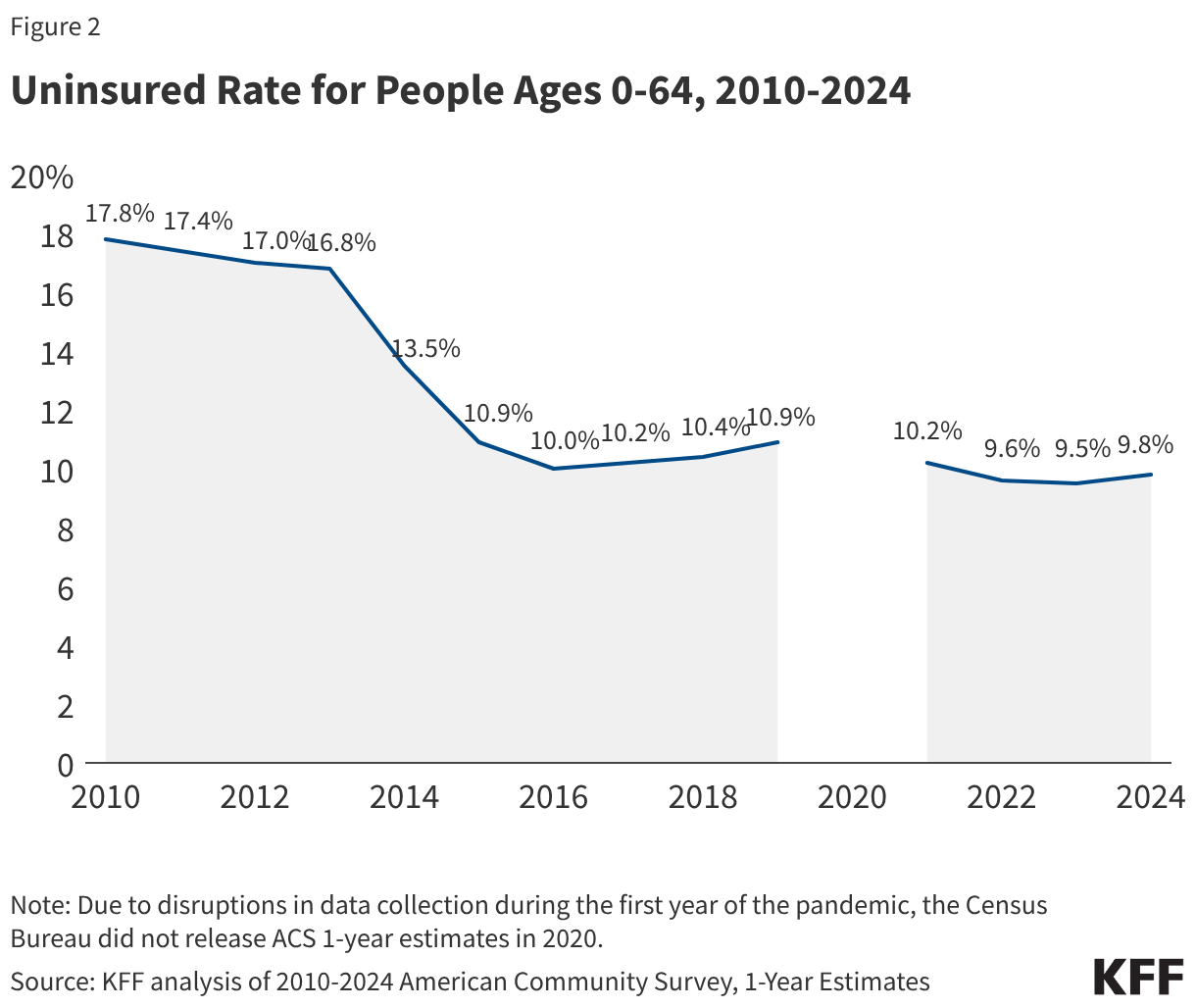
The Chronology of the Coverage Reversal: From Pandemic Protections to Unwinding
To understand the 2024 increase in the uninsured rate, one must look back to the legislative response to the COVID-19 pandemic. In 2020, the Families First Coronavirus Response Act (FFCRA) included a continuous enrollment provision that prohibited states from disenrolling individuals from Medicaid in exchange for enhanced federal funding. This provision acted as a vital safety net, ensuring that even as the economy fluctuated, millions of Americans maintained consistent access to healthcare.
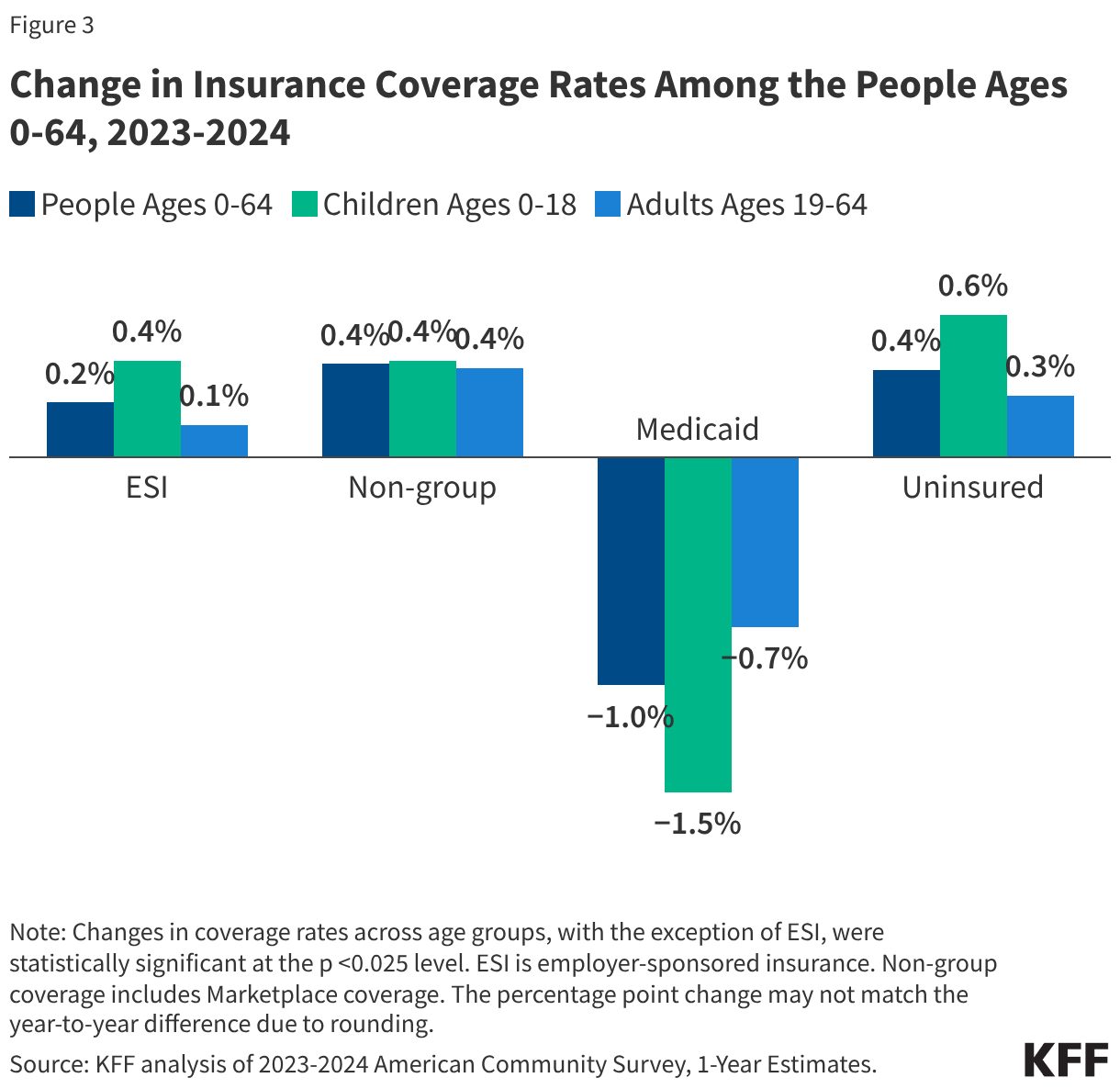
The timeline of the current coverage crisis began in earnest in April 2023, when federal law allowed states to resume routine Medicaid eligibility redeterminations—a process that became known as the "Medicaid unwinding." Throughout late 2023 and the entirety of 2024, states worked through massive backlogs of renewals. While many individuals were disenrolled because they were no longer eligible due to increases in income, millions of others lost coverage due to "procedural reasons," such as failing to receive a renewal form or facing bureaucratic hurdles in the application process.
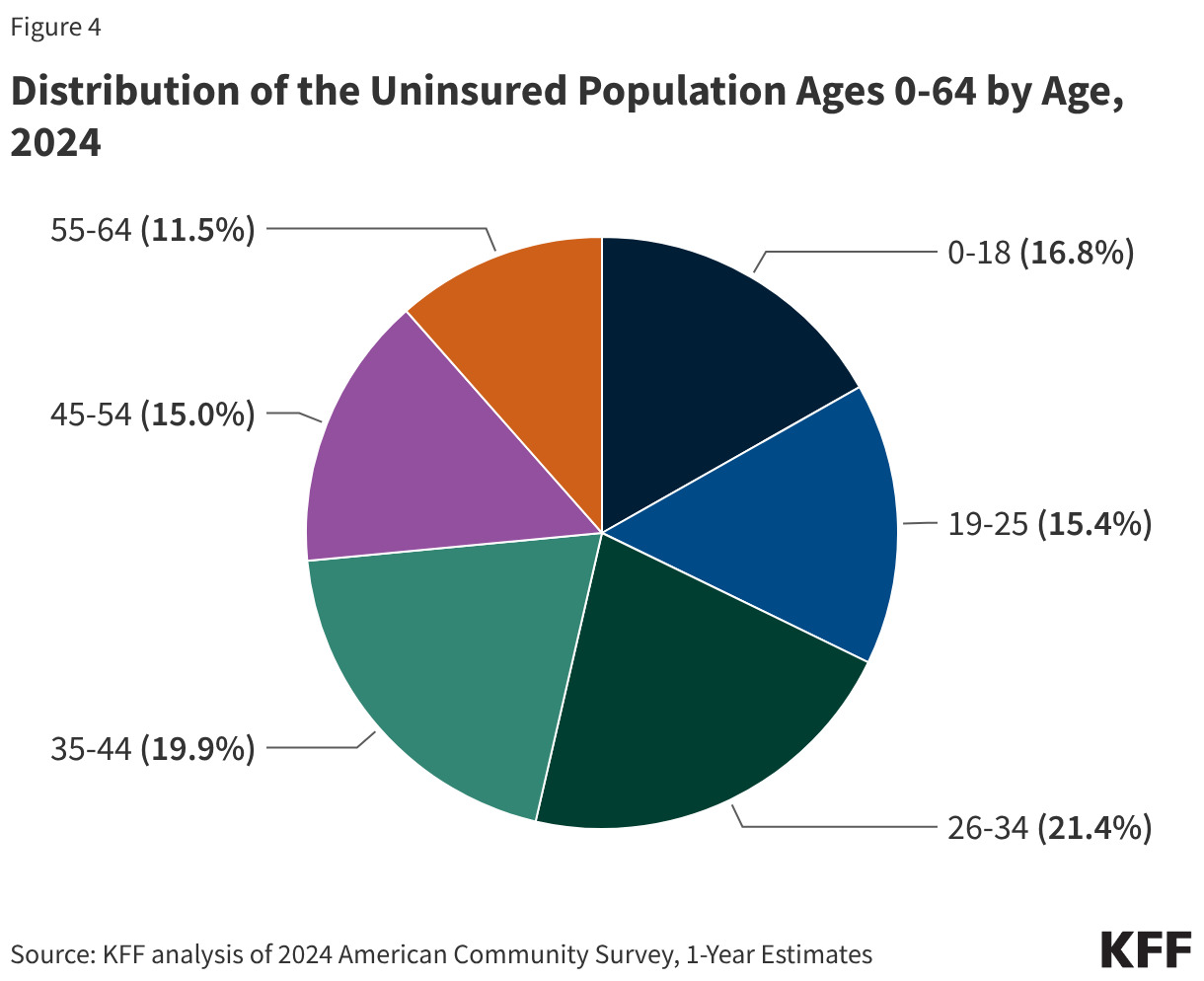
By the end of 2024, nearly all states had completed this unwinding process. While some individuals successfully transitioned to subsidized coverage through the ACA Marketplace—aided by enhanced premium tax credits—the transition was far from seamless. For many, the Marketplace options remained unaffordable despite subsidies, or the administrative complexity of switching plans resulted in a total loss of coverage.
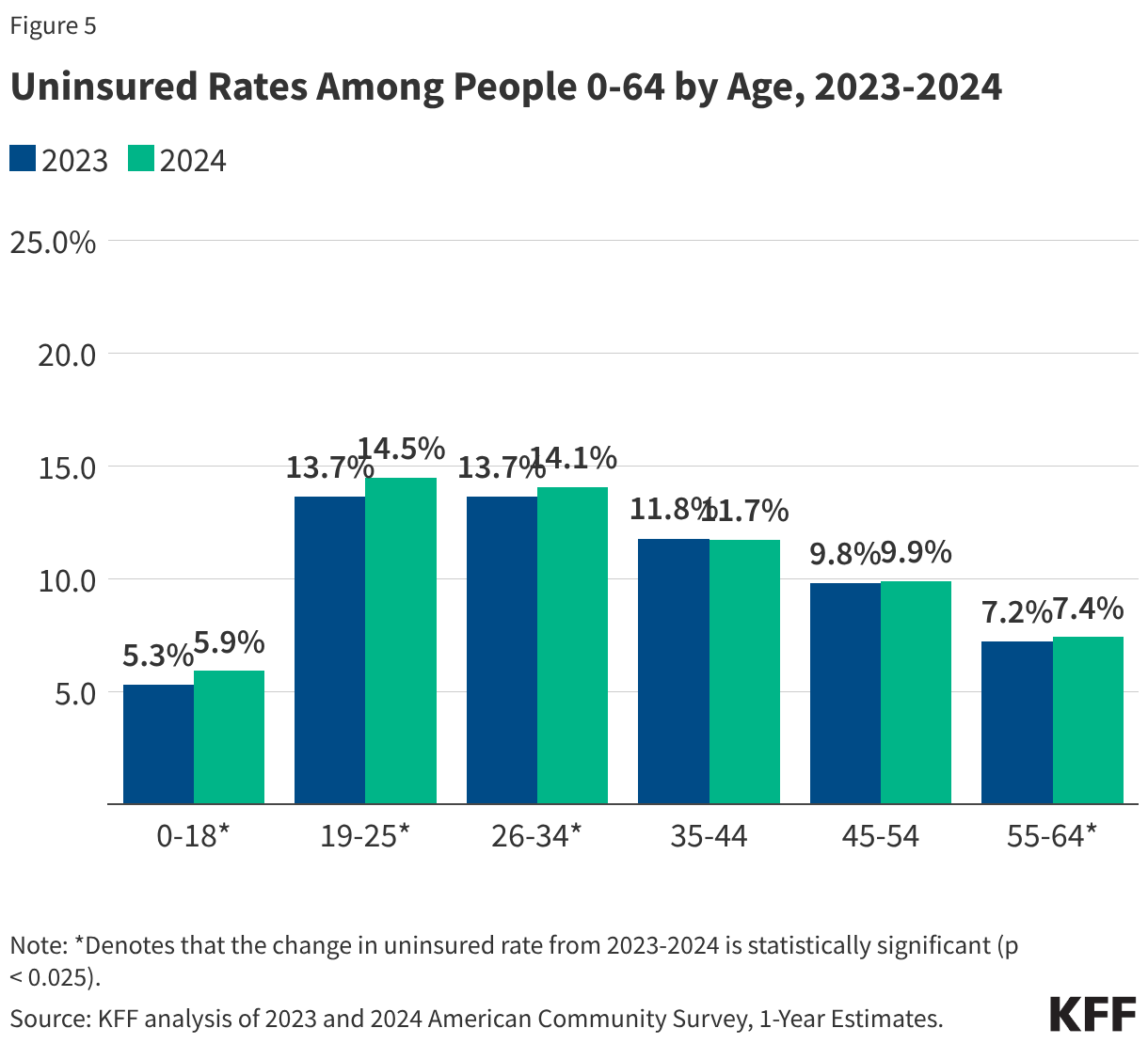
Demographic Analysis: Who is Falling Through the Cracks?
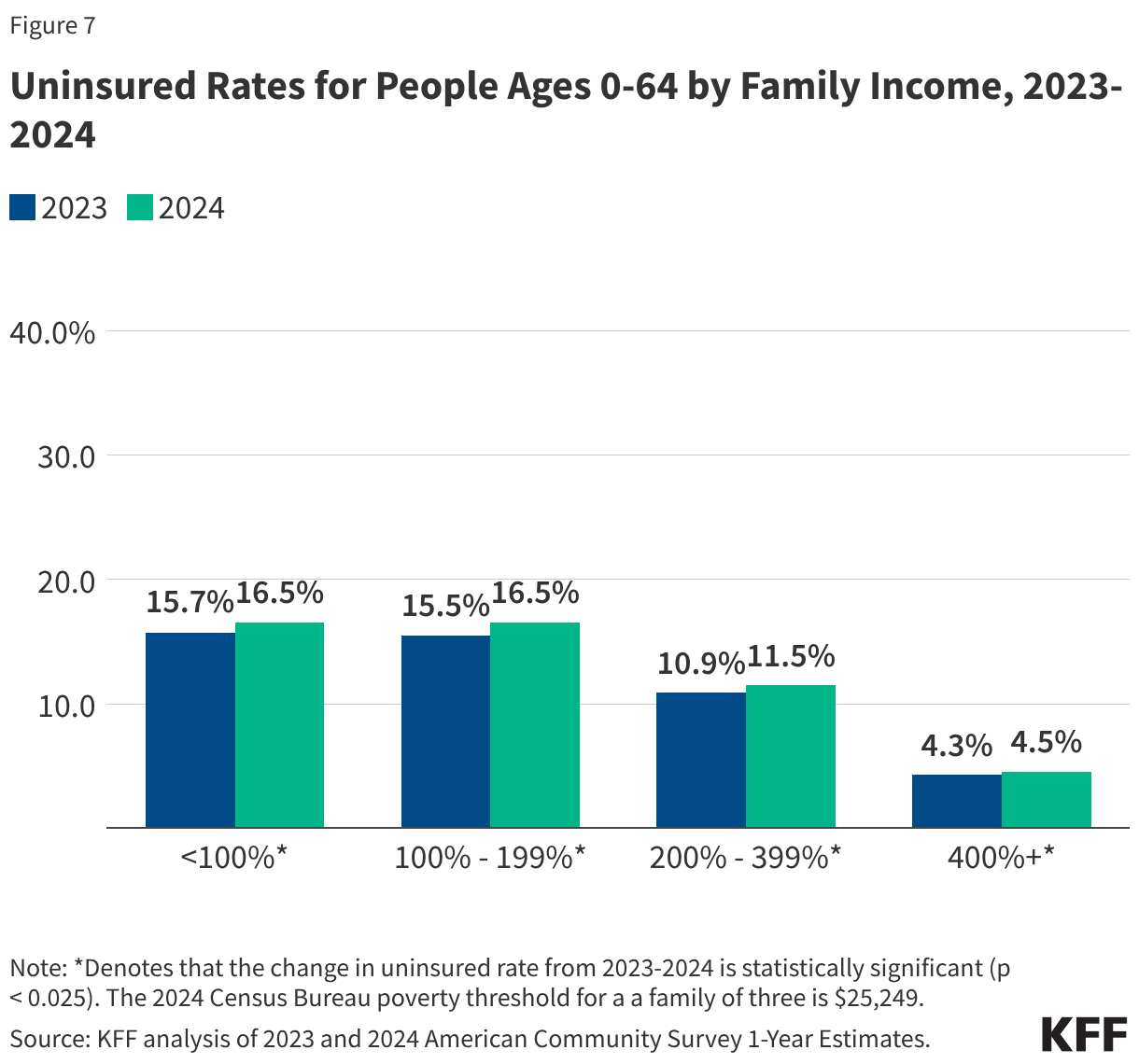
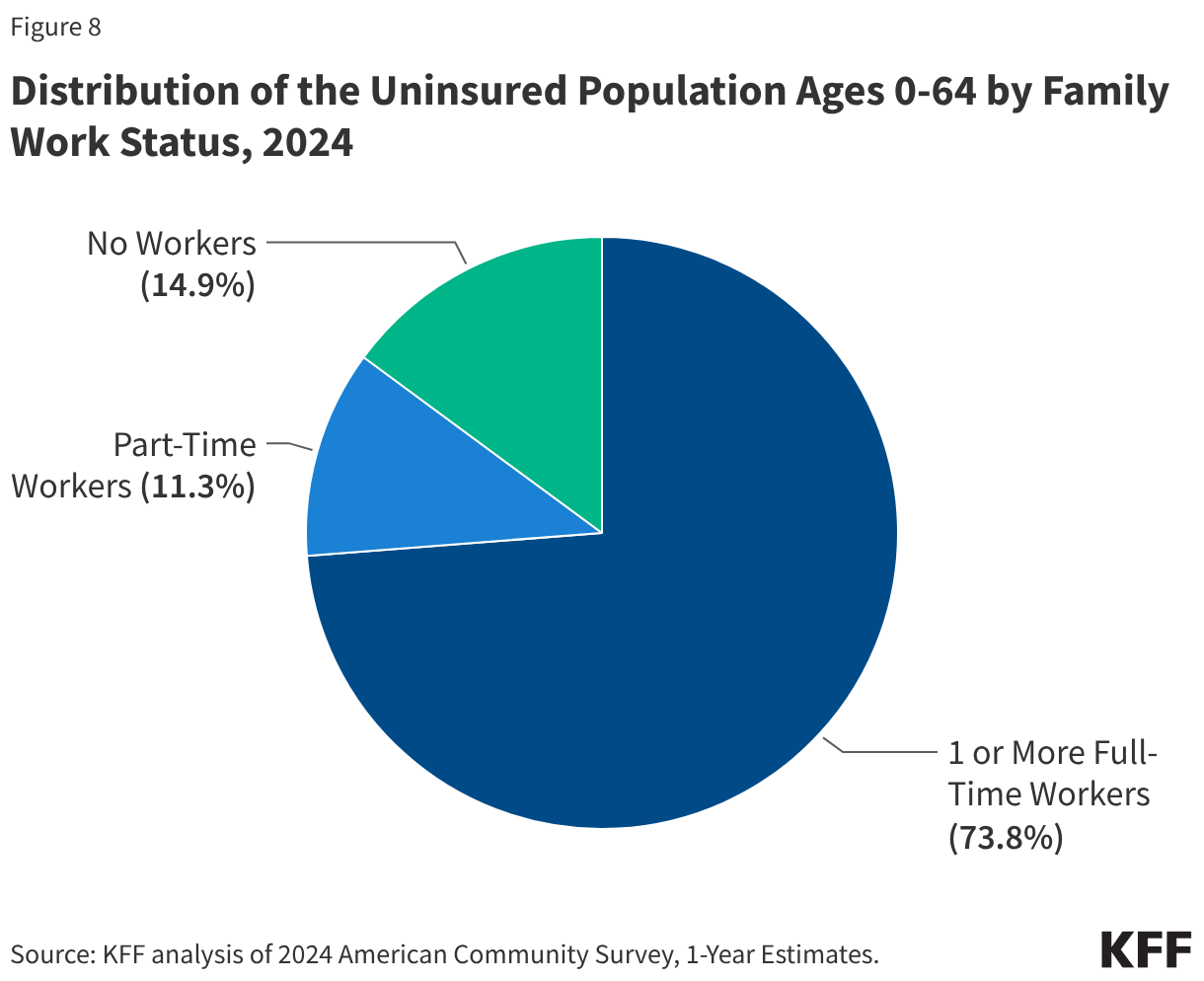
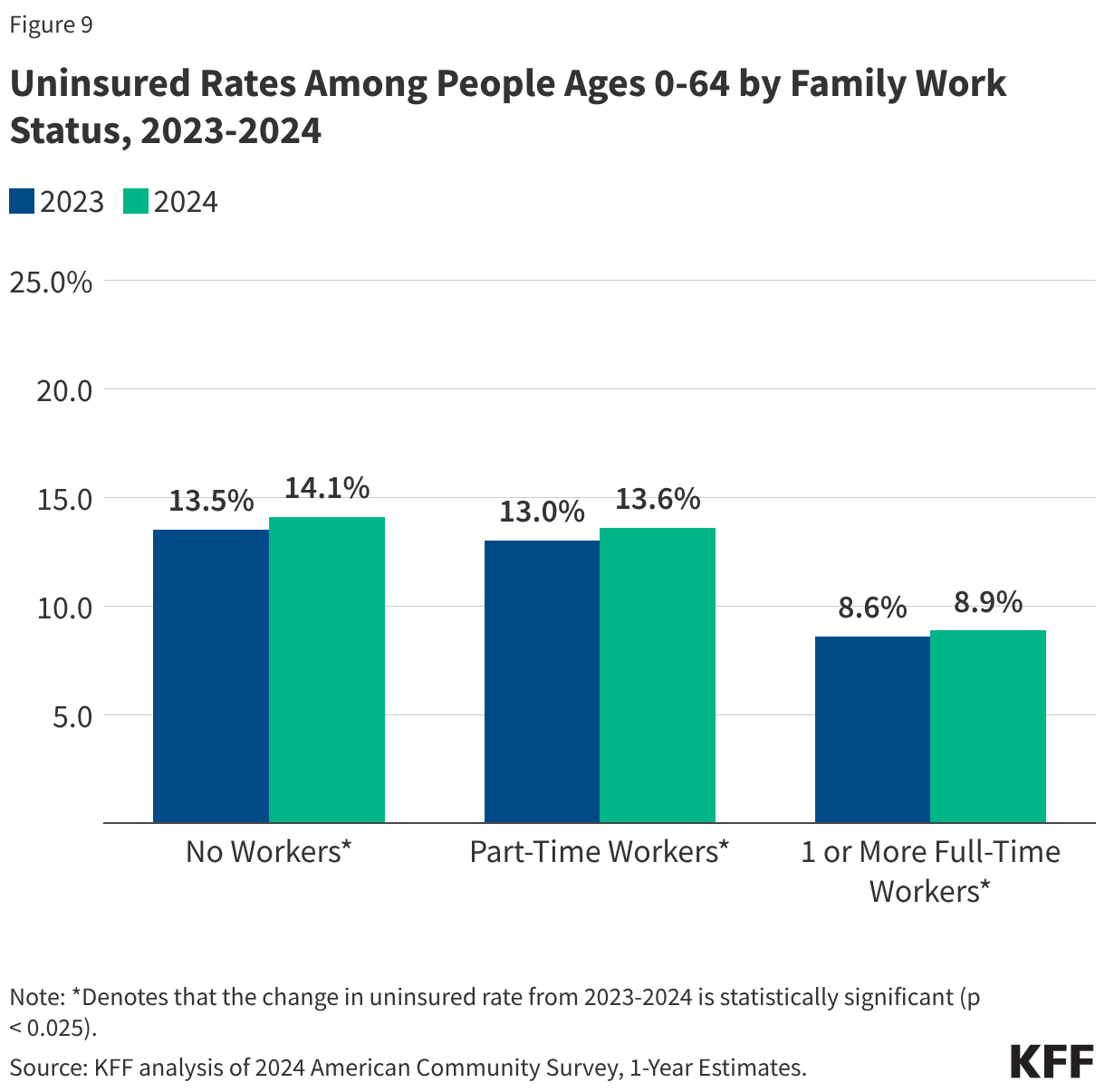
The 2024 data reveals that the burden of being uninsured is not distributed equally across the American population. The profile of the uninsured remains predominantly low-income and working-class. Over 80% of those without insurance in 2024 belonged to families with incomes below 400% of the federal poverty level (FPL), and 85.1% were in families with at least one worker.
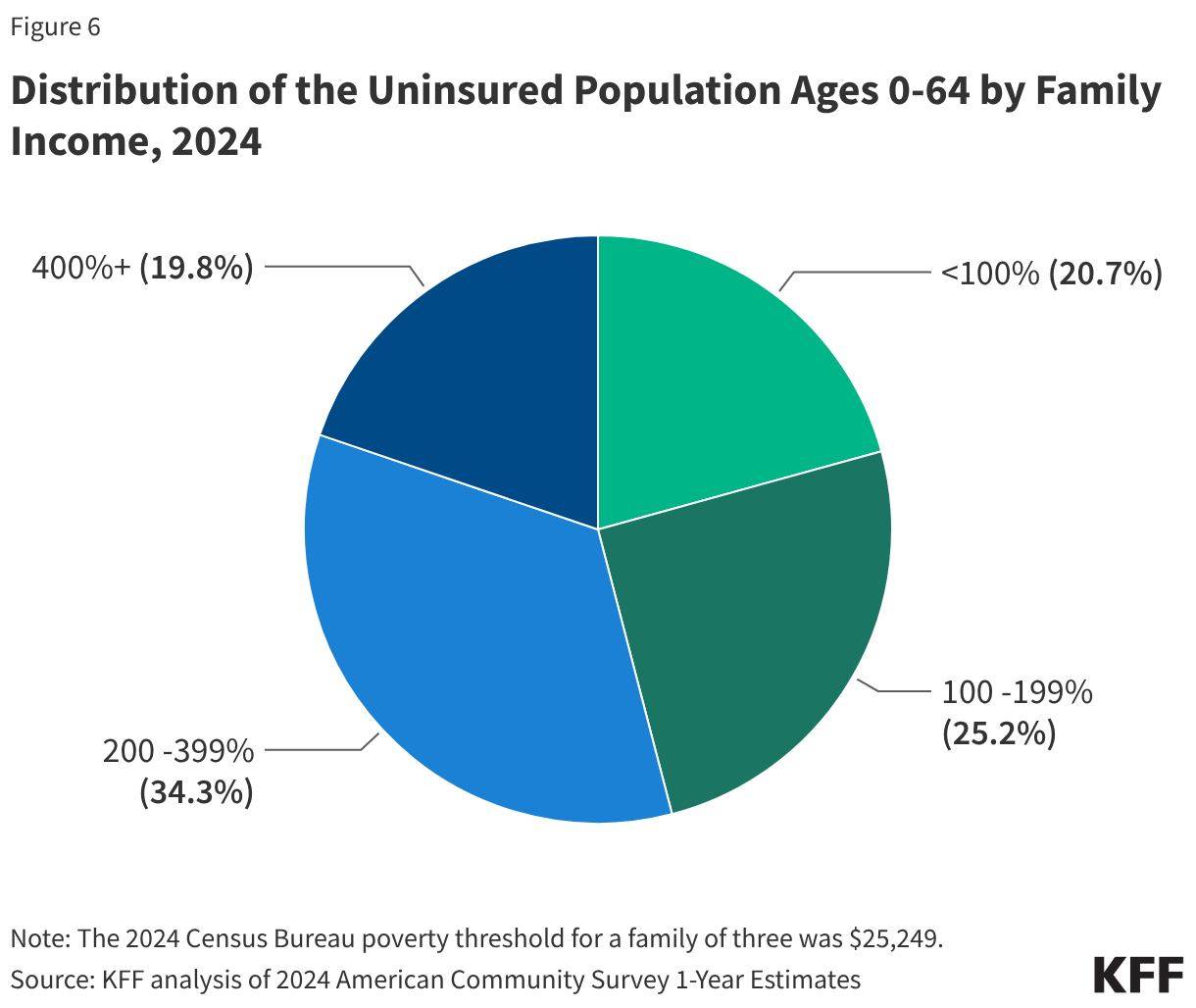
The Vulnerability of Children and Young Adults
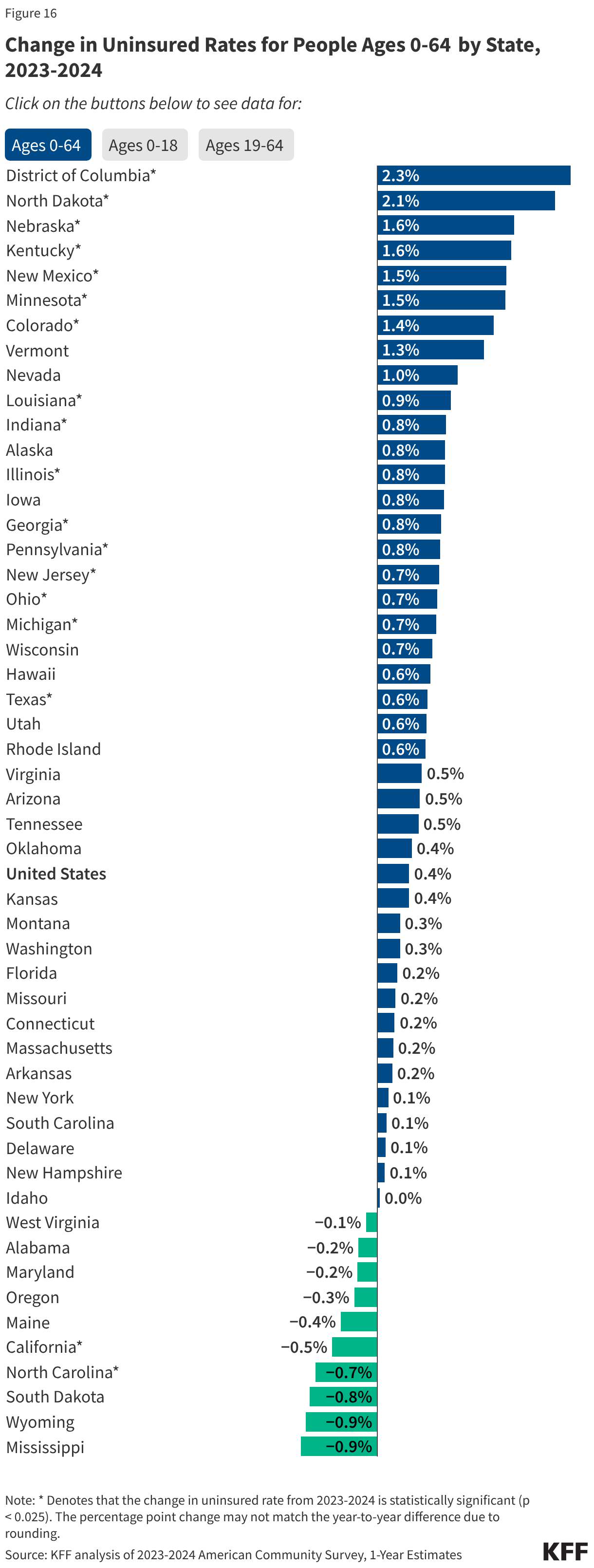
One of the most concerning findings from the 2024 report is the disproportionate impact on children. The uninsured rate for children ages 18 and younger rose from 5.3% in 2023 to 5.9% in 2024. This increase was sharper than the increase seen among adults, driven primarily by a steep drop in Medicaid coverage for minors. Young adults ages 19-25 also remain a high-risk group, with an uninsured rate of 14.5%, often due to aging out of parental plans or transitioning into entry-level jobs that lack robust benefits.
Racial and Ethnic Disparities
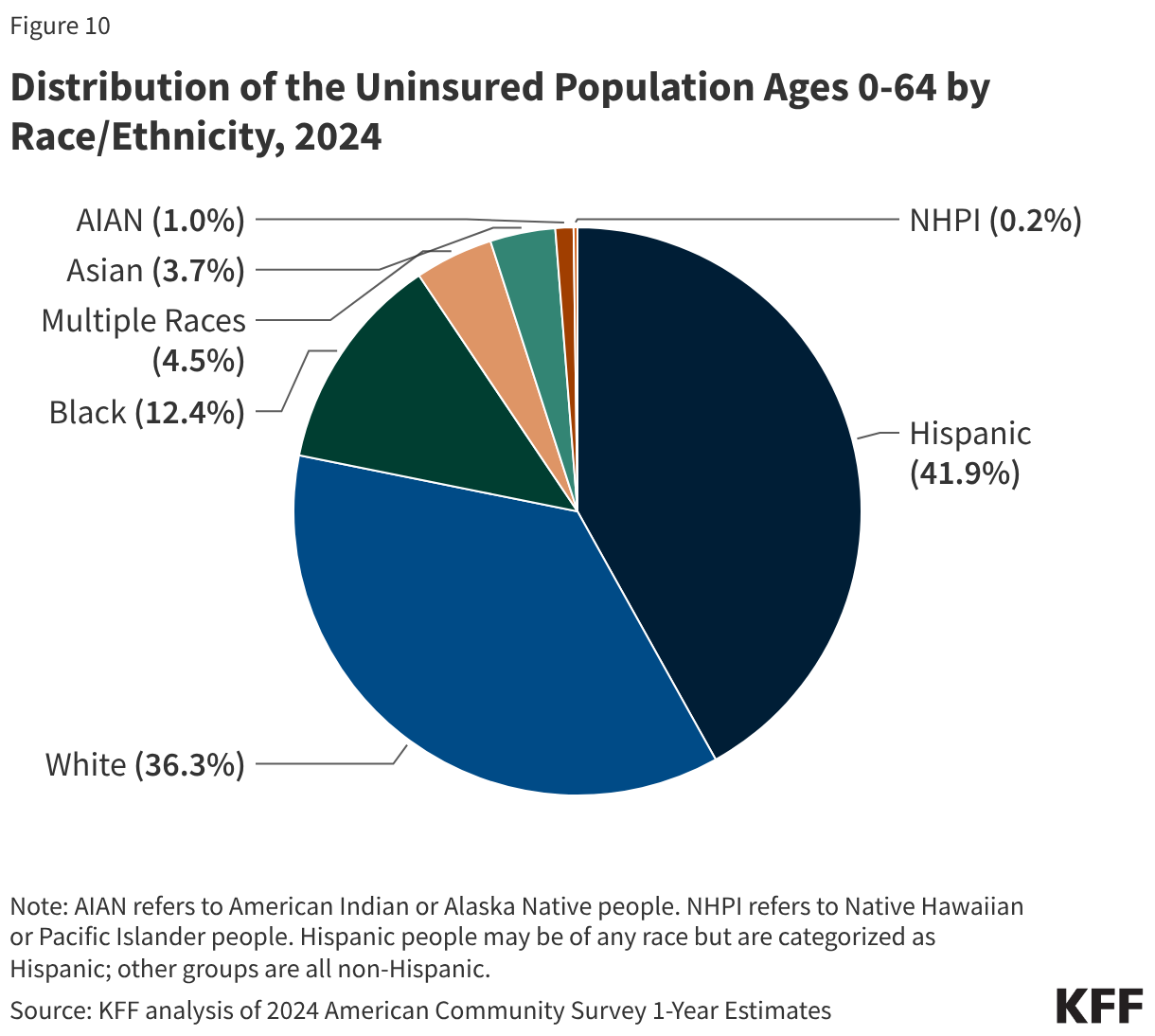
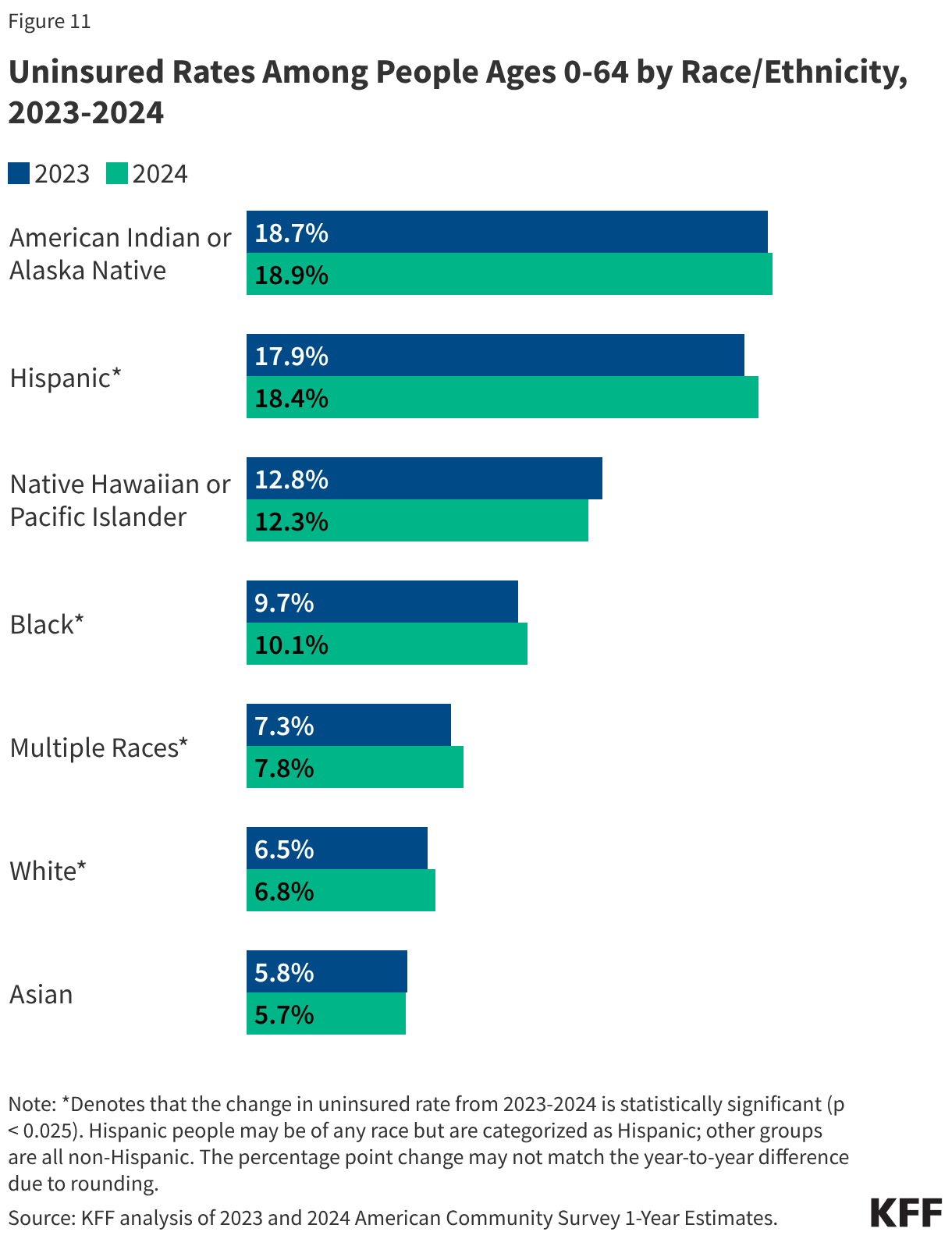
Health coverage remains a focal point of racial inequity in the United States. In 2024, nearly two-thirds of the uninsured population were people of color. Hispanic and American Indian/Alaska Native (AIAN) populations continue to face the highest risks, with uninsured rates of 18.4% and 18.9%, respectively—more than double the rate of White Americans (6.8%). Black Americans (10.1%) and Native Hawaiian/Pacific Islanders (12.3%) also experienced higher-than-average uninsured rates. While the ACA has narrowed these gaps over the last decade, the 2024 data suggests that the Medicaid unwinding has stalled or reversed progress in achieving health equity.
The Citizenship Gap
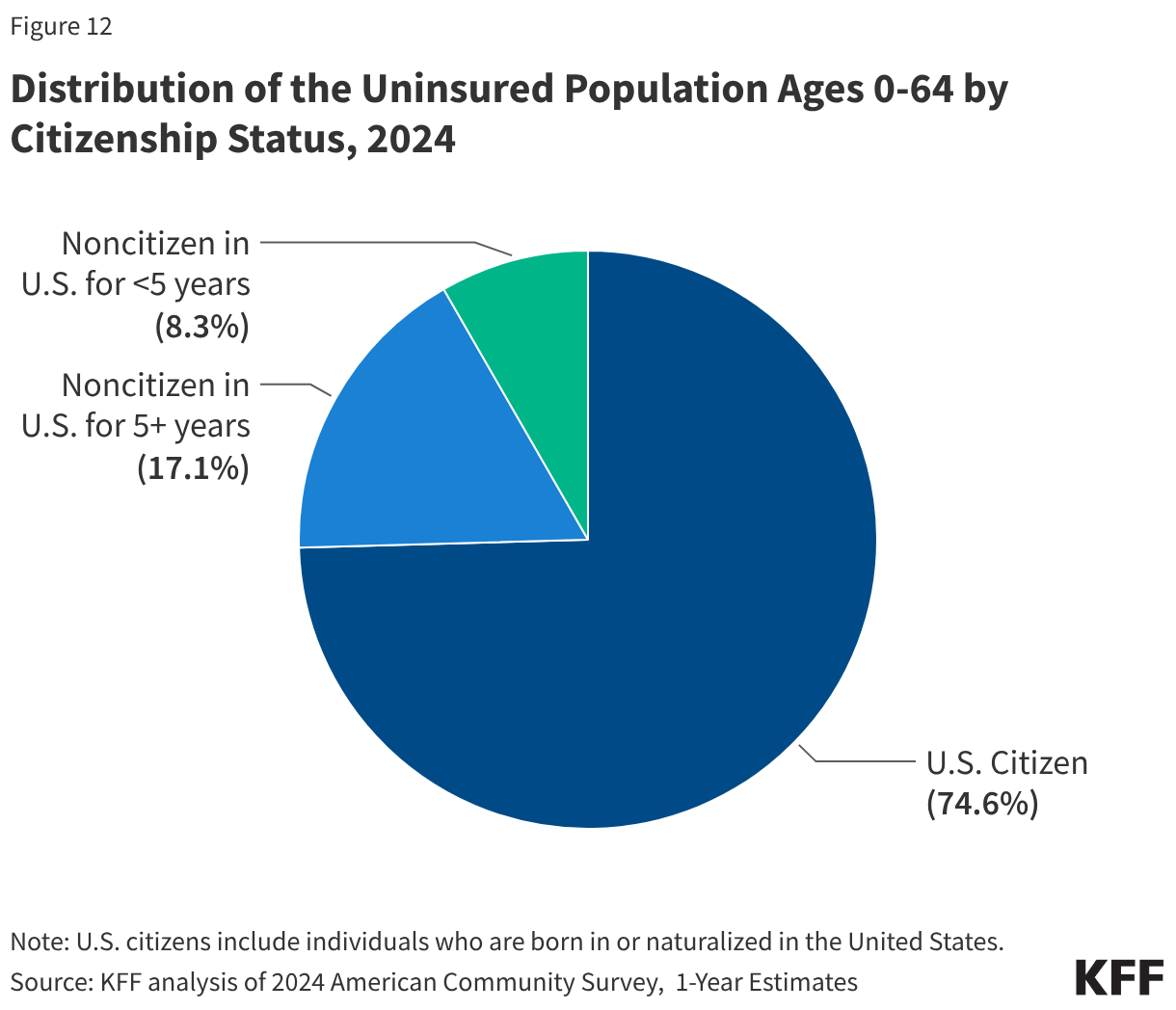
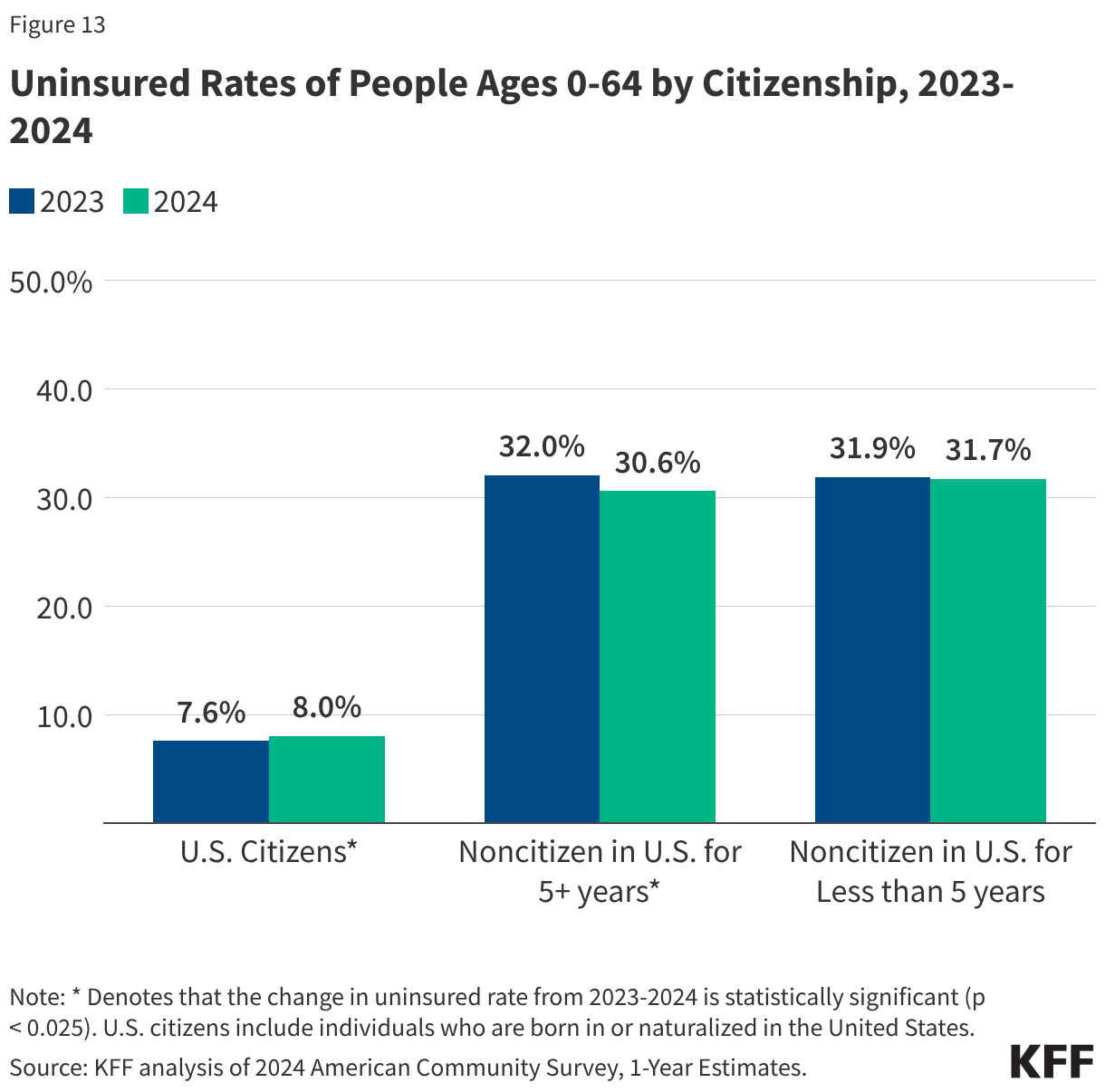
Citizenship status remains a primary determinant of insurance access. Noncitizens are more than 3.5 times as likely to be uninsured as U.S. citizens. In 2024, nearly one-third of all noncitizen immigrants lacked coverage. This is exacerbated by the "five-year bar," which prevents many lawfully present immigrants from accessing Medicaid, and a total lack of federal options for undocumented individuals. Policy analysts also point to a "chilling effect," where immigrant families avoid enrolling in public programs for which they are eligible due to fears regarding future immigration status or enforcement activities.
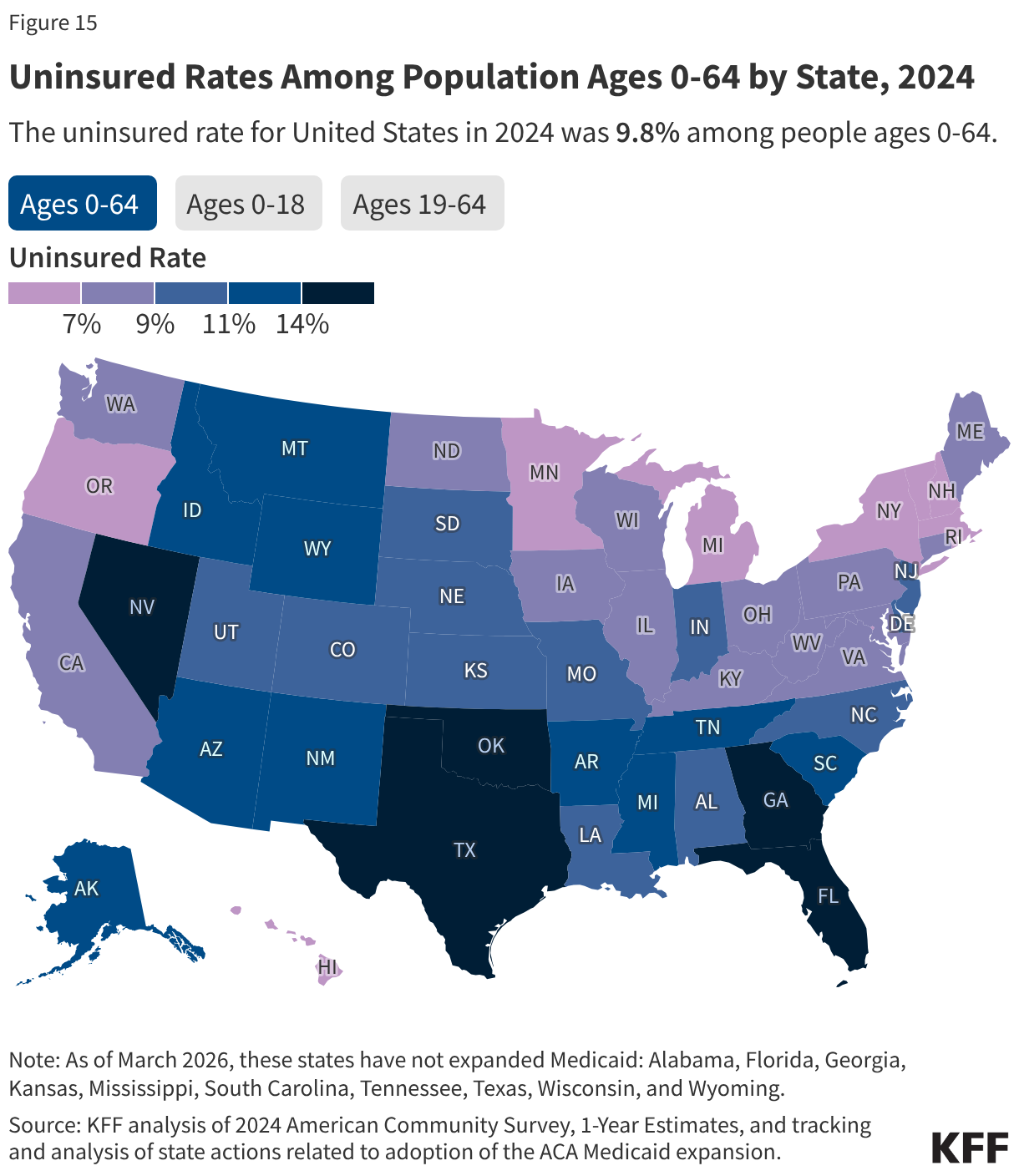
The Geographic Divide: Medicaid Expansion vs. Non-Expansion
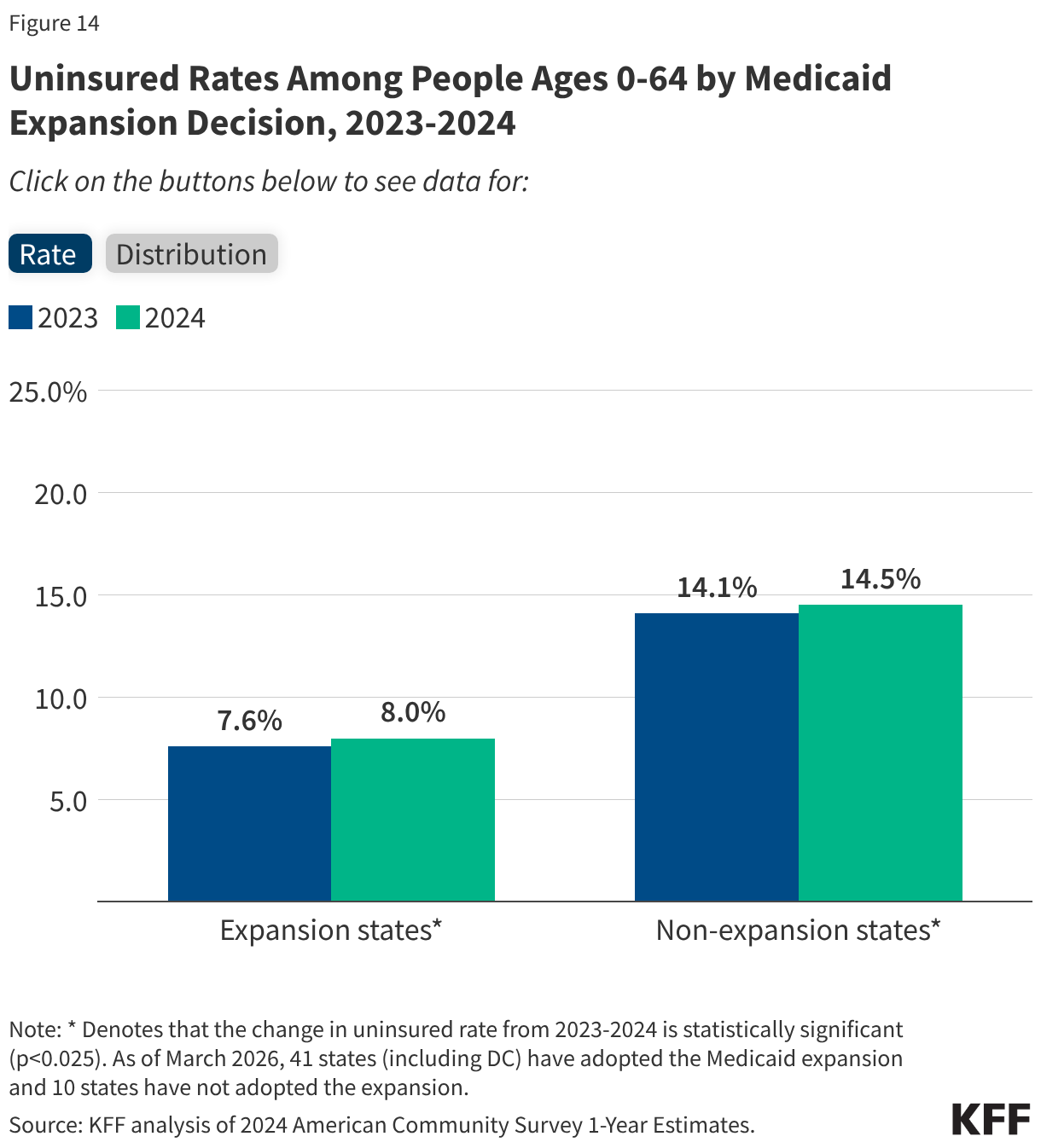
A person’s zip code remains one of the most accurate predictors of their insurance status. As of 2024, 41 states and the District of Columbia have expanded Medicaid to cover nearly all adults with incomes up to 138% of the FPL. However, the ten states that have not expanded Medicaid—including Texas, Florida, and Georgia—account for a staggering 42% of the nation’s uninsured population.
In these non-expansion states, the uninsured rate is 14.5%, nearly double the 8.0% rate seen in expansion states. In these regions, a "coverage gap" exists where individuals earn too much to qualify for traditional Medicaid but not enough to qualify for Marketplace subsidies. For example, Texas maintains the highest uninsured rate in the country at 19.2%, while Massachusetts, a state with robust state-level protections and expansion, sits at just 3.3%.
The High Cost of Being Uninsured: Medical and Financial Consequences
The lack of insurance is not merely a statistical concern; it has profound implications for public health and the financial stability of American households. Data from 2024 indicates that uninsured adults are twice as likely as those with insurance to delay or forgo medical care due to cost.
Barriers to Chronic Disease Management
The impact is particularly devastating for those with chronic conditions. Among adults with diabetes, more than 42% of the uninsured reported delaying or skipping necessary medical care because they could not afford it, compared to just 11% of those with insurance. Research consistently shows that gaining insurance leads to earlier diagnoses of cancer and cardiovascular issues, while the lack of coverage is associated with higher mortality rates. One recent study concluded that Medicaid expansion alone saved an estimated 27,000 lives between 2010 and 2022.
The Burden of Medical Debt
Financial distress is a hallmark of the uninsured experience. In 2024, 59% of uninsured adults reported having difficulty paying for healthcare costs. Furthermore, 62% of uninsured adults carry some form of healthcare-related debt. This debt often leads to a "domino effect" of financial instability, with uninsured individuals being more likely to overdraw checking accounts, rely on payday loans, or be contacted by debt collection agencies. Nearly 60% of uninsured adults stated they would be unable to find $2,000 for an emergency, compared to 39% of insured adults.
Policy Analysis and Future Implications
The outlook for the next decade suggests that the uninsured rate may continue to climb. Several key factors are expected to drive this trend:
- The 2025 Reconciliation Law: Legislative changes included in the 2025 reconciliation law are projected to alter Medicaid eligibility and impose stricter work requirements in some jurisdictions. The Congressional Budget Office (CBO) estimates that these changes, combined with other administrative actions, could lead to over 14 million additional people becoming uninsured by 2034.
- Expiration of Marketplace Subsidies: The enhanced premium tax credits first enacted under the American Rescue Plan Act (ARPA) and extended by the Inflation Reduction Act (IRA) are currently set to expire. If these subsidies are not renewed, Marketplace coverage will become unaffordable for millions of current enrollees, likely triggering a mass exodus from the private insurance market.
- Immigration Policy: Increased enforcement and more restrictive eligibility rules for immigrants are expected to further depress enrollment among lawfully present residents and their citizen children, worsening disparities in health outcomes.
Official Responses and Industry Reactions
Healthcare advocates and hospital associations have expressed growing concern over these trends. Safety-net providers, including community health centers and public hospitals, are bracing for a surge in uncompensated care. Data shows that charity care costs are significantly higher in states that have not expanded Medicaid, placing a heavy financial burden on local healthcare infrastructures.
Hospital administrators have noted that when patients lack insurance, they often delay care until their conditions become acute, leading to more expensive emergency room visits and poorer long-term outcomes. "The data from 2024 is a wake-up call," said one public health analyst. "We are seeing the direct result of removing the guardrails that kept the system stable during the pandemic. Without a renewed commitment to affordability and expansion, the progress made over the last decade is at risk of being completely erased."
Conclusion
The 2024 increase in the uninsured rate serves as a critical indicator of the fragility of the American healthcare system. While the ACA provided a foundation for coverage, the reliance on temporary pandemic protections and the ongoing political divide over Medicaid expansion have left millions of Americans vulnerable. As the "unwinding" concludes and new legislative challenges emerge, the nation faces a pivotal moment. The choices made by federal and state policymakers in the coming years will determine whether the 2024 uptick is a temporary setback or the beginning of a long-term decline in national health security. For the 26.7 million people currently without a safety net, the stakes could not be higher.