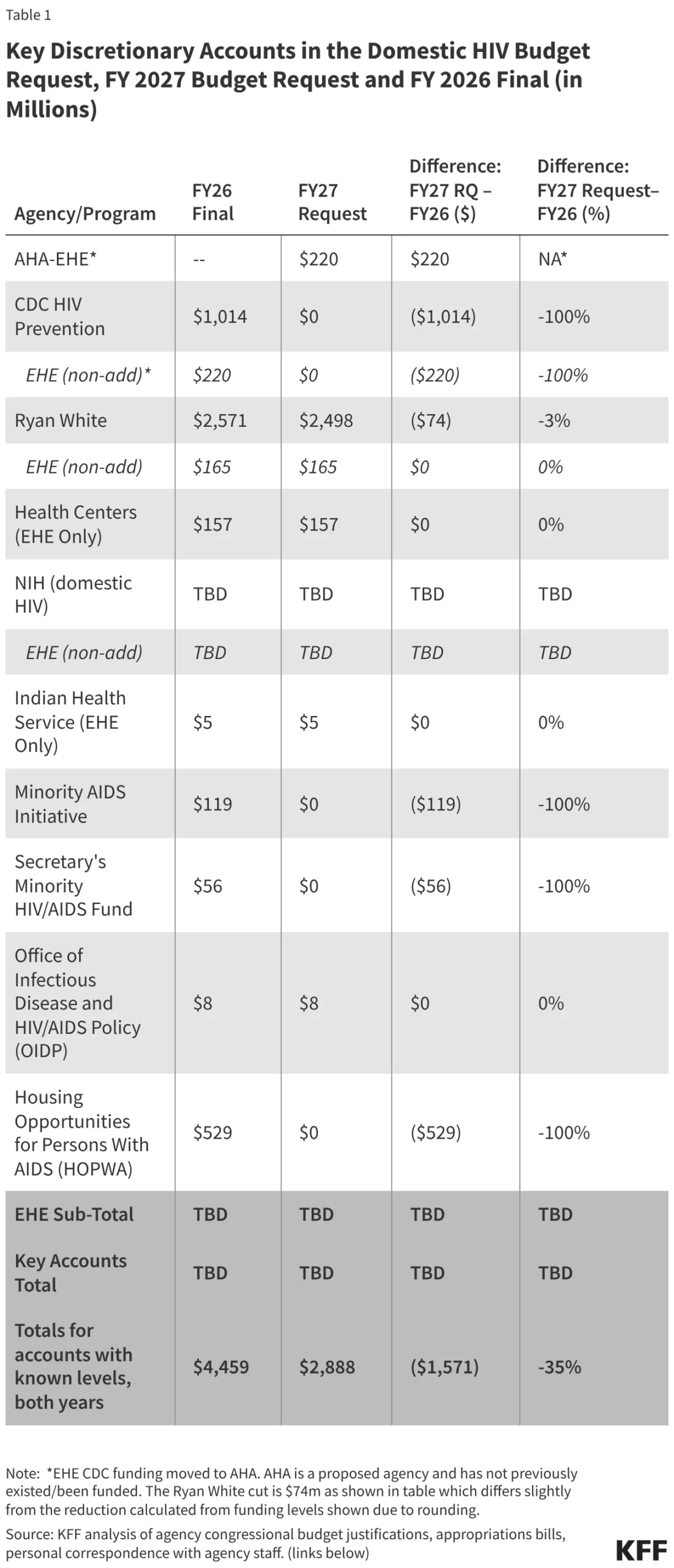
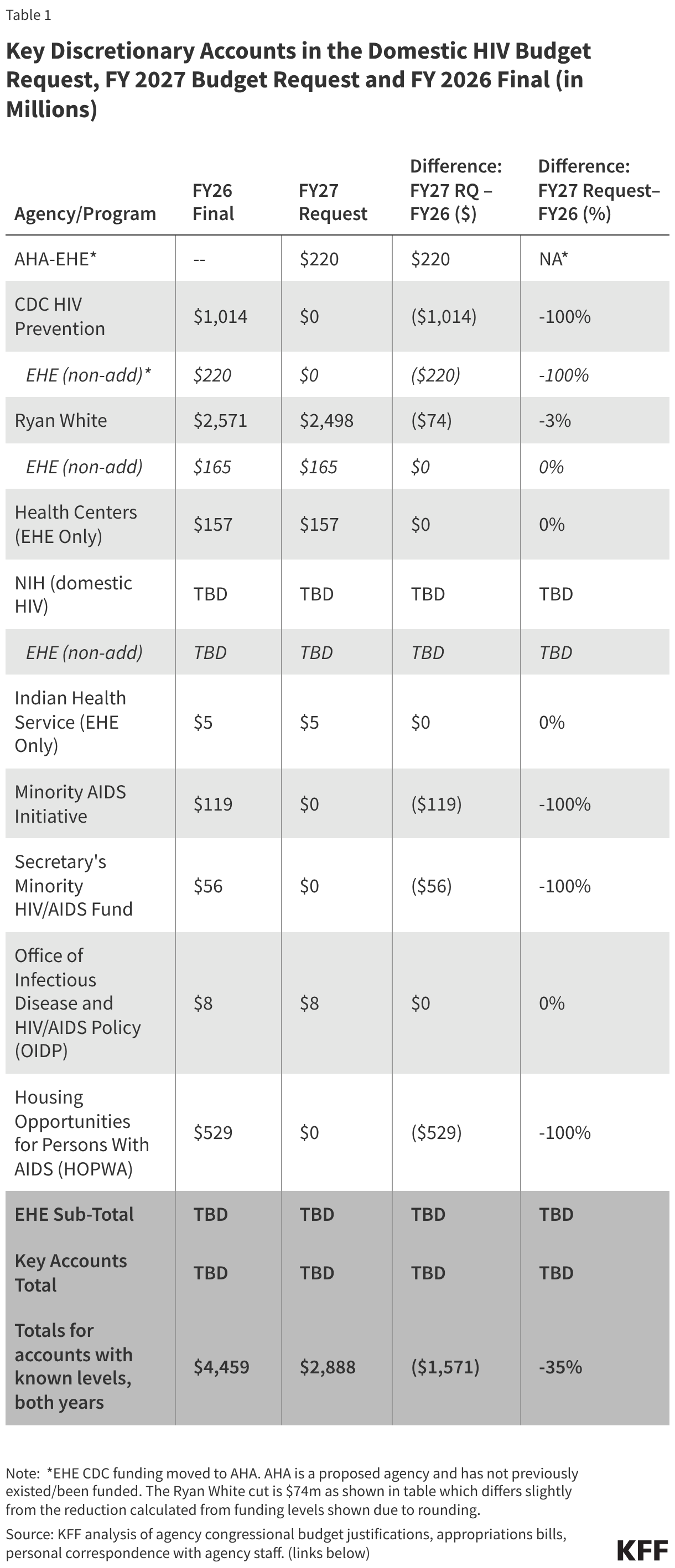
The Trump administration released its fiscal year (FY) 2027 budget request on April 3, 2026, outlining a federal spending plan that proposes a $1.6 billion reduction in funding for domestic HIV programs, representing a 35% decline from the previous year’s enacted levels. This budget, the second of President Trump’s second term, signals a fundamental shift in the federal government’s approach to the HIV epidemic, prioritizing the consolidation of programs under a new central agency while eliminating several long-standing pillars of prevention, research, and housing support.
While the budget request serves as a primary statement of the administration’s policy priorities, it remains subject to the "power of the purse" held by the U.S. Congress. In FY 2026, the administration proposed similar reductions, but Congress ultimately chose to maintain funding at levels consistent with prior years. However, the FY 2027 request doubles down on several controversial structural changes, including the creation of the Administration for Healthy America (AHA), a proposed agency intended to absorb many functions currently managed by the Health Resources and Services Administration (HRSA) and the Centers for Disease Control and Prevention (CDC).
Structural Reorganization and the Administration for Healthy America
Central to the administration’s FY 2027 proposal is the migration of several core HIV initiatives to the proposed Administration for Healthy America (AHA). This move, which was initially proposed and rejected by Congress in the FY 2026 cycle, aims to centralize the federal response to infectious diseases. According to the budget documents, the AHA would prioritize HIV/AIDS programs as part of a broader mandate to align public health efforts with the administration’s overarching health policy goals.
Under this plan, the Ryan White HIV/AIDS Program and the Health Center Program would be moved from HRSA to the AHA. Additionally, the Office of Infectious Disease and HIV/AIDS Policy (OIDP), currently housed within the Office of the Assistant Secretary for Health, would also be integrated into the new agency. This reorganization would also see the Ending the HIV Epidemic (EHE) initiative—a program launched during the first Trump administration in 2019—transferred from the CDC to the AHA.
Proponents of the reorganization argue that centralizing these programs will reduce bureaucratic overlap and improve efficiency. However, public health experts have expressed concern that the move could disrupt established relationships between federal agencies and local health departments, potentially stalling progress in regions where HIV transmission remains high.
Elimination of CDC Prevention and Safety Net Programs
The most significant fiscal reductions in the FY 2027 request are targeted at the CDC’s domestic HIV prevention efforts. The budget proposes the total elimination of core HIV prevention funding at the CDC, which has historically accounted for approximately 91% of all federal spending on domestic HIV prevention.

While the $220 million currently allocated to the CDC for EHE activities would be preserved, it would be moved to the AHA. This results in a net decrease of $794 million for the CDC’s HIV division—a 78% drop from FY 2026 levels. This reduction would effectively end federal support for several large-scale testing, surveillance, and outreach programs managed directly by the CDC.
Furthermore, the budget proposes the elimination of several other specialized programs:
- Housing Opportunities for Persons with AIDS (HOPWA): Funded at $529 million in FY 2026, this Department of Housing and Urban Development (HUD) program would be completely defunded. Since 1992, HOPWA has been the only federal program dedicated to the housing needs of low-income people living with HIV.
- Ryan White Part F: The budget calls for the elimination of Part F, which supports the AIDS Education and Training Centers (AETCs), the Special Projects of National Significance (SPNS), and dental programs. These programs are critical for training healthcare providers and developing innovative care models.
- Minority AIDS Initiative (MAI): Several components of the MAI, which addresses the disproportionate impact of HIV on racial and ethnic minority communities, face elimination. This includes $119 million previously allocated to the Substance Abuse and Mental Health Services Administration (SAMHSA) and $56 million from the Secretary’s Minority HIV/AIDS Fund.
Impact on Research and Innovation
The National Institutes of Health (NIH), the world’s leading funder of HIV research, is also facing substantial proposed cuts. The National Institute of Allergy and Infectious Diseases (NIAID), which manages the bulk of the NIH’s HIV research portfolio, would see its budget reduced by $1.8 billion, a 27% decrease from $6.5 billion to $4.8 billion.
While the specific allocation for domestic HIV research within this reduced NIAID budget has not been finalized, the scale of the cut suggests a significant retrenchment in the search for a cure and the development of next-generation treatments. In FY 2025, HIV research at the NIH was funded at approximately $3.3 billion. A reduction of this magnitude could impact clinical trials, vaccine research, and the development of long-acting antiretroviral therapies.
Notably, the FY 2027 request also continues to omit funding for a national Pre-Exposure Prophylaxis (PrEP) program, a cornerstone of the Biden administration’s HIV requests. The lack of federal investment in PrEP expansion, combined with the proposed cuts to prevention, suggests a shift in focus away from bio-medical prevention and toward a more centralized, treatment-focused model.
A Timeline of Recent Federal HIV Policy
The FY 2027 budget request arrives amidst a period of significant administrative and legislative tension regarding public health spending.
- February 2019: President Trump launches the "Ending the HIV Epidemic: A Plan for America" (EHE) initiative during the State of the Union address, aiming to reduce new infections by 90% by 2030.
- 2021–2024: The Biden administration expands the EHE initiative, emphasizing health equity and proposing a multi-billion dollar national PrEP program.
- January 2025: President Trump begins his second term; the administration begins utilizing executive actions to delay or rescind previously appropriated public health funds.
- June 2025: Significant layoffs at the CDC are reported following a rescission of public health funding, leading to litigation from several state attorneys general.
- March 2026: Congress passes the FY 2026 appropriations bill, largely ignoring the administration’s proposed HIV cuts and maintaining funding at prior-year levels.
- April 3, 2026: The FY 2027 budget request is released, renewing the proposal for the AHA and deeper cuts to the CDC and HUD.
Congressional Response and Administrative Maneuvers
The budget request is only one part of the administration’s strategy to reshape federal HIV spending. In recent months, the executive branch has employed "impoundment" tactics—delaying or canceling the distribution of funds already authorized by Congress. These actions have created a climate of "funding uncertainty" for state health departments and community-based organizations.
In some instances, these delays have led to legal challenges. For example, the Attorney General of California recently filed suit to protect over $600 million in health funding that the administration sought to rescind. While some grants have been reinstated following temporary restraining orders, the administrative friction has made long-term planning difficult for HIV service providers.
Legislative leaders have signaled that the FY 2027 request will face a difficult path in Congress. Members of the Appropriations Committees have historically viewed HIV funding as a bipartisan priority, particularly the Ryan White program and the EHE initiative. Critics of the budget argue that the proposed cuts would undo decades of progress, potentially leading to an increase in new infections and higher long-term healthcare costs.
Broad Implications for Public Health and Equity
The potential consequences of the FY 2027 budget extend beyond the balance sheet. Public health advocates warn that the elimination of HOPWA and CDC prevention funds could create a "perfect storm" for the resurgence of the epidemic.
Housing stability is widely recognized as a "social determinant of health" for people living with HIV. Research consistently shows that individuals with stable housing are more likely to achieve viral suppression, which not only keeps them healthy but also prevents the transmission of the virus to others (Undetectable = Untransmittable, or U=U). The elimination of HOPWA could jeopardize the health of thousands of low-income individuals, potentially increasing the burden on emergency rooms and the Medicaid system.
Furthermore, the cuts to the Minority AIDS Initiative come at a time when racial disparities in HIV outcomes remain a primary concern. African American and Latino communities continue to experience higher rates of new diagnoses and lower rates of viral suppression compared to their white counterparts. Advocates argue that removing targeted funding for these communities could exacerbate these inequities and stall the national goal of ending the epidemic.
As Congress begins its deliberations on the FY 2027 appropriations bills, the debate will likely center on the balance between fiscal consolidation and the maintenance of a robust public health infrastructure. For the millions of Americans living with or at risk for HIV, the outcome of this legislative process will determine the availability of life-saving care and the future trajectory of the epidemic in the United States.